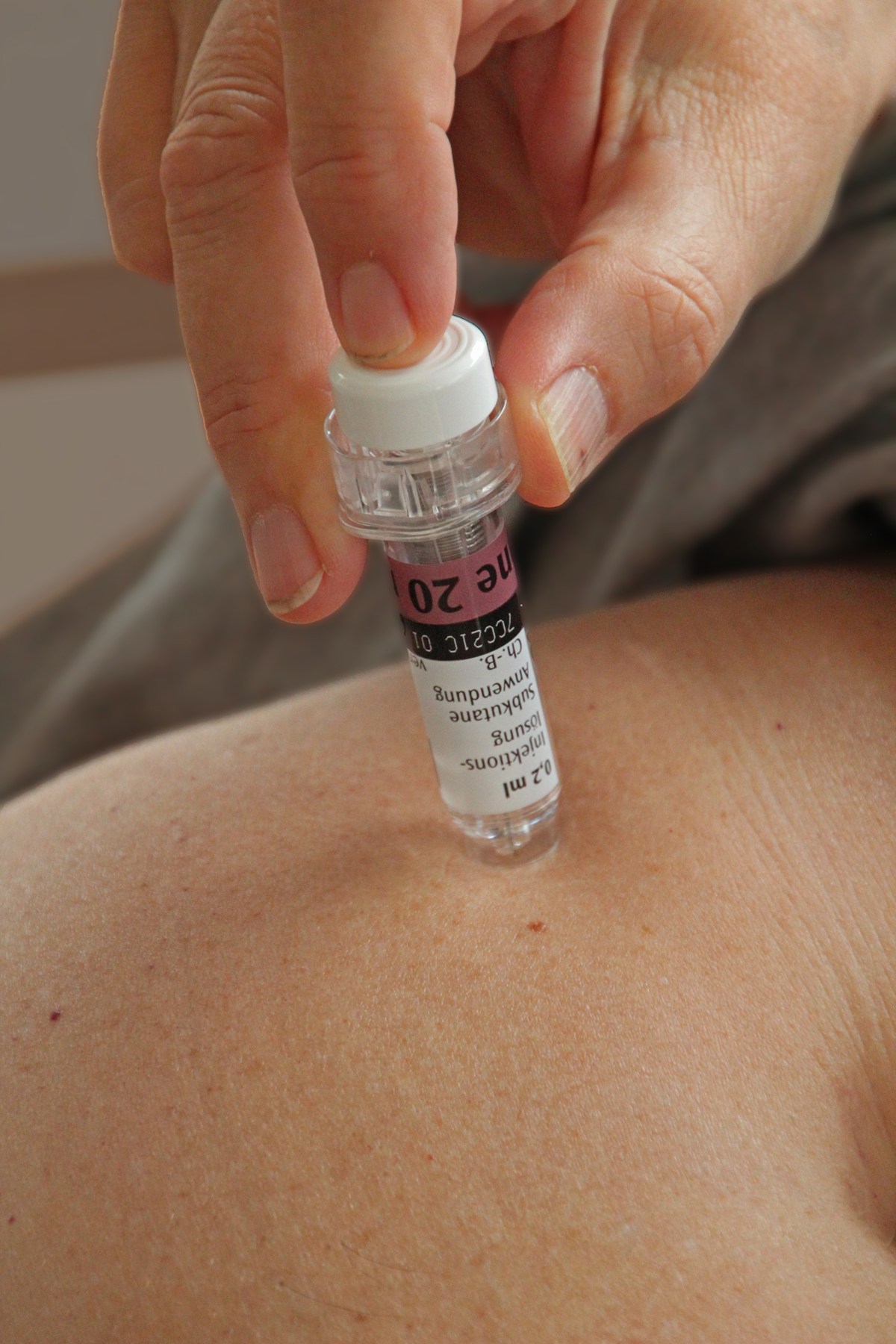
Tinzaparin is the blood thinning (anti-coagulant) medication that belongs to the group of low molecular weight heparin (LMWH). As all other LMWH, tinzaparin is used for prevention of blood clots and the treatment of deep vein thrombosis (DVT) and pulmonary embolism (blood clots in the lungs).
It is usually given subcutaneously or in some cases intravenously.
Side Effects
The most common tinzaparin side effects include hematologic problems. There are reports of patients experiencing hemorrhage, hematoma, thrombocytopenia, epistaxis, hematuria and anemia. Many different bleedings and blood-related problems were also associated with the use of this medication.
Heparin-inducedthrombocytopenia (HIT) may be present in patients using unfractioned heparin or LMWHs, and could lead to transient ischemic attack, skin necrosis, thrombosis, gangrene or stroke. Women, especially non-white, with lower body weight or with thrombocytopenia, are at greater risk of developing this condition.
Patients using tinzaparin might also experience heart and chest problems: chest pain, hypo or hyper-tension, angina pectoris, tachycardia, etc. Some patients reported pulmonary embolism or liver problems while using this drug.
There might be present some headache, fever, nausea, vomiting, digestion difficulties, and also some back pain in these patients. Tinzaparin also affects the central nervous system and may induce dizziness and confusion.
Skin problems are present at the injection spot and people complained about hematoma, abscess, cellulitis and skin necrosis. Some of the patients using tinzaparin experienced rash, pruritus, urticaria or ischemic necrosis.
Complications
Patients using tinzaparin while having some other medical condition might bleed easily. This include: bleeding diseases, poorly controlled hypertension, abdominal bleeding, kidney or liver problems, amyloidosis or infection of the heart lining. Recent surgical procedures, especially eye, brain or spine surgeries might also cause the same unwanted effect.
There is a possibility of severe blood clots in the brain or spinal cord, if you are using tinzaparin. This potential complication is emphasized in patients who had recent epidural anesthesia, lumbar puncture (spinal tap), spinal surgery or genetic spinal defect. Other blood thinners, Aspirin and NSAIDs (non steroidal anti-inflammatory drugs) also have the same adverse effect.
Warning
Many drugs interfere with tinzaparin, so make sure to inform your doctor and pharmacist about all medications, OTC drugs and remedies you have been using.
Peopleallergic tinzaparin or any other substance in the drug should not use it. If you had an allergic reaction to heparin, benzyl alcohol, sulfites or pork products do not use this drug.
Patients with the history of low platelet count or those with active bleeding also shouldn’t use tinzaparin.
This medication may be responsible for some non-specified neoplasms.












Your thoughts on this
Loading...