Optic neuritis is the medical term that refers to inflammation of the optic nerve, one of the twelve cranial nerves in charge of transmission of light signal processed in the retina to specific portions of the brain (the occipital cortex). The nerve comprises nerve tracts which may get seriously damaged if inflammation is not diagnosed timely and treated properly.
Optic Nerve Inflammation
The inflammation of this type affects people of all ages and may be unilateral or bilateral. However, the majority of patients are actually individuals between 30 and 35 years of age, mostly females. The prevalence of optic neuritis is 115/100,000 and each year around 5 out of 100,000 individuals develop the condition.
The actual cause of optic neuritis has not been identified yet. Scientist believe that the inflammation results from an underlying autoimmune disease. The body simply does not recognize the components of the nerve as its own parts. Instead they are mistaken for foreign particles hence they are attacked by antibodies and other active components of the immune system.
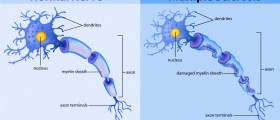
Many times optic neuritis is the first problem affecting people suffering from multiple sclerosis. In multiple sclerosis the body attacks the myelin sheath covering nerve fibers. Once myelin gets damages the underlying nerve cells are no longer protected and get easily damaged as well. Various parts of the brain and spinal cord may be affects by the process of demyelination including the optic nerve. Inflammation of the nerve is frequently recurrent.
Furthermore, neuromyelitis optica is one more autoimmune disease that may precipitate optic neuritis. This medical condition leads to more complex and severe inflammation of the nerve compared to inflammation associated with multiple sclerosis.
It is also possible to develop optic neuritis as a complication of various other diseases that are not autoimmune in origin. For example, inflammation of the optic nerve is reported to affect people suffering from diabetes, bacterial or viral infections such as Lyme disease, TBC, HIV etc. and cranial arthritis. What is more, some drugs precipitate optic neuritis too. Certain antibiotics and ethambutol are only some of them. And finally, in rare instances optic neuritis develops as a side effect of radiation therapy or may be associated with Leber's hereditary optic neuropathy.
Once the nerve gets inflamed and swollen its function becomes impaired. Loss of vision develops over the course of an hour or several hours, the pupil loses its ability to react when stimulated by bright light and one also have problems regarding color vision. Inflammation additionally triggers pain which is particularly intense while moving the eyeballs.
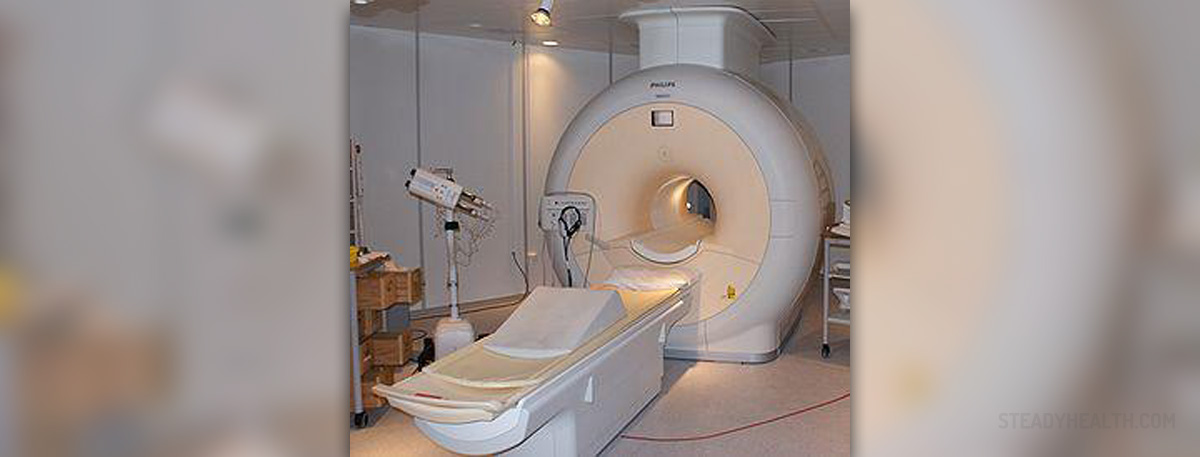
MRI Scan to Diagnose Optic Neuritis
MRI ( Magnetic Resonance Imaging) is a medical imaging technique highly efficient in visualization of internal structures of the body. The images of the desirable structures are obtained after a powerful magnetic field generated by the MRI machine aligns the magnetization of atoms in the parts of the body subjected to the test. This technique is especially capable of differentiating soft tissues in the body. By doing so doctors may have better insight in organs such as the brain, muscles and heart and damage they sustain. MRI posses no harm since it does not involves radiation of any kind However, it simply cannot be performed in people who have metal implants or metallic foreign objects in their bodies or a heart pacemaker. Severely claustrophobic patients are also not suitable candidates for MRI.
Now, this is a very efficient tool for diagnosing optic neuritis and sometimes identification of its underlying cause. In the majority of cases, however, optic neuritis can be easily diagnosed according to clinical and ophthalmologic examination findings. MRI of the nerve is basically reserved for atypical cases when doctors are not sure whether the condition is actually optic neuritis or its resembles this type of inflammation. MRI in such atypical cases may additionally help when it comes to obtaining information regarding future risk for development of multiple sclerosis. Namely, certain white-matter abnormalities of the brain may introduce the forthcoming multiple sclerosis. It is estimated that optic neuritis actually represents an introduction to multiple sclerosis in approximately 15-20% of patients with such brain changes. Also, around half of patients with optic neuritis are at risk of developing multiple sclerosis within the following 15 years.
Additionally, MRI may exclude other conditions that might have caused secondary inflammation of the nerve.
Unlike MRI, CT scans are not that sensitive when it comes to confirmation of optic neuritis. This is the reason why this medical imaging technique is not routinely engaged in the process of diagnosing the condition.
Patients suffering from optic neuritis may spontaneously recover within 2-3 weeks. Others require medications such as corticosteroids that will speed up the recovery, reduce swelling and prevent irreversible damage to the nerve. Patients in whom optic neuritis is not associated with multiple sclerosis have better chances to recover completely without any sequelae. Potential complications stem either from the inflammation itself or the administered drugs. Patients may experience a wide range of side effects due to corticosteroids or the very damage to the optic nerve may trigger vision loss.


_f_280x120.jpg)





-And-Multiple-Sclerosis-Differences-And-Similarities_f_280x120.jpg)





Your thoughts on this
Loading...