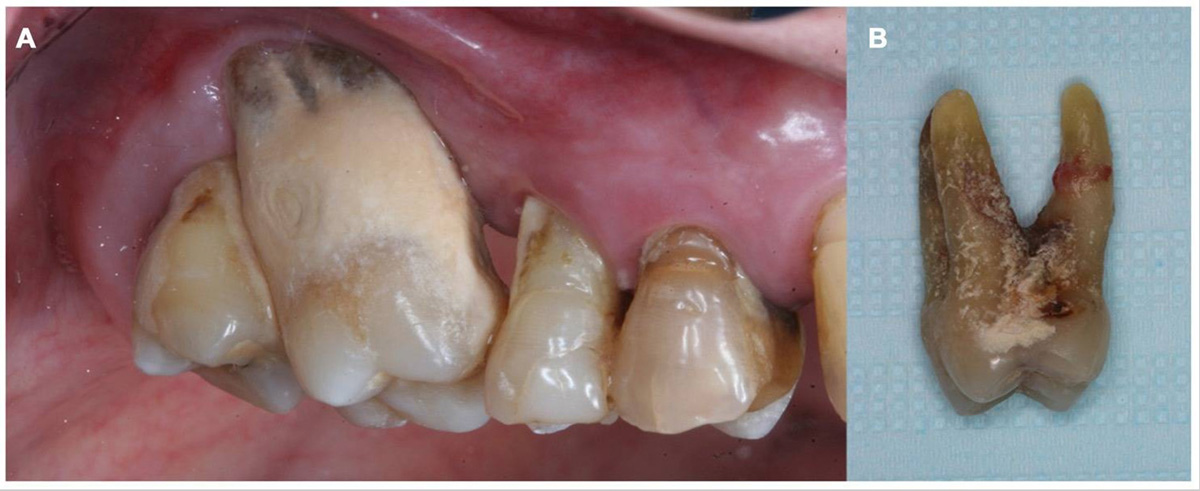
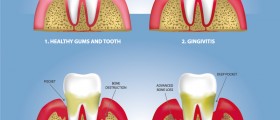
Periodontitis is a type of inflammatory condition that affects the soft tissue around our teeth, and is caused by microorganisms living on their surface. This is a progressive disease that attacks the alveolar bone, and if left untreated will lead to tooth loss. A professional, called periodontist, conducts a test for periodontitis by performing a clinical exam, as well as taking x rays of the patient’s mouth (the upper and lower jawbone).
When it comes to periodontitis, there are seven major types of the condition including gingivitis, chronic periodontitis, aggressive periodontitis, periodontitis as a manifestation of systemic disease, necrotizing ulcerative gingivitis and/or periodontitis, abscesses of the periodontium, and combined periodontic-endodontic lesions. Further, the magnitude of the condition alludes to the percentage of sites of dentition affected in the patient. There are six probing sites including mesiobuccal, mid-buccal, distobuccal, mesiolingual, mid-lingual, and distolingual. If up to 30% of the sites are affected, the condition is classified as localized. Otherwise, it is termed as generalized. Lastly, the severity of this health issue is measured by the extent of periodontal ligament fibers that have been lost. A mild attachment loss is 1-2mm, moderate 3-4 mm, whereas severe is 5 or more mm.
Periodontitis Epidemiology
Periodontitis is widespread in the United States with a prevalence of 30-50% of the population, with only 10% suffering from more severe forms. As daily oral hygiene is crucial to its prevention, periodontitis is more frequent among poor and developing regions, and consequently less common in those with more access to better dental care.
Periodontitis Signs and Symptoms
There are many easily recognizable signs and symptoms that accompany periodontitis such as tenderness, swelling, and bleeding of the gums while brushing, gingivial recession, bad breath, and loose teeth along with loose pockets between the gums and teeth. It should be noted that there are conditions in other parts of the body that are linked to periodontitis including diabetes, high level of C-reactive protein, myocardial infarction, and so on.
Causes of Periodontitis
Even though the main cause for both gingivitis and periodontitis is the microbial plaque that covers the teeth, there are many other factors that contribute to periodontitis. Things like poor oral hygiene, smoking, bad nutritional habits, diabetes, tartar or calculus formed from layers of plaque in the mouth, higher stress levels, low resistance to infection of the patient, and so on, have all been linked to the formation of periodontitis.
Periodontitis Initial Therapy and Surgery
Therapy for periodontitis starts with the elimination of microbial plaque and calculus. Firstly, the treatment will include cleaning below the gum line, which is called scaling. In some cases, root planing is employed, which is another kind of cleaning of the same area, but may require a local anesthesia and more than one visit to the dentist. Other elements of the problem could be addressed too, such as altering the bite, sealing of the gaps between teeth, and so on. Some dentists recommend at home injecting of anti-microbal solutions into the pockets as it reduces contamination and inflammation.
Furthermore, some individuals may require dental surgery to help stop the destruction of the periodontium caused by periodontitis. Types of periodontal surgery include open flap debridement, osseous surgery, and guided tissue regeneration and bone grafting. Periodontal surgery will remove the excess calculus build-up, and reduced the pockets as much as possible to stop further teeth loss and damage. Studies have shown that periodontal surgery is effective in stopping mild to progressive periodontitis insofar that it leads to less additional breakdown and tooth loss in nearly 85% of patients.
Periodontitis Prognosis
The level and severity of periodontitis are measured by a instrument called a periodontal probe. A periodontal probe is a stick that a dental professional installs into the space between the gums and the teeth, and if the probe can glide more than 3 mm below the gum line, the patient is thought to be able to clean it at home with a toothbrush. Consequently, if the probe slips more than 3mm into the pockets, regular cleansing at a dental office is required. Finally, if the depth of the pocket is more than 6-7 mm, surgical intervention is necessary to stop further damage.
Periodontitis Prevention
Typical daily oral hygiene routine is known to prevent periodontitis. Dental professionals recommend daily brushing using a soft tooth brush, regular flossing between meals, rinsing with antiseptic mouthwash solutions, using inter-dental tooth brushes, and having regular dental check-ups, as well as thorough removal of plaque build-up every 3 to 12 months. Individuals with arthritis, or other kinds of dexterity problems, for instance, may find it difficult to practice satisfactory oral hygiene, in which case frequent visits to the dentist are urged. By any means, the progression of periodontitis will not be stopped without the proper oral hygiene and it requires a continuing commitment on the part of the patient.









,-Don't-Ignore-Receding-Gums_f_280x120.jpg)


Your thoughts on this
Loading...