What is Acid Reflux Surgery?
Surgery for acid reflux disease is invasive procedure with one goal-reduction of damage to the esophagus caused by excess of stomach acid. This type of surgery is not commonly performed and is reserved only for severe cases of the disease. In case the patient responds suitably to medications there is no need for him/ her to be operated.
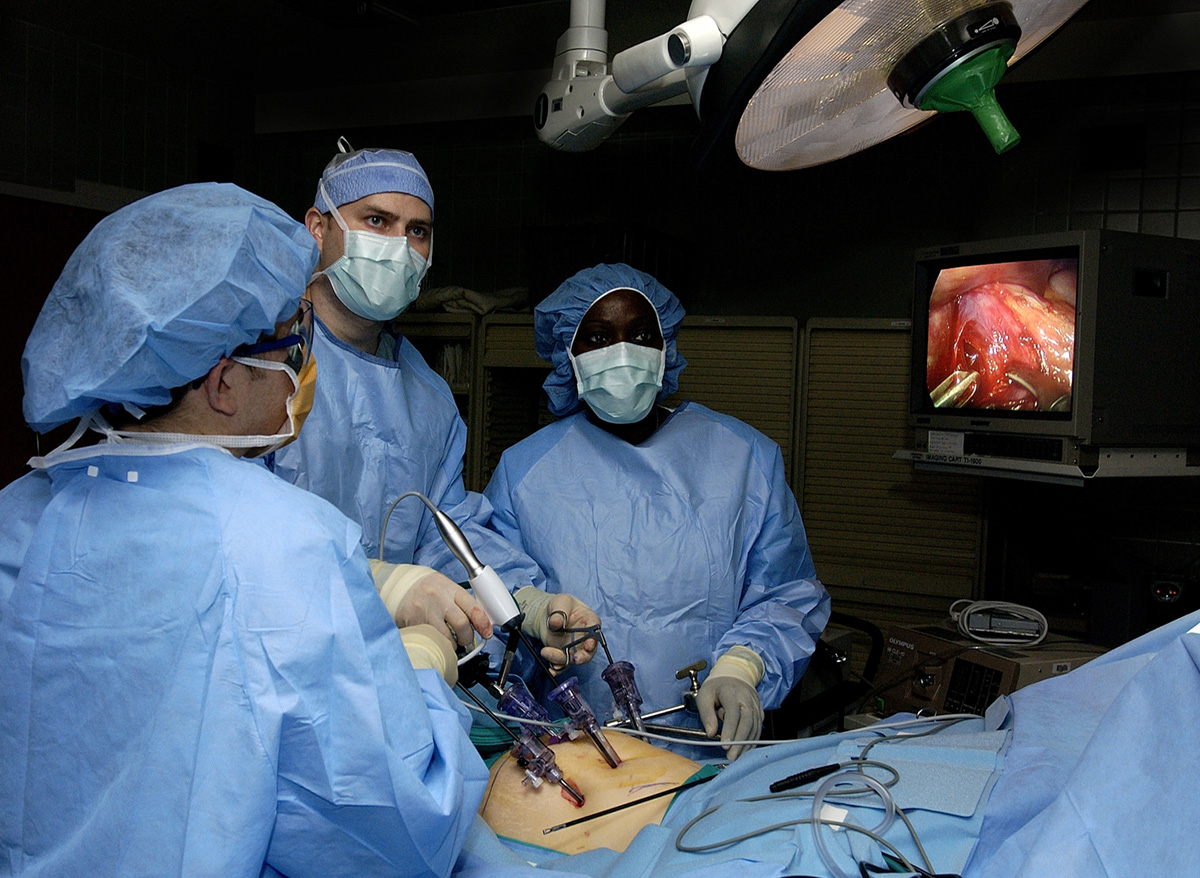
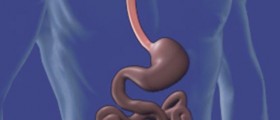
Nissen fundoplication is the standard surgery for acid reflux disease. The entire procedure is most commonly performed laparoscopically. This makes the surgery minimally invasive. In some cases the surgery is performed in a form of traditional open surgery. The procedure includes wrapping of the parts of the stomach around the lower esophagus. This way the natural valve between the stomach and the esophagus is strengthen and the acid simply does not enter the esophagus any more. Hence, the damage to the esophagus is eliminated and damaged mucous membrane gets the chance to recover.
