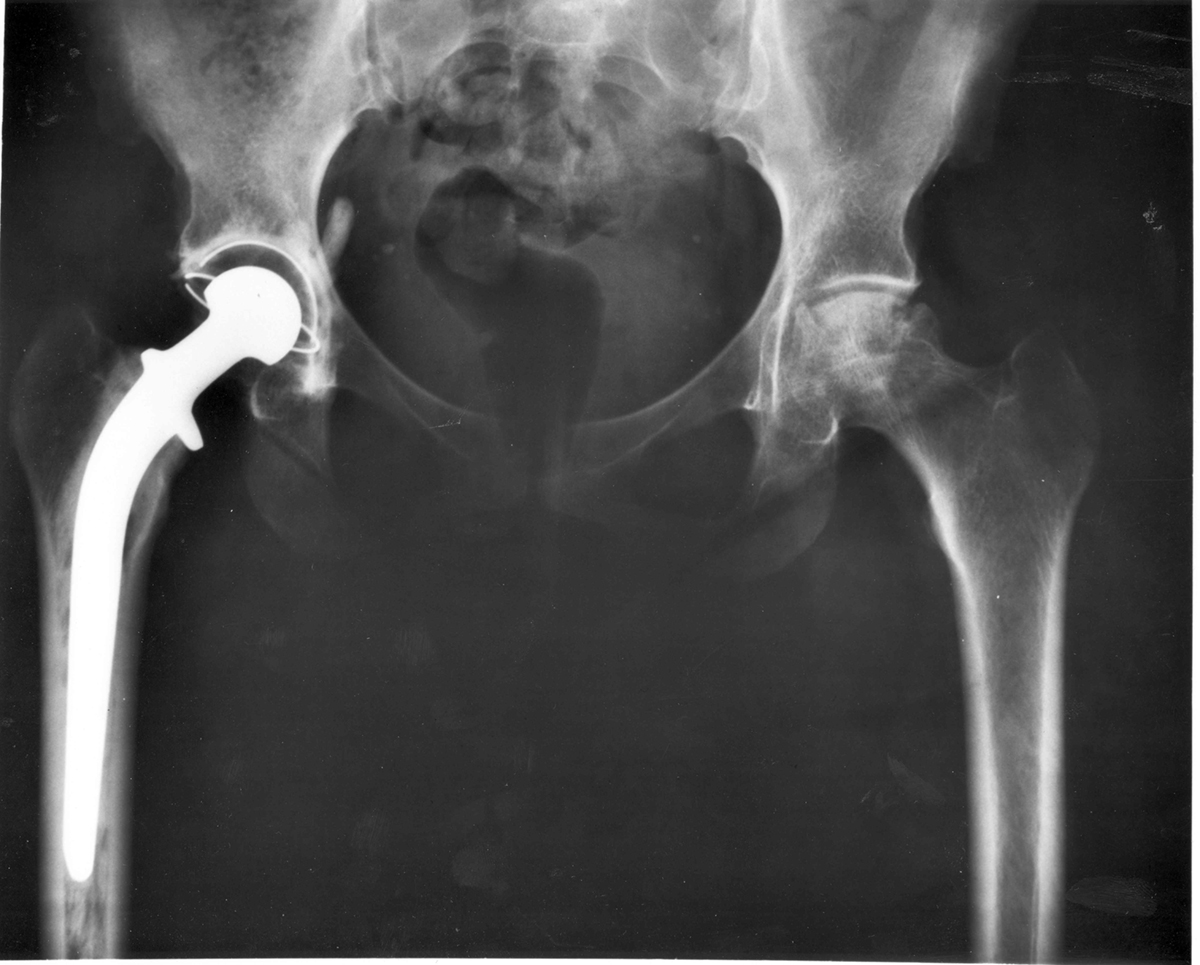
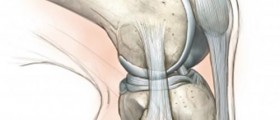
The hip joint (the acetabulofemoral joint) is the joint between the femur and the pelvis, to be more precise the acetabulum of the pelvis. The role of the joint is to provide with support regarding the body weight while standing and moving (e.g. running, walking etc.). Both hip joints are of major importance when it comes to retaining balance and any damage in the area results in various difficulties.
