Definition
A mammogram is an x-ray examination of the breasts that is utilized for cancer inspection, and in various stages of cancer. For instance, the screening mammogram is performed on women who are not experiencing any kind of symptoms as a routine check. A mammogram is able to reveal two distinct signs of breast cancer, such as a lump that hasn’t appeared yet as well as higher levels of calcium, which sometimes allude to cancer. At the same time, once a lump is discovered a diagnostic mammogram is employed to further investigate the changes identified by the screening mammogram. In addition, there has been a wide range of scientific research done to explore the benefits of regular breast checkups, and on the whole most clinicians agree that mammograms do reduce the death rate of breast cancer. It is highly advised that women over 35 years of age get a mammogram every 1 to 2 years, while anyone who experiences symptoms like nipple discharge or pain should definitely consult with a medical care provider in a timely manner.
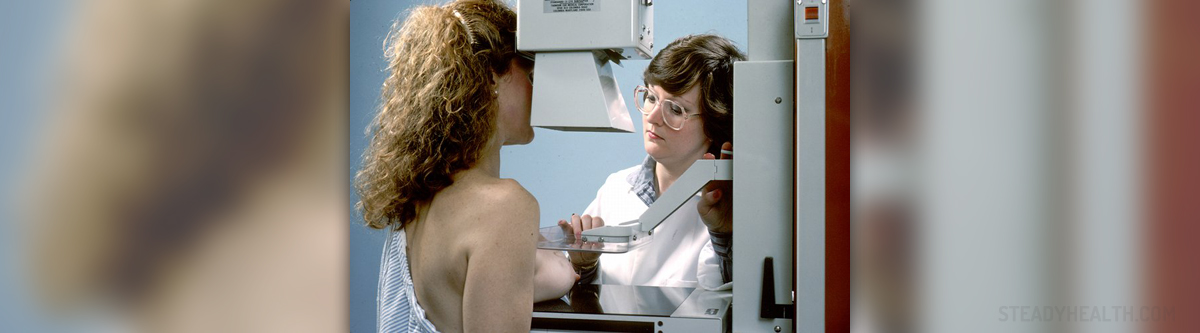
How a Mammogram is Performed
In order to get a mammogram, an individual makes an appointment with an authorized health care professional, in this case a radiologic technologist. During an examination, the breasts are placed on a stand and pressed with a paddle for the sake of levelling out the tissue so that the x–ray can be performed quickly and accurately. The compression of the breasts reduces the fogginess as well as the dispersing of the image. On the other hand, the compression produces discomfort and it is advised that individuals with sensitive breasts have the mammograms taken when the tenderness is least felt in the cycle. Further, a mammogram takes two images of each breast, one from the top to the bottom, and the other from the side, so the patient is asked to switch positions. At the same time, individuals must remain motionless during the taking of the image. An examination usually lasts for half an hour, although the diagnostic mammogram might take a little more time as more images are necessary. A radiologist sends the results of a mammogram to the primary health care provider of the patient, who further proposes a course of treatment or follow up tests. Additional analysis is usually recommended if there is a change detected by an x–ray as there are other means of testing that yield more detailed results in certain instances.
Screening Mammograms
Screening mammograms are widely used for early detection of breast cancer. They have proved to be valid as well as reliable, producing results that lead to the commencement of early therapy and subsequently to saving lives. It should be noted, however, that early detection does not guarantee full recovery nor does it help individuals whose health condition is already damaged beyond repair. As is the case with many medical tests, a screening mammogram is not capable of detecting cancer every time, and will miss, on average, around 20 percent of tumors that are actually present. A breast is composed of fatty tissue, which emerges as dark matter on an x–ray, and dense tissue, which emerges as light matter when screened. As the cancer cells also surface as light matter and can be confused for dense tissue, the screening mammogram is not always accurate. It should be noted that younger women have more dense tissue than their older counterparts and are at a higher risk of receiving a false result from a mammogram. A false result in turn postpones therapy and provides a deceitful sense of security. There are also cases in which a mammogram does not necessarily detect cancer, but it does not appear to be normal either. Additional testing, such as ultra sound or a biopsy, is recommended to get to the source of a potential problem. Similarly, younger women are more prone to false positive mammograms, but so are those individuals with breast cancer history or persons who are receiving any kind of estrogen or hormonal therapy. False positive results can lead to unnecessary emotional stress, but in any case must be followed up with supplementary analyses. Further, there have been many instances in which a screening mammogram detects a change in the breast tissue that will not cause any discomfort or pose a threat but nevertheless labels it as cancer. Such occurrences lead to overdiagnosis, and subsequently unnecessary cancer treatment, which in and of itself can leave many adverse health consequences. Finally, all mammograms need a portion of radiation, which is in general harmless, but after repeated exposure is known to produce cancer. A medical care provider who is performing the mammogram should always be aware of any underlying illnesses a person may have as well as if there is a possibility that a patient might be pregnant.



_f_280x120.jpg)






_f_280x120.jpg)
Your thoughts on this
Loading...