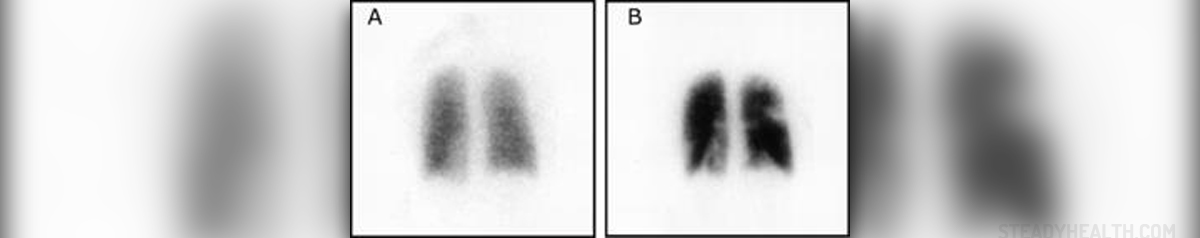
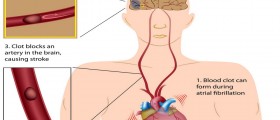
Blockage of one or more arteries in the lungs may cause the condition known as pulmonary embolism. This may happen to healthy people, if a blood clot from some part of the body travels to the lungs and blocks an artery or arteries.
People affected by pulmonary embolism may experience various symptoms, depending on the severity of the condition, involvement of the lungs and general health of the affected individual. Patients suffering from heart or lung diseases may find their condition to be a contributing factor to pulmonary embolism.
What Are Symptoms of Pulmonary Embolism?
Most patients experience sudden and unexplained shortness of breath, that does not correspond to the level of activity the person is engaged in. Chest pain and cough with bloody or blood streaked sputum are also quite common among people suffering from pulmonary embolism. Some of the patients may suspect they are having a heart attack because of severe chest pain they are experiencing, especially while they cough or breathe deeply or even try to eat, stoop or bend.
Pulmonary embolism can also induce wheezing, weak pulse, rapid or irregular heartbeats and fainting or lightheadedness. Patients also report that they sweat excessively and they have clammy or bluish skin, due to lack of oxygen.
Any unexplained shortness of breath, chest pain or bloody cough should be reported to your doctor immediately, since pulmonary embolism may be very severe medical condition and even pose a threat to your life. Prompt treatment with some medications against blood clotting is known to significantly reduce lethal consequences.
How to Prevent Pulmonary Embolism?
The most important thing when it comes to pulmonary embolism is to prevent clot formation in your vein, otherwise known as deep vein thrombosis.
Long flight or automobile rides are situations which may increase the risk of blood clots in the veins. Make sure to take a walk every now and then, at least once in an hour and you may also do several knee bends. While sitting, exercise the ankles and toes, avoiding sitting with crossed legs for a long time. Support stockings may also be a good idea to increase circulation in your legs.
In the hospital, your doctors may give some anticoagulant (anti-blood clotting) therapy, using heparin or warfarin to prevent formation of blood clots. There are also some graduated compression stockings that can be used, as well as some pneumatic compression. Physical activity is also appreciated among hospitalized patients at risk of developing blood clots.
- www.cdc.gov/ncbddd/dvt/facts.html
- www.cdc.gov/ncbddd/dvt/data.html
- Photo courtesy of Westgate EJ, FitzGerald GA by Wikimedia Commons: commons.wikimedia.org/wiki/File:Pulmonary_embolism_scintigraphy_PLoS.png










Your thoughts on this
Loading...