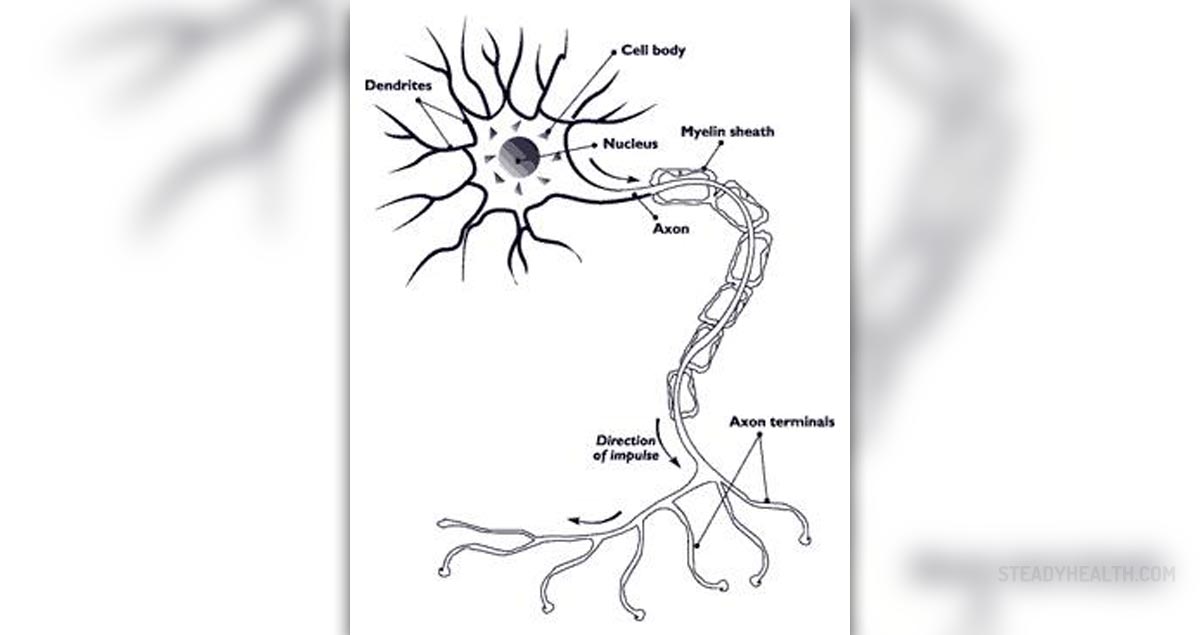
The trigeminal nerve is one of 12 cranial nerves (the 5th cranial nerve) that innervates the face and is in charge of sensation in the face. Trigeminal neuralgia is a medical condition that leads to painful sensations distributed throughout tissues innervated by the trigeminal nerve. Apart from pain patients suffering from trigeminal neuralgia may also experience facial spasms and tics. The pain predominantly remains localized on one side of the face. The diagnosis of the condition can be confirmed only when other neurological abnormalities are excluded including trigeminal neuralgia which develops as a result of some structural lesions of the nerve.
What is Trigeminal Neuralgia?
The condition is blamed for one of the most severe types of pain a man can experience. The pain such patients typically feel is described as shock-like. Repeated attacks may occur within minutes. Many times patients feel pain after specific spots are stimulated. These are known as trigger points and may vary from patient to patient. Once the initial attack subsides patients enter remission which may last from several days to sometimes years.
Trigeminal neuralgia is actually a very rare condition. It is estimated that each year around 150 out of a million individuals get affected. It may affect people of all ages, although people over the age of 50 seem to be more prone to this type of neuralgia.
Scientists have identified several underlying causes of the condition. The pressure of a blood vessel on the root of the trigeminal nerve seems to play significant role in the onset of pain. Also, the pain may be associated with demyelinization which is, for instance, seen in patients suffering from multiple sclerosis, especially advanced stages of the disease. Furthermore, pressure of a tumor on the nerve and physical damage to the nerve are two more reasons behind trigeminal neuralgia. Finally, in some patients the condition is idiopathic while there are also assumptions that sometimes the disease can be inherited.
No matter what the cause is, practically all patients complain about the same symptoms. They experience sudden, sharp pain which may be additionally described as stinging or stabbing. It lasts for a couple of minutes and easily repeats. The pain is generally distributed over one half of the face. In rare occasions both sides are affected. Certain activities and pressure applied onto certain parts of the face may precipitate the pain. For instance, some patients experience pain while eating or talking while in others shaving or even touching the face may be accompanied by excruciating pain.
All individuals suffering from trigeminal neuralgia may be classified into those with 'classic' trigeminal neuralgia pain and others with atypical trigeminal neuralgia pain. In the first group the pain is sharp, throbbing and resembles electrical shocks. The facial muscles remain strong and there is no numbness. Patients enter distinct periods of remission and they generally respond well to treatment with Tegretol.
Atypical form of the disease is also characterized by shock-like pain. The pain is usually described as throbbing or burning. Some individuals experience pulsating and crushing painful sensations. Unfortunately, these patients may not have remission at all. The condition is severe and complex. What is more, it is simply resistant to most available medications which makes treatment practically inefficient.
MRI in Diagnosing Process of Trigeminal Neuralgia
MRI (magnetic resonance imaging) is a powerful imaging technique which efficiently gives insight in many soft tissues in the body without using radiation. It is rather expensive diagnostic procedure, therefore, may not be indicated in all patients suffering from trigeminal neuralgia.
Now, initially, the process of diagnosing the condition starts with patient's medical history, physical and neurological exam. Symptoms and signs of the disease are very helpful but additional tests are simply essential for confirmation of the disease. These also rule out other conditions that may mimic trigeminal neuralgia.
Both CAT scan and MRI may be used in such patients. MRI (and even high-definition MRI angiography) provides with perfect insight in the very nerve and the brain stem and may confirm if the nerve is under compression due to enlarged vein or artery. The best results are achieved with a special MRI technique called 3-D volume acquisition where patients receive a contrast injection. Many times MRI shows no abnormalities which makes the condition idiopathic.
Still, there are no specific tests that can for sure confirm trigeminal neuralgia. So, most doctors rely on clinical findings and MRI exams.
As far as treatment for trigeminal neuralgia is concerned, doctors may opt for several medications. Carbamazepine is an anticonvulsant and the first drug of choice for these patients. If it fails to provide with desirable results, patients may be prescribed baclofen, clonazepam or gabapentin. Pain associated with trigeminal neuralgia might be brought under control with a newly introduced agent called Trileptal. The drug seems to have fewer side effects compared to carabamazepin.
And finally, in case medicamentous therapy is not sufficient enough in controlling painful sensations, patients undergo surgery. There are several techniques applied and they include gamma-knife radiosurgery, microvascular decompression, balloon compression, radiofrequency thermal rhizotomy or rhizotomy alone (severing the nerve) as well as glycerol injections.











Your thoughts on this
Loading...