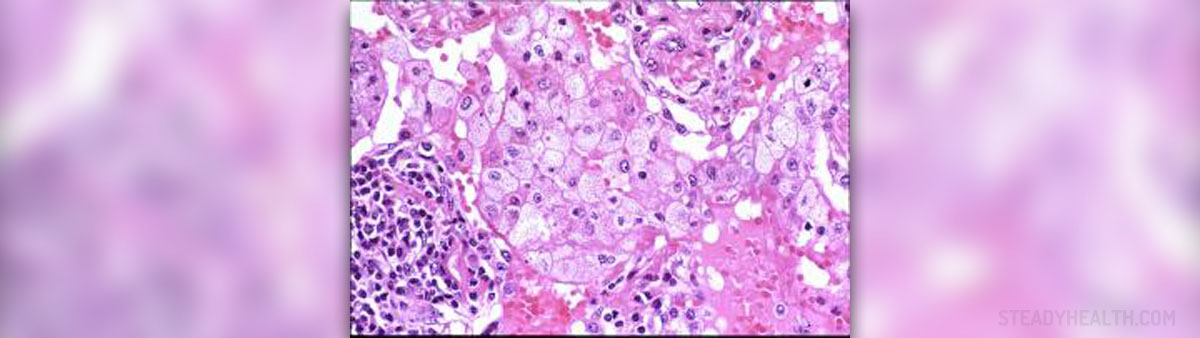
Pneumonia is an inflammatory infection of the lungs. It is characterized by inflammation of the parenchyma of the lungs, or alveoli, and abnormal alveolar filling with fluid. Pneumonia have a wide number of different causes. While bacterial infections are the most common culprit in pneumonia cases, viruses (including COVID-19), fungi, parasites, and chemical or physical injury to the lungs can all lead to pneumonia as well.
Pneumonia: Epidemiology
Pneumonia is a common, but very serious, disease that may occur at any point of life. It is one of the leading causes of death among children, elderly people, and those who are chronically ill. This disease is the leading cause of children’s death in developing countries. According to the World Health Organization, one in three newborn infant deaths are due to pneumonia. It is estimated that somewhere around 150 million new cases of pneumonia occur worldwide each year among children younger than 5 years. This means approximately 10 to 20 million hospitalizations. Up to 1 million of these deaths are caused by the bacteria Streptococcus pneumoniae, and this kind of pneumonia is vaccine-preventable.
Pathophysiology of pneumonia
Ppneumonia develops as a result of inflammation of the alveolar space, in one lung or both lungs. The alveoli are tiny sacs in human lungs that are filled with air. The alveoli are responsible for gas exchange, and any kind of inflammation in the alveolar space compromises this process.
Pneumonia commonly develops as a complication of other lower respiratory infections, such as bronchiolitis or laryngotracheobronchitis. However, pneumonia may also occur as a result of invasion by bacteria, viruses, or fungi, chemical injury or direct lung injury.
Bacteria are the most common cause of pneumonia. Streptococcus pneumoniae is the most common, but other pathogens such as anaerobic bacteria, Staphylococcus aureus, Haemophilus influenzae, Chlamydia pneumoniae, C. psittaci, C. trachomatis, Moraxella (Branhamella) catarrhalis, Legionella pneumophila, Klebsiella pneumoniae, and other gram-negative bacilli, may also cause pneumonia.
The pathophysiology of pneumonia is characterized by four stages. The first stage of the disease occurs within 24 hours of infection and it is distinguished by vascular congestion and alveolar edema. The lungs are also invaded by bacteria and few neutrophils. Typical symptoms include:
- Cough
- Fever
- Chills
- Increased sputum production
- Shortness of breath
- Sometimes pleurisy, an inflammation of the lining between your lungs and ribs, something that leads to chest pain
Loss of appetite, wheezing, joint and muscle aches, shivering, headaches, extreme fatigue, and feeling disoriented and confused are also all possible symptoms of pneumonia. Anyone who has a combination of these symptoms should seek medical help for proper diagnosis.
The second stage of pneumonia is called “red hepatization”. In this stage, the lungs take on a structure similar to the consistency of liver, with the presence of many erythrocytes, neutrophils, desquamated epithelial cells, and fibrin within the alveoli.
The third stage is the “gray hepatization” in which the lung is gray-brown to yellow because of fibrinopurulent exudate, disintegration of red cells, and hemosiderin.
The fourth, and the final, stage of pneumonia is called “resolution” and it is characterized by breakdown of the substances causing inflammation. In this stage, white blood cells are fighting off invading micro-organisms, and the remains are usually coughed up. This stage is characterized by restoration of the pulmonary architecture.
The management of pneumonia depends on its cause, and can include antibiotics, antifungal medications, and oxygen therapy.













Your thoughts on this
Loading...