Total Hip Replacement Procedure
A total hip replacement procedure is an invasive surgical approach when the both damaged cartilage and parts of the bone that create the hip joint are replaced. The joint per se represents a ball and a socket. The socket is the acetabulum of the pelvis while the ball is the head of the femur. The surgery includes removal of the damaged ball and socket and their replacement with the artificial materials (prosthesis). Once the prosthesis is inserted in the desirable place it is sealed and fixed with methylmethacrylate. There are also prosthesis which are not additionally fixated and they allow cells from the remnant of the femur to grow inside the prosthesis eventually making it stable. The duration of so called 'cementless' prosthesis is much longer compared to standard prosthesis and, therefore, it is recommended more in younger patients.
Not all individuals suffering from damage to the hip joint will undergo total hip replacement. Doctors will recommend the surgery if all conservative treatments fail to help relieve symptoms of hip degeneration and prevent further damage to the joint. In the majority of cases osteoarthritis of the hip joint and its associated complications are indications for total hip replacement. Osteoarthritis is connected with the process of aging which explains why most patients are older individuals. Also, osteoarthritis affects children with congenital abnormality of the hip joint and may result from some injuries to the joint. Apart from osteoarthritis, other conditions such as hip fracture, rheumatic arthritis, aseptic necrosis of the hip bone etc. are reasons why patients undergo total hip replacement.
The damaged hip is to blame for chronic pain and difficulties walking, climbing stairs and similar. The disability of this type can be improved with the surgery.
Unfortunately, even when the damaged joint is replaced with prosthesis, there is a risk of treatment failure. This is why is is essential to compare the benefits and risks and recommend surgery only if its benefits exceed the potential complications.
How is Total Hip Replacement Done?
When it comes to preparation for the surgery, it basically comprises pre-operative exams and tests, donation of blood by the very patients which is used for transfusion during the surgery and evaluation of all the comorbidities. Some medications patients use on a regular basis might be discontinued at some point prior to the surgery. This particularly refers to Aspirin. Aspirin is a potent anticoagulant. If one takes it without interruption before the surgery, he/she exposes him/herself to increased risk of excessive bleeding. And finally, before total hip replacement all patients undergo routine evaluation of blood counts, electrolytes, blood tests assessing the kidney and liver function, chest X-ray and electrocardiography.
The surgery is relative long, lasting between 2 and 4 hours. There are additional few hours necessary for preparation. The surgeon chooses among several techniques. The posterior approach includes incisions on the back when the joint is reached via the piriformis muscle and the short external rotators of the femur. This approach is very efficient and prevents certain complications, abductor dysfunction in particular.
Furthermore, the lateral approach is another frequently used technique. In includes manipulation with the hip abductors which are either lifted or divided. The lateral approach carries less risk of dislocation compared to the posterior approach but it is associated more with healing problems affecting the abductor muscles.
The antero-lateral approach allows surgeons to reach the joint and perform the replacement through the space between the tensor fasciae latae and the gluteus medius.
And finally, the anterior approach includes separation of the sartorius muscle and tensor fascia latae.
After the surgery patients are transferred into a recovery room where they spend some time being observed. Once the operated individuals are stabilized they return to a hospital room. Initially, all of them receive fluids and medications through an intravenous line. The dressing applied during the surgery will stay on for a couple of days and is then changed. Pain-killers relive pain which is sometimes intense.
One of the measures which are routinely employed is prevention of blood clot formation in the lower extremities. Namely, these patients are practically immobile which contributes to blood clotting and thrombus formation. Compressing stockings may force the blood from the lower limbs to circulate. Also, some individuals receive blood thinners.
Those having problems with urination are temporarily inserted urinary catheters.
And finally, as soon as patients become capable they engage in rehabilitation programme which will help them recuperate and start using the operated leg once again.








Your thoughts on this
Loading...