The cystic duct is anatomical structure which connects the gallbladder and extrahepatic bile duct. There are several anatomical variants of cystic duct but in most cases these are not clinically relevant problems. More often, dilation of cystic duct is seen to cause confusion after some imaging studies performed on the patient. However, primary and secondary diseases may also be associated with cystic duct dilation and this condition should be properly diagnosed.
Cystic Duct Anatomy
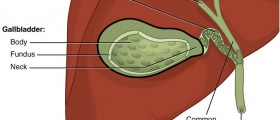
As mentioned, the cystic duct joins extrahepatic bile duct and the gallbladder. It is usually several centimeters (2 to 4 cm) long, containing concentric folds which are called the spiral valves of Heister. This structure is frequently seen as to have serpentine or tortuous course, while its diameter is normally somewhere from 1 to 5mm (millimeters).
In most people, the cystic duct enters the extrahepatic bile duct from the right lateral position. It can also enter this duct from medial, anterior or posterior aspect, but these cases are much rarer. Cystic duct is runs parallel to extrahepatic bile duct and it can be of spiral course in some patients.
Diagnostic Methods
Depiction of normal anatomy and changes of the cystic duct may be seen on different procedures and imaging. Doctors may use: computed tomography (CT), direct cholangiography, magnetic resonance (MR) imaging (MR cholangiopancreatography, and cholescintigraphy) or ultrasonography (US). Direct cholangiography could include endoscopic retrograde cholangiopancreatography (ERCP), intraoperative cholangiography, percutaneous transhepatic cholangiography (PTC) and T tube. Out of all these diagnostic and depiction methods, direct cholangiography and MR cholangiopancreatography have been considered to give optimal visualization in almost every case.
In direct cholangiography the cystic duct is filled with adequate amount of contrast material in injection, after which, the patient is placed in optimal position. If there is no filling of the cystic duct, patients positioning is more common explanation than any obstruction of the cystic duct.
The cystic duct is seen as high signal intensity structure on MR cholangiopancreatography. Alteration of image acquisition is usually helpful to differentiate extrahepatic bile duct and the cystic duct (if they happen to overlap). T2 weighed sequences are considered as optimal to depict the cystic duct. T1 weighed images are also good, but only when the cystic duct contains concentrated bile.
Dilation of Cystic Duct
Obstruction of the biliary tract may cause cystic duct dilation, especially when the cystic duct is located above the obstruction lesion. Dilation can be so significant, that the cystic duct may appear as gallbladder or dilated hepatic branch. However, this condition doesn’t have to provoke dilation of the cystic duct and it may stay of normal size even if there is some significant dilation of the extrahepatic bile duct.
Dilated cystic duct should be properly diagnosed, in order to avoid complications such as leakage of the bile, cystic duct injuries or mistaken placement of proximal end of endoscopic stent into the cystic duct. Additionally, dilated cystic duct may look like: cystic mass in porta hepatis or the head of pancreas.
- www.ncbi.nlm.nih.gov/pmc/articles/PMC3693258/
- medlineplus.gov/ency/article/000263.htm
- Photo courtesy of Madhero88 by Wikimedia Commons: commons.wikimedia.org/wiki/File:Gallbladder.png










Your thoughts on this
Loading...