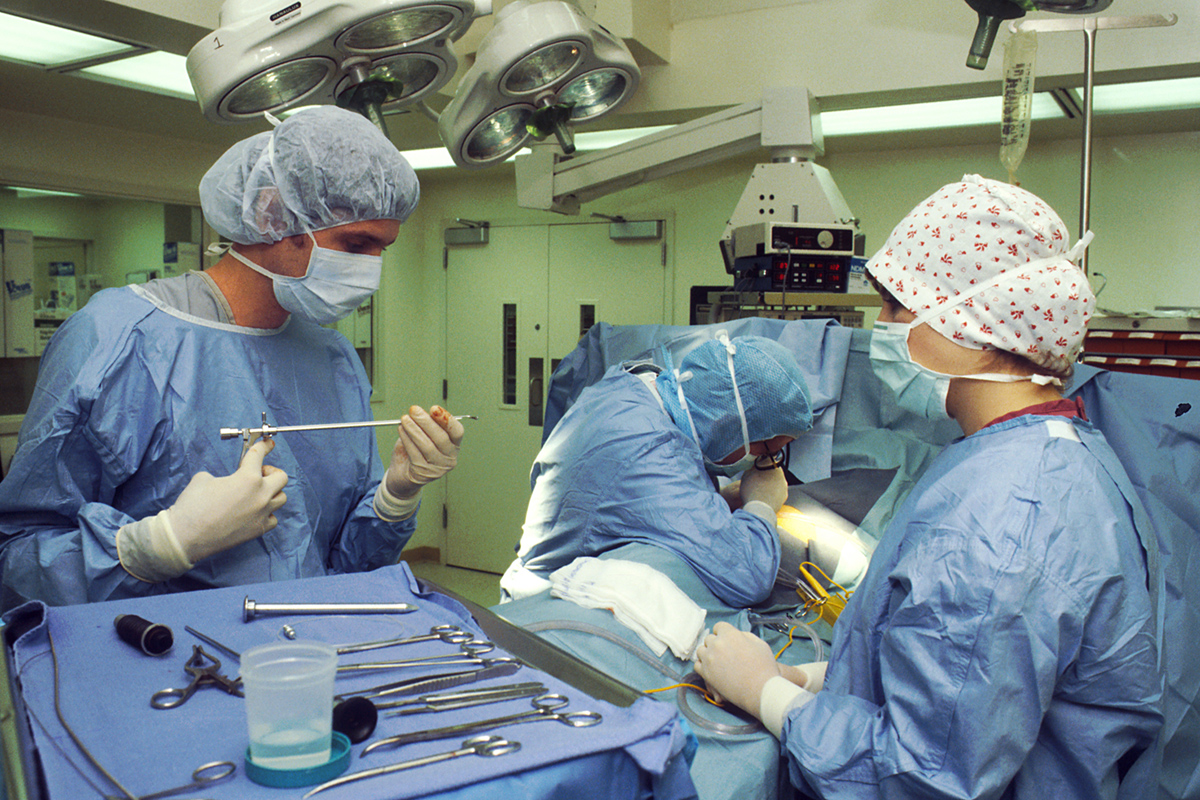
Gastroesophageal reflux disease (GERD), also known as acid reflux disease or gastric reflux disease, is a chronic condition characterized by the backflow of stomach acid into the esophagus. People suffering from this digestive illness experience heartburn, difficulty when swallowing, chest pain, the feeling as if they have a lump in the throat, hoarseness or sore throat. The condition is most commonly treated with medication or surgically.
Incisionless surgery
It is estimated that around 20 percent of Americans suffer from symptoms associated with GERD, which is why the Center for the Future of Surgery at UC San Diego Medical Center is testing this new surgical procedure that would provide relief for around 20 million of people across the country. This clinical trial procedure has received approval from UCSD Institutional Review Board and has been ongoing since November 2009.
The procedure takes 45 minutes and is carried out with an endoscope (a long, flexible tube affixed with a small camera) used for the examination of the interior of organs. In this procedure surgical instruments are fixed onto an endoscope and then lowered down the patient’s upper stomach through their mouth. The surgeon then uses three small titanium staples to link a small segment of the stomach to the upper esophagus. It is important to note that this is performed through a sophisticated computerized device operated by a surgeon. In patients with GERD, the muscle in the lower part of the esophagus weakens and are no longer able to function as a valve, which prevents the stomach contents from travelling back up to the esophagus. This surgery enables the muscle to act as a protective valve again.
Advantages
The advantages of incisionless surgery are many. Traditional methods to correct GERD include open surgery, in which one long incision is made in the patient’s abdomen as well as the less invasive laparoscopy procedure. , in which the surgeon creates up to five incisions in order to place the instruments and operate on the patient. This new procedure, still undergoing clinical trials, is minimally invasive, as it does not rely on incisions to restore esophagus to its normal function. No incisions means no stitches, which further means that the patient needs less time to recover. Thus, the need for painkillers accompanying the recovery process of the person undergoing a traditional procedure is eliminated. Surgeons testing this procedure state that the primary side effect of this incisionless surgery is a sore throat.












Your thoughts on this
Loading...