Polymyositis and dermatomyositis are both medical conditions that belong to a group of myopathies. The former develops in the form of inflammation and subsequent degeneration of muscles while the latter is actually polymyositis accompanied by inflammation of the skin.
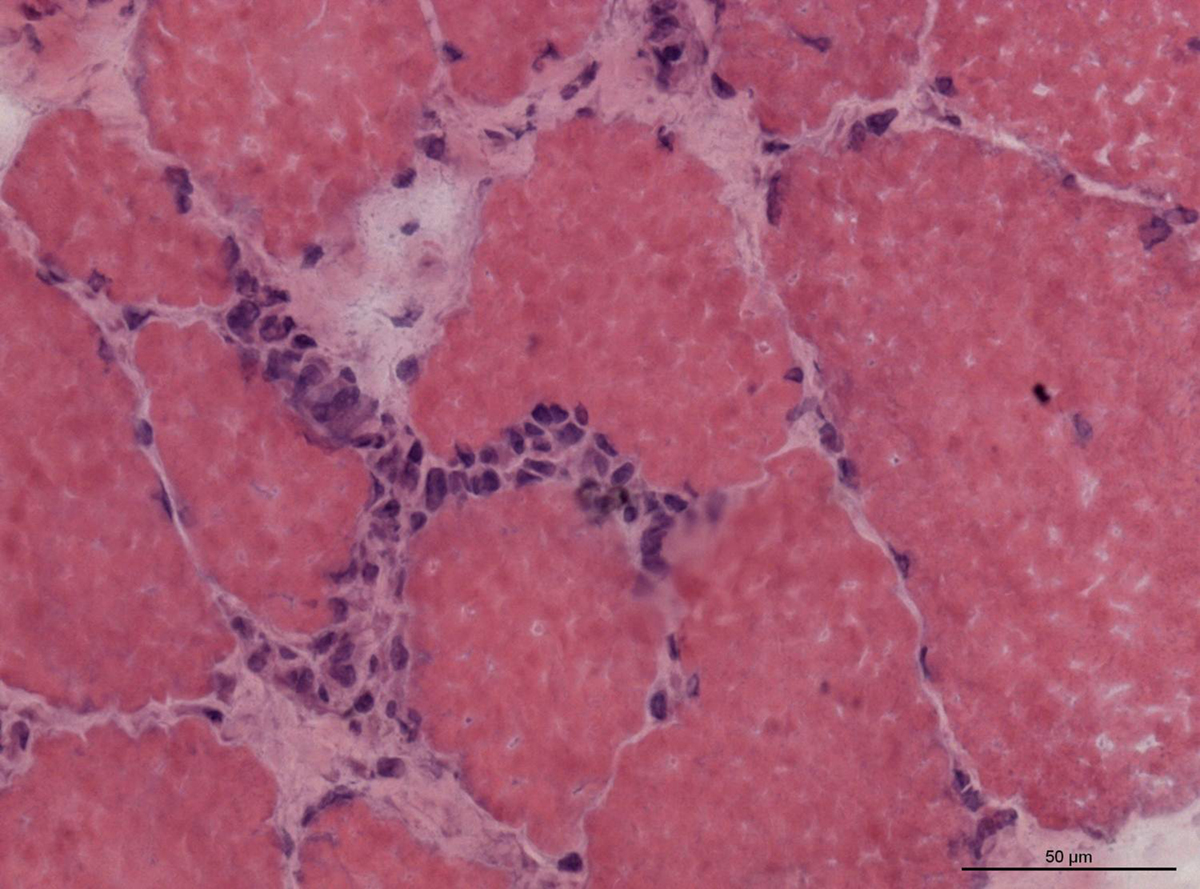
Both conditions are acquired primary diseases in which inflammation affects only the striated muscles and gradually triggers muscle weakness. Damage to the affected muscles is additionally accompanied by an increase of serum muscle enzymes.
Even though polymyositis and dermatomyositis are autoimmune illnesses and belong to a same group of diseases, they have rather unique clinical and histological features.
