
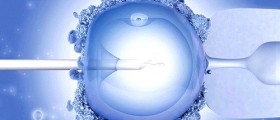
ICSI stands for intracytoplasmic sperm injection, and refers to a procedure in which a single sperm is injected directly into the center of a woman's egg. ICSI is used in conjunction to IVF, a procedure during which eggs are artificially retrieved from a woman's body, fertilized in a lab setting, and placed into the uterus. The usual invitro fertilization procedure involves places egg and sperm in a petri dish and waiting for fertilization to occur. ICSI, therefore, is a more specialized form of conventional IVF. ICSI is used in cases of male infertility, where a man has abnormal sperm. Healthy sperm are selected by the fertility clinic and chosen to be injected directly into the egg.
For the female partner, undergoing IVF with an intracytoplasmic sperm injection is identical to a more conventional round of IVF. Fertility drugs will be administered in preparation, eggs retrieved (see egg retrieval for IVF), and later put back. For men, ICSI might be more complicated but the real differences between ICSI and regular IVF lies in the lab procedures. The male will be required to provide a sperm sample, like with regular IVF. After this has happened, the healthy, good quality sperm is selected and separated from the abnormal sperm. Or in some cases, sperm can be removed directly from the scrotum, if an ejaculation does not provide sufficient sperm. This requires an additional procedure. Then, the sperm will be placed into the very center of an egg, hopefully resulting in the creation of an embryo.















Your thoughts on this
Loading...