Tonsillitis is an inflammation of the tonsils. The most common bacteria that cause this disease include group A, B, C, and G hemolytic streptococci. All hemolytic bacteria are connected with the development of rheumatic fever, which is only one of the compilations of tonsillitis.
The condition very rarely occurs due to infection caused by Bacteroides species, Hemophilus influenza, Staphylococcus aureus, Moraxella catarrhalis, and Mycoplasma pneumoniae. Extreme cases may include Corynebacterium diphteriae and Francisella tularensis. They are responsible for lethal membranous pharyngotonsillitis.
Complications
Severe complications are not so common, but if they occur, they include peritonsillar and intratonsillar abscesses, deep neck space infections, inflammatory torticollis, hemorrhagic tonsillitis, postangilar sepsis, and vascular complications.
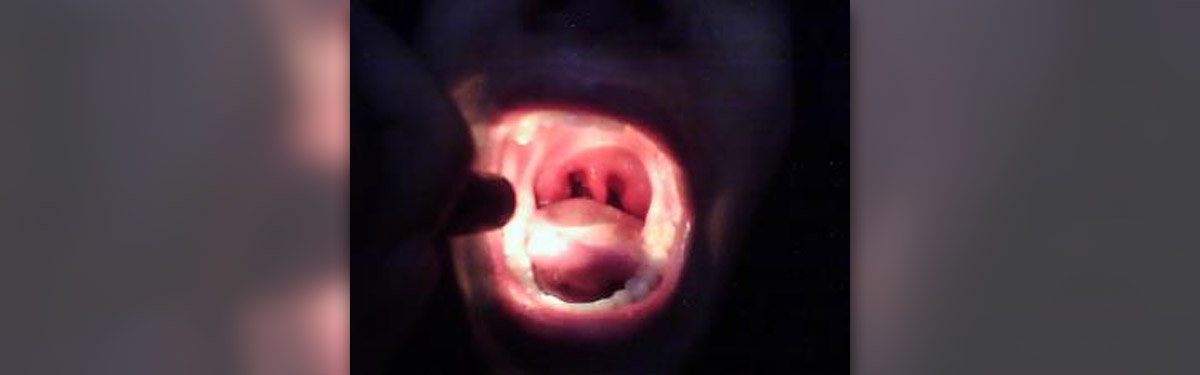
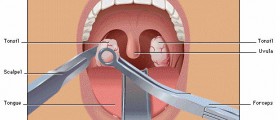
Peritonsillar abscess is a collection of pus located in deep areas of the neck. This most frequent infection spreads along the connective tissue of the tonsils into the peritonsillar space. Sometimes, this condition is treated by needle aspiration or by making an incision along with the drainage of the abscess. Another solution is tonsillectomy.
Intratonsillar abscess, also known as phlegmonous tonsillitis is rather rare and includes the formation of the very abscess within the tonsil. The symptoms and the treatment for this complication are the same as in the case of peritonsillar abscess.
Deep neck infections are not so frequent. What happens is that peritonsillar abscesses may spread and affect deep tissues of the neck (mainly peripharyngeal space, but peripharyngeal space can be affected as well). The condition is very dangerous and the patient shows signs of fever and prostration. The diagnosis is set after the CT scan of the head and neck is performed. The treatment includes antibiotics and external drainage. The most severe cases can end with erosion of the internal carotid artery, thrombophlebitis of the internal jugular vein, or mediastinitis and necrotizing fasciitis.
Inflammatory torticollis occurs when the infection spreads to the neck and the neck is in the wrong position either drawn down or rotated to one side with the chin facing the other side. This is due to a spasm of the sternocleidomastoid muscle. The treatment for this condition is immobilization of the neck. The spine films have to rule out the possibility of fracture and rotatory subluxation.
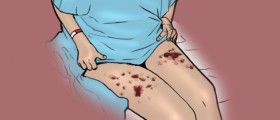
Vascular complications include the formation of hematoma which is a tense, purple, or brownish change on the skin or mucosa. This is caused by peritonsillar abscesses and deep neck abscesses. All the cases which include recurrent hemorrhage from the nose, ears, or throat must be thoroughly examined. A lingering clinical course of several weeks or more may point to the occult abscess. Cranial neuropathies of the X and the XII and even a case of Horner's syndrome must be taken seriously as they may be caused by the hemorrhage.
Hemorrhagic tonsillitis is an extremely rare complication.
Postanginal sepsis is a complication of anaerobic tonsillitis. It starts with mild tonsillar infection and ends with life-threatening thrombophlebitis of the internal jugular vein. The symptoms include strong pain in the neck and a palpable mass under the sternocleidomastoid muscle. High temperature, chills, and stiff neck are present as well.
This severe complication can lead to additional problems, including potential septic embolization and metastatic abscesses in the lungs, liver, or brain or septic arthritis osteomyelitis. The diagnosis is set by a CT scan, and the treatment includes antibiotics with an emphasis on anaerobic coverage. Even drainage of the abscess is performed together with ligation or excision of infected veins if necessary.
- The objective of this work was to study the epidemiological and therapeutic profile of tonsillitis and their complications in the ENT Department and Head and Neck Surgery of the Mother-Child University Hospital in Luxembourg.
- This is a prospective study over a 12-month period from January 2018 to December 2018, including all patients who presented with tonsillitis and/or their complications.
- Three hundred and fifteen (315) patients were collected during this period. The average age in our study was 14.25 years with extremes ranging from 2 years to 61 years. The sex ratio was 0.65 in favor of the female sex. During this period we recorded 80.95% of cases of uncomplicated tonsillitis including 60.50% for acute tonsillitis, 24.5% for chronic tonsillitis 5% for adenoid tonsillitis and 19.05% for complications.
- Complications included peritonsillar phlegmon 42.22%, heart disease 33.33%, cervical cellulitis 8.89%, adeno-phlegmon 6.67%, para-pharyngeal abscess 4.44%, and sepsis 4.44%. The exclusive medical treatment was performed in 44.31%. Surgical treatment (drainage incision and tonsillectomy) was performed in 55.69%.










Your thoughts on this
Loading...