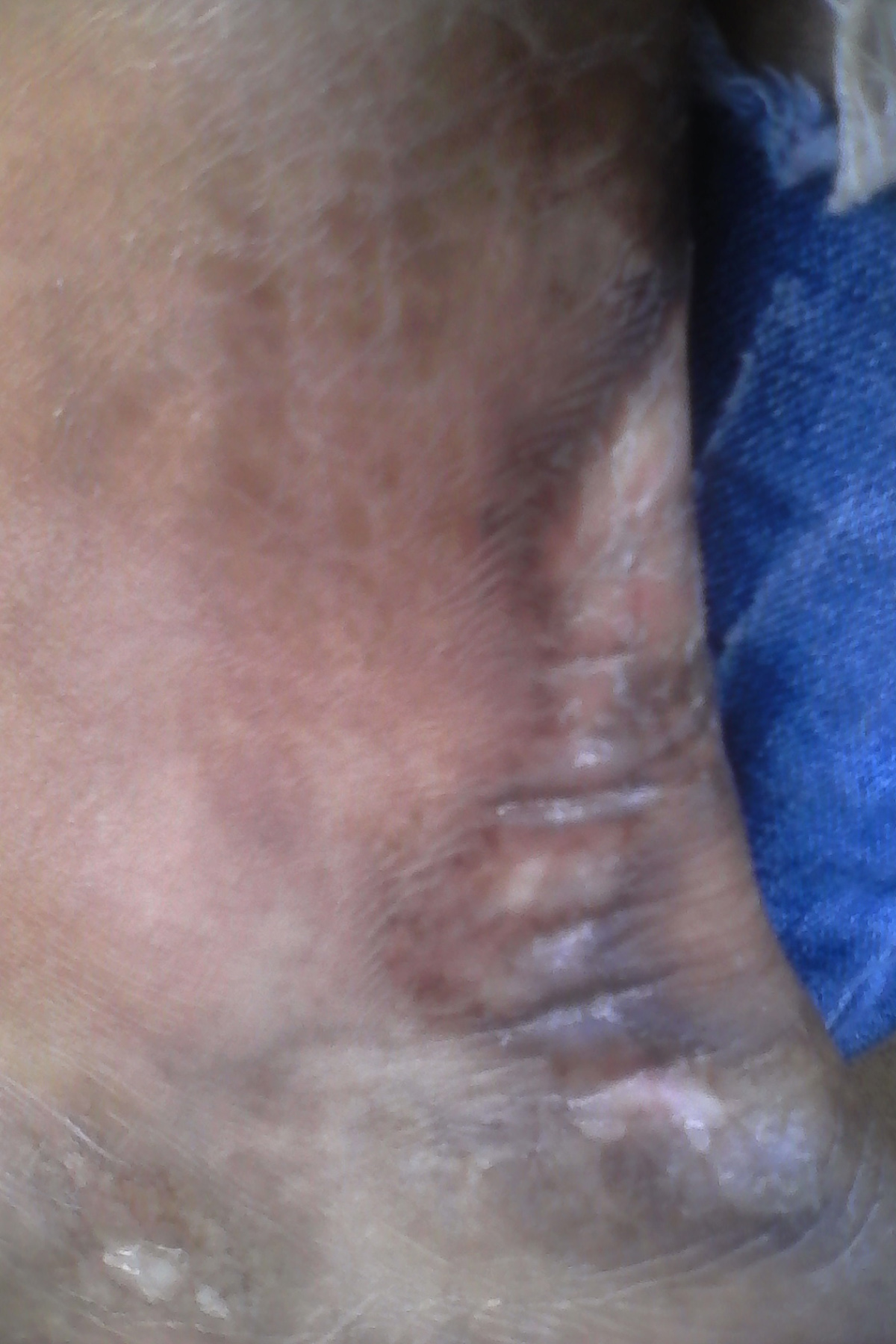
Scleroderma is a Chronic Systemic Autoimmune Disease
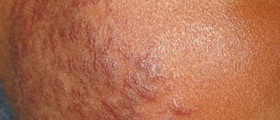
Scleroderma is a condition affecting connective tissue throughout the body as a result of certain changes in the immune system. The disease is classified as autoimmune meaning that the body attacks its own, healthy cells. Progression of the disease is associated with changes affecting the skin and blood vessels which may eventually cause serious health problems and complications.
Localized Scleroderma and Systemic Scleroderma
Scleroderma is basically classified into two major forms, limited systemic scleroderma and diffuse systemic scleroderma.
