
Toxic shock syndrome is a potentially deadly condition, taking place due to one's exposure to several different types of bacterial toxins, depending on the type of infection which provokes it. Most commonly, this condition is triggered by two different types of bacteria – Streptococcus pyogenes and Staphylococcus aureus, even though the former case is not so frequent.
Therefore, it you desire to learn more about the toxic shock syndrome, predominantly the causes and symptoms behind it, go through the lines below.
Symptoms of Toxic Shock Syndrome
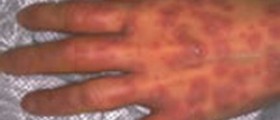
Commonly, the signs behind this condition depend greatly on the underlying causes of it. Therefore, the toxic shock syndrome related to staphylococcus aureus may typically manifest through a high fever, low blood pressure, confusion and malaise and, once the condition reaches a higher level of severity, coma, stupor or even organ failure and death. Usually, the infected individuals experience the appearance of a rash on the surface of their skin, being quite similar to sunburns. The rash may appear anywhere on the body, even on the lips, mouth, eyes, palms and soles.
If an individual manages to go through the worst stages of the toxic shock syndrome of this type, after about two weeks, the rash is likely to peel off or fall off.
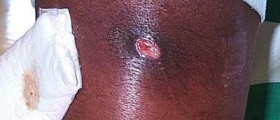
On the other hand, if the toxic shock syndrome is triggered by the exposure to toxins originating from streptococcus pyogenes, the symptoms are likely to be different. Namely, people who develop this form of infection are likely to have suffered from some other kinds of skin infections stemming from the exposure to the same bacteria. The pain may occur at the site of the infection and the symptoms similar to the ones mentioned above may start appearing. However, the sunburn rash is usually not present during toxic shock syndrome caused by this sort of bacteria.
All in all, the symptoms of the toxic shock syndrome, according to the 1981 CDC criteria are high body temperature (fever), being above 38.9 degrees Celsius or 102.2F, blood pressure lower than 90mmHg and the rash, manifesting through intense erythroderma, with subsequent desquamation, concentrating on the soles of the feet and the palms predominantly.
Some other symptoms which may appear hand-in-hand with the toxic shock syndrome are vomiting and diarrhea, hyperemia of vaginal, oral or conjuctival mucous membranes, kidney failure, hepatic inflammation, thrombocytopenia and confusion.
Treatment Options
Most commonly, toxic shock syndrome requires immediate hospitalization. The patients are usually admitted to the intensive care and provided with fluid management, ventilation, renal replacement therapy and inotropic support, depending on the severity of the symptoms and the presence or absence of kidney or other organ failure.
The health experts concentrate on removing the cause of the toxic shock syndrome, draining the abscesses or collections. Since many cases of toxic shock syndrome take place due to inadequate use of tampons, if this is the case, these should be removed. Basically, if the trigger of the infection is not removed, the chances of treatment are significantly decreased.
The bacteria itself are dealt with through antibiotic therapy, mainly based on a combination of cephalosporins, penicilins or vancomycin. Sometimes, clindamycin or gentamicin may be added to the combination, stopping the productions of toxins and increasing the chances of recovery.
Prognosis
Typically, if this condition is treated timely, full recovery is likely to occur within two or three weeks. However, without the proper treatment, the toxic shock syndrome can lead to death in a matter of hours.
Statistically, based on a study carried out by Patrick Schlievert in 2004, 3 or 4 cases of toxic shock syndrome appear in 100,000 females who use tampons on a yearly basis. Some tampon production companies have confirmed even higher numbers of such occurrences, declaring that about 1 to 17 women, among 100,000 tampon users suffer from toxic shock syndrome every year. In California, eight people have died from toxic shock syndrome over the course of 3 years, from 2000 to 2003 and experts claim that, taking into consideration that, today, women experience menstruation earlier than before, the numbers are rising. Nevertheless, negligence is a common factor in toxic shock syndrome affecting tampon users. Namely, the tampon is usually forgotten and left inside the body prior to the onset of the infection. On the other hand, some health experts consider the new types of highly absorbent tampons responsible for the occurrence of toxic shock syndrome.
Either way, it is highly advisable not to leave the tampons in overnight, let alone for longer periods of time. Hygiene plays a great role in prevention of this condition.
All in all, many different symptoms are related to the toxic shock syndrome. Usually, the initial symptoms are mild and the severity of the condition escalates with the infection and toxin exposure themselves. Timely treatment is necessary in cases of toxic shock syndrome, increasing one's chances of survival. Simply, if proper treatment does not take place, the sufferer is likely to die.
Therefore, be careful regarding the toxic shock syndrome, pay attention to your hygiene and react timely if you notice any of the above mentioned symptoms, seeking immediate medical assistance.










Your thoughts on this
Loading...