Jock itch is a skin condition that affects the skin on and around the crotch. It mostly affects men although it can be seen in women too.
What is Jock Itch?
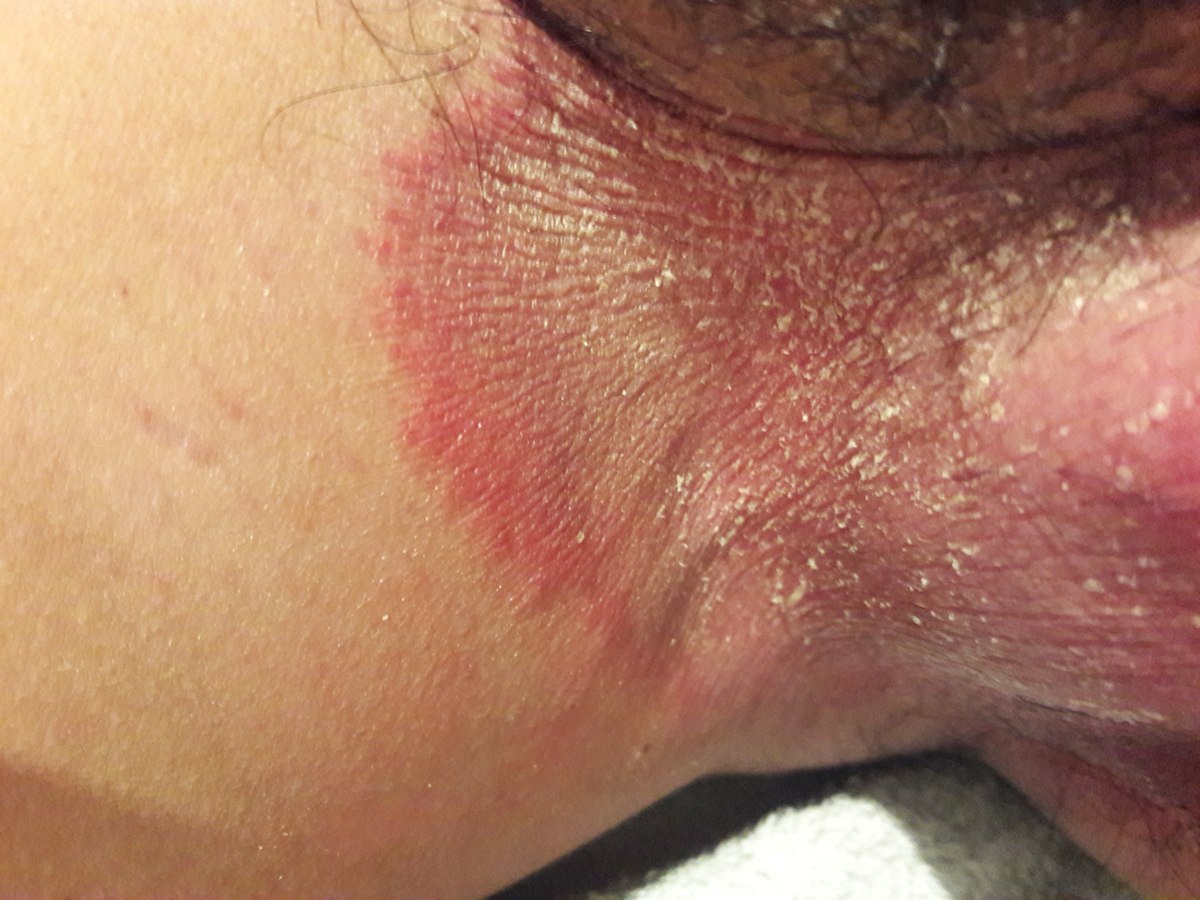
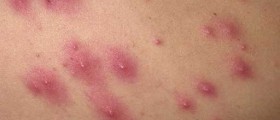
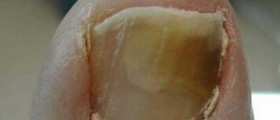
Jock itch is a fungal infection of the skin, also known as tinea cruris. Some people also call it crotch itch, crotch rot, and gym itch. It appears in the groin area and involves symptoms like itching, burning, tingling, redness, rash, flaking cracking, or rippling skin. It can even develop small boils and pustules. Jock itch can extend from the groin to the thighs, skin folds, and buttocks.
As previously mentioned, jock itch is more often seen in men than in women. The fungus that causes it prefers dark, moist, and warm environments, much like the one created in the groin area when the clothes are on. It is often seen in athletes because when they work out in their mostly synthetic sports garments, they tend to sweat more, which creates a favorable ground for the fungus to thrive.
