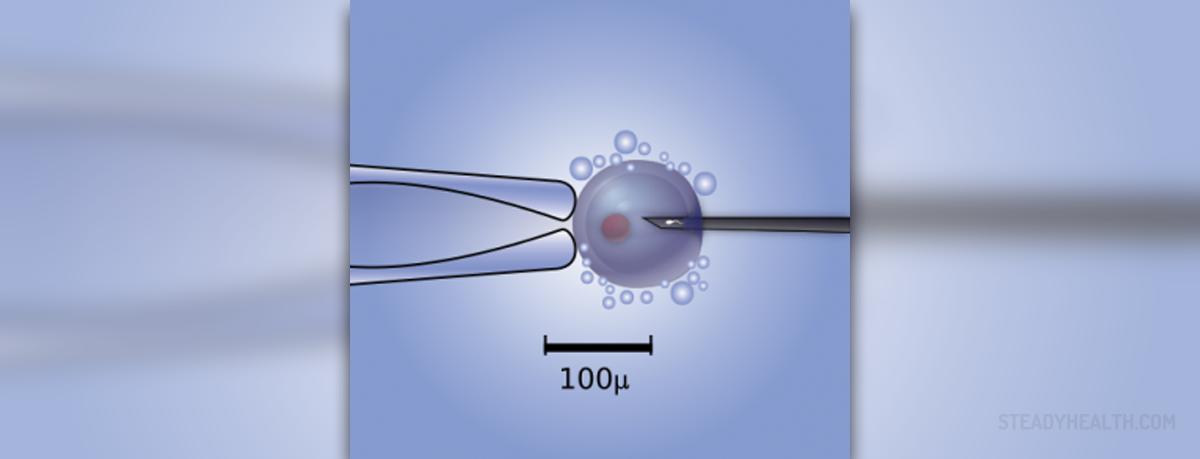
The use of ICSI has become more widespread in recent years, and according to some data, the procedure is now used in combination with around half of all IVF procedures. Unlike regular IVF, only one sperm is needed for ICSI. As the name intracytoplasmic sperm injection already suggests, one previously selected sperm is injected directly into the center of the egg. Embryos that are created in this manner can then be transferred into the uterus of the mother, or in some cases a surrogate mother. Intracytoplasmic sperm injection first came into use in 1992, and it is greatly increases the odds of pregnancy if the male partner has fertility problems. These can include problems with sperm morphology; the shape, size or structure of the sperm, as well as low sperm count, and motility problems (when the sperm "swim" too slowly).
Like any other IVF procedure, the female partner will first be administered fertility drugs to stimulate the release of multiple eggs. Once the eggs are harvested, a sperm sample will be taken from the male partner. If the man is not able to produce sperm through ejaculation, sperm can also be retrieved directly from his body in a separate medical procedure. This procedure is called testicular sperm extraction. After the sperm have become available, the chosen sperm are individually injected into the retrieved eggs. Once that stage has passed, the rest of the procedure is then the same as any other IVF procedure. If you need ICSI, you might benefit from reading about how to find the best fertility clinics for male infertility.












_f_280x120.jpg)

Your thoughts on this
Loading...