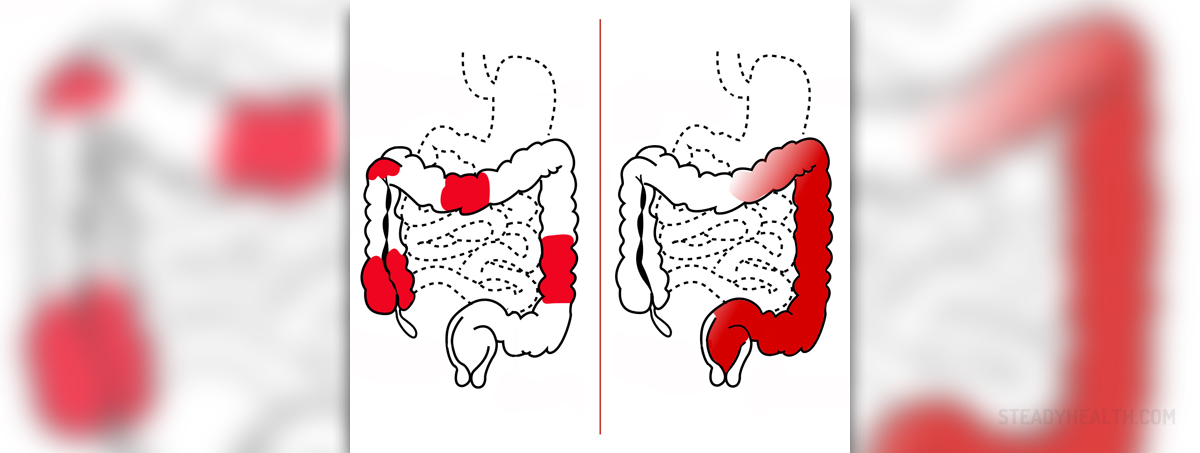
Ulcerative colitis is a chronic inflammatory bowel disease. Inflammatory changes affect the lining of colon and rectum. The clinical course of disease is characterized by changing of worsening symptoms periods and stages without symptoms.
Symptoms
At the beginning symptoms usually appear gradually, almost always with bloody-mucous diarrhea of varying severity. Most patients feel good at the beginning of the disease. Later signs may be pallor, weight loss, abdominal pain to the touch and finding blood in the colon during digitorectal examination.Treatment
The initial therapeutic approach depends on the severity of the disease. Inflammation of the final part of the colon (proctitis) is initially treated with local application of 5-aminosalicylic acid (mesalazine or steroids). Mesalazine enema or suppositories take precedence over the local application of steroids.Ulcerative proctitis also includes application of tablets or capsules Sulfasalazine and various oral 5-ASA formulations. Symptomatic improvement is usually seen after three or four weeks. When the remission is achieved, the medication dose can be gradually reduced to maintenance dose.
Systematic use of corticosteroids or immunosuppressive therapy is rarely needed in patients with ulcerative proctitis. Left-sided colitis may respond to topical medications, but more often it is necessary to include oral therapy. Treatment varies depending on the condition severity. Therapy, for mild to moderate severity of illness, can be started with mesalazine in standard doses. Therapeutic response is usually expected after 4 to 6 weeks. When the remission is achieved, the dose is gradually reduced to maintenance dose. If the symptoms occur again, despite taking maintenance therapy, higher doses of medication are needed to prevent their repetition. Supplementation of folic acid is recommended for patients who are on long-term sulphasalazine therapy because this drug acts as antimetabolites of folic acid. Corticosteroids are used for treating severe ulcerative colitis. The initial dose depends on the patients weight and severity of symptoms. Starting dose is gradually decreased after ten to fourteen days.
Immunosuppressive therapy is introduced in patients who do not show a good response to the offered treatment options. Pancolitis with mild to moderately severe clinical manifestation is treated with a combination of oral mesalazine or sulphasalazine and mesalazine topical therapy. The use of corticosteroid therapy should last not longer than three months.
Immunosuppressants such as azathioprine can be very effective in the treatment of ulcerative colitis.
Continuous disease activity, resistance to corticosteroids or immunosuppressive therapy inefficiency, may indicate use of anti TNF therapy in the treatment of ulcerative colitis. Severe or fulminant colitis - treatment begins with parenteral systemic corticosteroids, with full implementation of supportive therapy that includes infusion solutions and antibiotics. The possible beneficial effect of local enema therapy in this difficult clinical situation shouldn't be ignored.
In very difficult situations when the occurrence of toxic megacolon is possible, there is a therapeutic option of anti TNF therapy (infliximab) or Cyclosporine.
Patients, whose colon is extended six centimeters or more and have toxic symptoms and who do not respond to the treatment with corticosteroids, Cyclosporine or infliximab, are potential candidates for surgery. The surgery is known as proctocolectomy with possible ileostomy during the surgery or later.
Nutrition
Nutrition plays an important role in patients with inflammatory bowel disease. Adequate micronutrients supply (vitamins and minerals) is particularly important, since deficiencies frequently occur in patients with ulcerative colitis. The most important tip for most patients is to consume adequate amounts of protein and have an adequate energy intake to maintain desirable body weight.There are indications that the health condition may be improved if the patients, who suffer from ulcerative colitis, follow the diets low in simple sugars or have hypoallergenic diet.











Your thoughts on this
Loading...