Treatment for Jock Itch
The first line of defense against jock itch is, like in many other conditions, prevention. Athletes, people who exercise a lot, and others who are prone to jock itch, should make sure to maintain proper hygiene in the area. They should shower immediately after workouts and dry the groin area carefully and thoroughly. The clothes should be made of breathable materials, such as cotton, and not synthetic blends. It also helps to put some baby powder on the area after it is dry.
Those who already have jock itch should make sure to sleep in light and loose clothes, the ones that do not cling to the groin. Sleeping nude or near a fan exposes the area to fresh air and greatly improves the condition.
If jock itch is in full swing, it is recommended to try one of many over-the-counter antifungal ointments that are available in drugstores. Active ingredients in these creams and ointments prevent the fungus from producing a substance called ergosterol. Without ergosterol, the fungus cannot survive.
Other medications that can be applied include Hydrocortisone creams that relieve the itching and redness while antifungal ointments do their job of killing the fungus.
- We searched the following databases up to 13th August 2013: the Cochrane Skin Group Specialised Register, CENTRAL in The Cochrane Library (2013, Issue 7), MEDLINE (from 1946), EMBASE (from 1974), and LILACS (from 1982). We also searched five trials registers, and checked the reference lists of included and excluded studies for further references to relevant randomised controlled trials. We handsearched the journal Mycoses from 1957 to 1990.
- Of the 364 records identified, 129 studies with 18,086 participants met the inclusion criteria. Half of the studies were judged at high risk of bias with the remainder judged at unclear risk. A wide range of different comparisons were evaluated across the 129 studies, 92 in total, with azoles accounting for the majority of the interventions. Treatment duration varied from one week to two months, but in most studies this was two to four weeks.
- The length of follow?up varied from one week to six months. Sixty?three studies contained no usable or retrievable data mainly due to the lack of separate data for different tinea infections. Mycological and clinical cure were assessed in the majority of studies, along with adverse effects. Less than half of the studies assessed disease relapse, and hardly any of them assessed duration until clinical cure, or participant?judged cure. The quality of the body of evidence was rated as low to very low for the different outcomes.
- Data for several outcomes for two individual treatments were pooled. Across five studies, significantly higher clinical cure rates were seen in participants treated with terbinafine compared to placebo (risk ratio (RR) 4.51, 95% confidence interval (CI) 3.10 to 6.56, number needed to treat (NNT) 3, 95% CI 2 to 4). The quality of evidence for this outcome was rated as low. Data for mycological cure for terbinafine could not be pooled due to substantial heterogeneity.
- Mycological cure rates favoured naftifine 1% compared to placebo across three studies (RR 2.38, 95% CI 1.80 to 3.14, NNT 3, 95% CI 2 to 4) with the quality of evidence rated as low. In one study, naftifine 1% was more effective than placebo in achieving clinical cure (RR 2.42, 95% CI 1.41 to 4.16, NNT 3, 95% CI 2 to 5) with the quality of evidence rated as low.
- Data for several outcomes were pooled for three comparisons between different classes of treatment. There was no difference in mycological cure between azoles and benzylamines (RR 1.01, 95% CI 0.94 to 1.07). The quality of the evidence was rated as low for this comparison. Substantial heterogeneity precluded the pooling of data for mycological and clinical cure when comparing azoles and allylamines. Azoles were slightly less effective in achieving clinical cure compared to azole and steroid combination creams immediately at the end of treatment (RR 0.67, 95% CI 0.53 to 0.84, NNT 6, 95% CI 5 to 13), but there was no difference in mycological cure rate (RR 0.99, 95% CI 0.93 to 1.05). The quality of evidence for these two outcomes was rated as low for mycological cure and very low for clinical cure.
- All of the treatments that were examined appeared to be effective, but most comparisons were evaluated in single studies. There was no evidence for a difference in cure rates between tinea cruris and tinea corporis. Adverse effects were minimal ? mainly irritation and burning; results were generally imprecise between active interventions and placebo, and between different classes of treatment.
Sometimes antifungal medication purchased in drugstores is not strong enough to solve the infection and it is necessary to see a doctor who will prescribe stronger medications. Jock itch should not be neglected or left untreated, because it can spread and become even more difficult to treat.









-Causes,-Symptoms-And-Diagnosis_f_280x120.jpg)



Your thoughts on this
Loading...