What are Dangers and Risks of Acid Reflux Surgery?
As it is the case with any other surgery even surgery for acid reflux carries certain risks.
In many cases patients have to deal with nausea, abdominal cramping, gas bloating syndrome and swallowing problems. These complications are generally not permanent and tend to withdraw in time.
Furthermore, some more serious complications include dumping syndrome, excessive scarring and in rare cases achalasia. There is also a chance of surgery failure when patients start to experience the same symptoms and signs of the disease even though they have been surgically treated.
Gas bloat syndrome is one of the potential complications of Nissen fundoplication. Patients suffering from this complication complain about belching due to gas accumulation in the stomach and small intestine. This complication affects approximately 2-5% of all patients and it generally withdraws within 2-5 weeks. In some cases the problem may persist. In case the condition persists in spite of dietary restrictions and counseling regarding aerophagia (swallowing of air that may be responsible for gas bloat syndrome) a person may need to undergo an endoscopic balloon dilatation.
During the very procedure the operated area is inflated with gas. The very presence of the gas together with psychological and physical trauma associated with the operation may lead to postoperative irritable bowel syndrome. This complication generally features with initial constipation and later diarrhea and gas expulsion.
One more side effect of the surgery is difficulty or even impossibility of one to vomit once he/ she has been operated. The problem is evident initially, but small amounts of vomit may be produced after the wrap settles over time. It is essential to restore one's ability to vomit since this defensive activity is essential in certain circumstances such as alcohol or food poisoning.
Nationwide population-based retrospective cohort study in Sweden between January 1, 2005, and December 31, 2014, based on all Swedish health care and including 2655 patients who underwent laparoscopic antireflux surgery according to the Swedish Patient Registry. Their records were linked to the Swedish Causes of Death Registry and Prescribed Drug Registry. The findings were as following:
- Among all 2655 patients who underwent antireflux surgery (median age, 51.0 years; interquartile range, 40.0-61.0 years; 1354 men [51.0%]) and were followed up for a median of 5.6 years, 470 patients (17.7%) had reflux recurrence; 393 (83.6%) received long-term antireflux medication and 77 (16.4%) underwent secondary antireflux surgery. Risk factors for reflux recurrence included female sex (hazard ratio [HR], 1.57 [95% CI, 1.29-1.90]; 286 of 1301 women [22.0%] and 184 of 1354 men [13.6%] had recurrence of reflux), older age (HR, 1.41 [95% CI, 1.10-1.81] for age ?61 years compared with ?45 years; recurrence among 156 of 715 patients and 133 of 989 patients, respectively), and comorbidity (HR, 1.36 [95% CI, 1.13-1.65] for Charlson comorbidity index score ?1 compared with 0; recurrence among 180 of 804 patients and 290 of 1851 patients, respectively).
- Hospital volume of antireflux surgery was not associated with risk of reflux recurrence (HR, 1.09 [95% CI, 0.77-1.53] for hospital volume ?24 surgeries compared with ?76 surgeries; recurrence among 38 of 266 patients [14.3%] and 271 of 1526 patients [17.8%], respectively).
- Secondary antireflux surgery included both open and laparoscopic fundoplication. Follow-up time started at the date of surgery and ended at onset of recurrence of reflux as defined by the last dispensing of medication reaching a cumulative treatment time of 6 months, secondary antireflux surgery, death, or December 31, 2014, whichever occurred first. Furthermore, patients receiving any prescribed proton pump inhibitor or histamine2 receptor antagonist, regardless of duration, were identified for descriptive purposes.
- Defined procedure-related acute complications occurring within 30 days of primary laparoscopic fundoplication or repeated surgery with laparoscopic or open fundoplication were assessed from the Patient Registry. These complications included pneumothorax, esophageal perforation, splenic injury, liver injury, and other specifically surgery-associated complications.
- In all, 109 patients (4.1%) had a defined complication within 30 days of the primary laparoscopic antireflux surgery, and the most common complications were infection (n?=?28; 1.1%), bleeding (n?=?24; 0.9%), and esophageal perforation (n?=?24; 0.9%). The 30-day all-cause mortality rate was 0.1% (n?=?2 patients, 1 because of inhalation of a foreign body and 1 because of suicide). During the entire postoperative follow-up, 21 patients (0.8%) received a diagnosis of dysphagia at any time, including 14 (0.5%) also requiring endoscopic dilatation.













Your thoughts on this
Loading...