If your gynecologist scheduled you a colposcopy, you might not be sure what this procedure is about. However, you should not be nervous since colposcopy is, on most occasions, just a part of a regular check-up.
On the other hand, this procedure can be used for the purpose of examination of abnormalities noticed in the results of Pap smear, a process in which samples of secretions and superficial cells of the cervix and uterus are collected and examined in the laboratory.
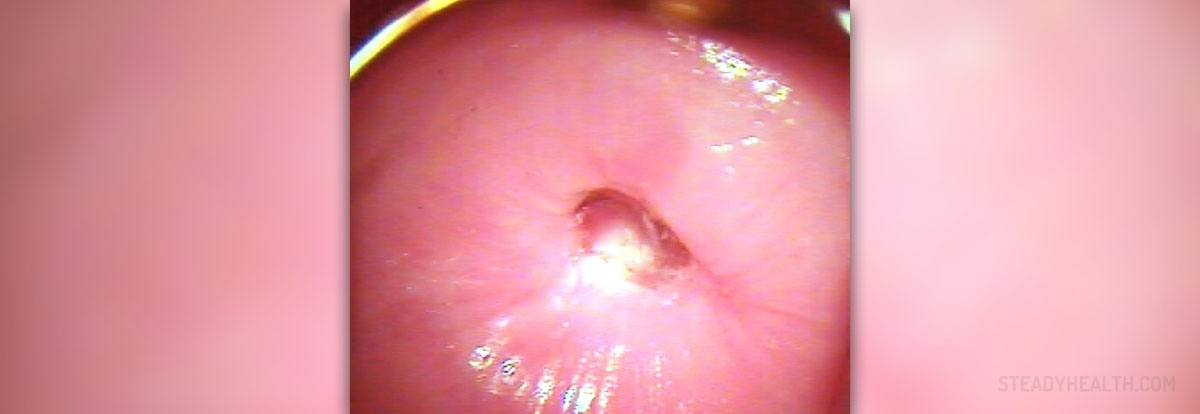
If the results suggest abnormalities, doctors usually recommend performing colposcopy, which determines the factors that caused abnormal findings of Pap smear. Colposcopy enables closer observation of the cervix, which is an opening from the vagina to the uterus.Colposcopy for Regular Check-Up
As it was mentioned above, colposcopy is usually done after the Pap smear findings have suggested conditions such as cervical dysplasia, cancer, presence of human papillomavirus, or ASCUS, which means atypical squamous cells of undetermined significance.
This procedure is usually done in less than 15 minutes. It is painless and performed in the gynecologist’s office. Like in Pap smear, it is done with the patient positioned on the examination table or chair. After inserting the vaginal speculum, the doctor will smear diluted vinegar onto the cervix and use an instrument called colposcope to examine the cervix. Diluted vinegar is used because it turns abnormal cells white.
In case any abnormalities are observed, the next step is to apply iodine, which allows an even closer and better look and dyes the abnormal cells brown. Sometimes the doctor takes a small sample of the tissue and sends it to the lab, through a process called a biopsy.
Colposcopy is generally considered a safe procedure and in most cases it does not cause any significant complications. However, some temporary side effects are always possible.
Side effects usually occur if the doctor has performed a biopsy along with colposcopy. In this case the patient may experience some cramping once local anesthesia wears off. The cramps are usually similar to those characteristic for the monthly period.
Colposcopy sometimes causes mild vaginal discharge and minor bleeding, usually in form of spotting. For this reason the patients are often advised to carry a sanitary pad with them and to use it after the procedure. The discharge and the bleeding should stop within a few weeks.
In rare cases, there may be some significant bleeding after the procedure. Additionally, colposcopy can cause a menstrual flow that is heavier than usual.
Finally, keep in mind that an infection of the biopsy site is rare but possible and it includes symptoms like fever, foul-smelling discharge, pain and heavy bleeding.
Sacrocolpopexy is a More Invasive Procedure
Sacrocolpopexy is an invasive surgical procedure that is most frequently used in the treatment of women with vaginal or uterine prolapse. This condition happens when muscles or the tissue that are supposed to hold the pelvis in certain position are weakened either due to the child birth, age, straining physical activity, or gaining the weight.
Predominantly, the consequences of this condition are related to urinary incontinence. Yet, they can also trigger problems with bowel movement, along with painful intercourse and sexual dysfunction.
However not all the women with these problems are adequate candidates. During sacrocolpopexy, vaginal vault prolapse will be corrected surgically by stitching the top of vagina or the cervix to the sacrum (tail bone), either with permanent stitches or with the help of a mesh, which will have to hold the vagina in its natural position.
It used to be commonly performed as an open surgery, done under general anesthesia and by a gynecologist, and the traditional approach requires a very long incision in the lower part of the abdomen. However, a newer and somewhat simpler procedure, called da Vinci sacrocolpopexy is also available now and it is minimally invasive, requiring very small incisions. In comparison to the traditional approach it has numerous benefits but the doctor is the one who decides which patient is a suitable candidate for it.
The most typical complications related to this procedure include pain, discomfort, infections, bleeding, blood clots and an adverse reaction to anesthetics. Rectum or bladder wall perforation, or pain during intercourse may also be experienced after the procedure.
Finally, since this is a very complicated surgery, in cases in which the mesh is used, it is possible that it comes out through the vagina, or that the urethra will be damaged, but this possibility is usually checked when the procedure is over. However, if everything goes well, as according to the statistics does in more than 90 % of cases the patient will have to stay in the hospital for 5 days while after 2 weeks she will be able to go back slowly to everyday activities.
To sum up, both colposcopy and sacrocolpopexy are procedures carried out by gynecologists. The difference between the two lie in the fact that coposcopy is commonly carried out during regular check-ups while the sacrocolpopexy is necessary in cases of vaginal vault prolapse. Thus, the latter is considered to be a much more serious procedure.



_f_280x120.jpg)





Your thoughts on this
Loading...