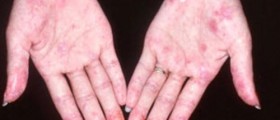
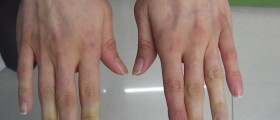
In patients suffering from limited systemic scleroderma, the only body parts affected by characteristic changes are the arms, hands and face. This form of the disease used to be referred as CREST syndrome. CREST is the abbreviation for specific complications connected to scleroderma which include calcinosis, Raynaud's phenomenon, dysfunction of the esophagus, sclerodactyly and telangiectasias. In spite of all the mentioned health issues such patients typically develop, they are also prone to pulmonary arterial hypertension, the most severe complications of the disease. It is estimated that hypertension of this type occurs in approximately one-third of all patients.
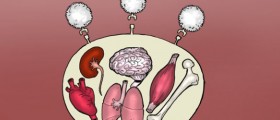
As for diffuse systemic scleroderma there are specific skin changes that rapidly affect large portions of the skin. Additionally, the process of sclerosis affects internal organs interfering with their function. In the majority of cases the condition leads to sclerosis of the kidneys and esophagus although the heart and lungs may be affected as well. This is a severe form of the disease, eventually making patients disabled.
There are also several more forms of the disease. Some are not characterized by skin changes at all. Instead there are only systemic manifestations of the disease. It is also possible for the disease to remain localized onto the skin which is the case in morphea and linera scleroderma.
Patients suffering from scleroderma who have developed heart complications basically have to deal high blood pressure, irregular heart rhythm and heart enlargement with associated heart failure. Furthermore, scleroderma of the kidneys may trigger malignant hypertension and acute renal failure. Sclerosis of the lungs is connected with breathing issues such as shortness of breath, breathing difficulty and cough. Pneumonia, alveolitis and cancer may occur as well. Digestive complications include difficulty swallowing, acid reflux, gastric antral vascular ectasia, diarrhea and weight loss.
Medicines Used to Treat Scleroderma
Scleroderma is incurable. However, with certain drugs progression of the disease and current symptoms and signs may be successfully brought under control. Complications are inevitable and their severity practically determines disability. Therefore, disability is individual, varying from patient to patient.
Since scientists have not managed to identify the actual cause and trigger of scleroderma the treatment is basically individual and adjusted to each and every patient. The goal is to alleviate symptoms as much as possible. Patients in whom Raynaud's phenomenon significantly interferes with circulation are supposed to take agents that efficiently increase blood flow to peripheral organs i.e. hands and fingers. These include nifedipine, amlodipine, diltiazem and felodipine.
Sclerosis affecting the skin is progressive. The course of the disease may be decelerated with D-penicillamine, cochicine, PUVA (psoralen + UVA treatment) or relaxin. Cyclosporine is a powerful immunomodulating agent administered in case of severe scleroderma.
Abnormal and intensive reaction of the immune system and subsequent damage to many organs is reduced with the assistance of several more immunosuppressive agents such as methotrexate, cyclophosphamide, azathioprine and mycophenolate.
Relevant Data
It may sound amazing but data regarding skin conditions that resemble scleroderma may be found in documents written by Hippocrates. These date back to 460-370 BC. There are several more findings dating back to 325-690 AD written by Oribasius and Paulus Agineta. The description of the skin conditions were not so precise so we simply cannot be sure that patients were at that time actually suffering from the same disease.
Today scleroderma affects all races and people all around the world. Still, women seem to be affected more. In the United States the condition is reported to occur in 1 out of 1,000 people. Children can develop scleroderma as well but they tend to have localized form of the disease rarely progressing into systemic sclerosis. In adults scleroderma usually occurs between the age of 30 and 50.
When it comes to prognosis, it is best in case of morphea and other limited forms of the disease. Such patients die either a natural death or due to other medical conditions and their complications. The prognosis is, however, not so good for patients with systemic form of the disease when more than one internal organ is affected. Even though the condition predominantly affects women, men are more prone to complications and die more. It is estimated that after being diagnosed most patients with limited disease may live 20-50 years while those with rapid progression and systemic, diffuse scleroderma have 50% to stay alive within the following 5 years. Lethal outcome is many times a consequence of pulmonary, kidney or heart complications.


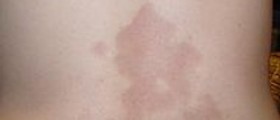
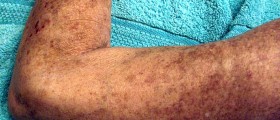






Your thoughts on this
Loading...