It is estimated that polymyositis and dermatomyositis predominantly affect people between 40 and 60 years of age and in children they commonly occur between 5 and 15 years of age. Both conditions affect women more and in adults they may develop together with other connective tissue disorders.
Muscle Weakness Caused by Inflammatory Myopathies
When it comes to pathophysiology, these two conditions are relatively similar.
Polymyositis (an immune mediated syndrome) develops as a consequence of defective cellular immunity and is commonly associated with other autoimmune diseases affecting the entire body. There are many different triggers of polymyositis. Viruses, malignant tumors, other connective tissue disorders and many more are all potential initiators of polymyositis. However, the condition may occur without any clear sign of any underlying disease or obvious trigger.
As for viruses, up until now scientists have managed to identify only several of these as potential triggers of polymyositis. They include human Retroviruses HIV and human T-cell lymphocytic virus type I (HTLV-I), the simian Retroviruses, and coxsackievirus B. These viruses cause direct damage to skeletal muscles and additionally increase the muscle susceptibility to further damage due to the condition.
Many times polymyositis develops at the same time as some viral infection. Patients usually complain about symmetrical muscle weakness that predominantly affects the upper arms, hips and thighs. Raynauds's syndrome is another characteristic of the disease. It is generally more frequent among young patients and is characterized by sudden pallor and tingling sensation in the fingers both of which develop as a consequence of exposure to cold or emotional stress. Additionally, there are joint aches and inflammation. The condition generally does not affect internal organs. If this occurs, it is highly likely that the heart or the lungs will be involved in the process of inflammation which subsequently leads to shortness of breath and cough.
In patients suffering from dermatomyositis there is an attack of the humoral immune response on muscle capillaries and small arterioles. The process of muscle inflammation also includes microangiopathy. Disease progression is blamed for destruction of capillaries and the muscles easily undergo the process of microinfarction. Finally, the affected muscles change in such a way that most of their healthy fibers are actually replaced with necrotic and degenerative tissue.
As far as symptoms and signs of dermatomyositis are concerned, they include all the symptoms of polymyositis along with symptoms and sign of skin inflammation. The skin is covered in a shadowy-red or even purplish rash. If it affects the face it may trigger swelling around the eyes. There is one more type of skin rash which is scaly, smooth and raised. It develops on other parts of the body, most commonly the knuckles and hands. After skin inflammation is brought under control, the affected skin undergoes pigmentation changes and there may be scarring as well.
Treatment for Polymyositis and Dermatomyositis
In mild cases of both polymyositis and dermatomyositis there is no need for treatment. Such individuals are due to use sun block agents on a regular basis, engage in physical activity to maintain muscle strength and if there are speech and languages difficulties or difficulty swallowing, patients work with a professional who will help them overcome the mentioned issues. These patients also have their creatine kinase levels measured and monitored.
Still, there are many patients who equally require treatment and whose symptoms and signs simply cannot be brought under control without efficient drugs. In order to prevent permanent muscle damage, medicamentous treatment must start on time. Similarly to other autoimmune diseases steroids are the cornerstone of polymyositis and dermatomyositis treatment. In mild cases these medications are used only topically while more complex cases require oral form of the drug. Patients may notice improvement 2-3 months after the onset of therapy. The major problem is the treatment that includes high doses of corticosteroids. These drugs have many side effects and it is best if the dose can be low, but efficient. In case higher doses are administered for a long period of time, such patients are monitored for side effects and may receive other drugs that prevent certain side effects from developing.
Other drugs that are prescribed to these patients include azathioprine, cyclophosphamide, methotrexate or high doses of intravenous immunoglobulin. It is also possible to treat these miopathies with antimalarial drugs and immunomodulatory drugs.
Finally, although the majority of patients respond well to treatment, many may end up with complications some of which are gastrointestinal ulcerations, subcutaneous calcification, ugly skin scars, cardiac abnormalities and interstitial lung disease.













Your thoughts on this
Loading...