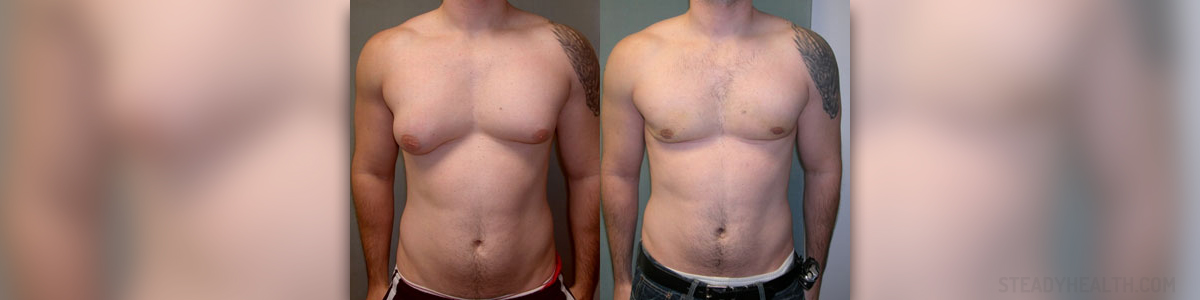
Gynecomastia is a sort of benign enlargement of the male breast. It can cause proliferation of its glandular component. It is determined by a rubbery or firm mass extending from the nipples in a concentric fashion. Gynecomastia is usually bilateral, but there are cases of unilateral occurrences.
This condition is caused by an altered estrogen-androgen balance, in favor of estrogen. It can also result from increased breast sensitivity to normal circulating estrogen. Estrogen induces ductal epithelial hyperplasia, ductal elongation and branching, proliferation of the periductal fibroblasts, and an increase in vascularity. This access estrogen is usually caused by a peripheral conversion of androgens through the function of the aromatize enzyme. This transpires mostly in muscles, skin and adipose tissue. The androgens are converted to estradiol and estrone.
Normally, the ratio of testosterone to estrogen production should be around 100:1, rising to 300:1 in circulation.
Gynecomastia is the most common reason for male breast evaluation. This condition commonly appears in infancy and adolescence, but it can happen in middle-aged males as well. When it presents in infants, the reason is usually high estrogen levels experienced in pregnancy. This makes the gynecomastia transient.
During puberty, a transient increase in estradiol is noticed in boys who develop this condition. It usually presents itself between 10-12 years of age and tends to regress within 18 months. Persistence of the condition is fairly uncommon.
When manifesting in older males, it is often multifactorial. The reason most often found to be decisive in inducing this condition is that of an increased aromatization of testosterone to estradiol, as well as the gradual decrease of testosterone levels. Older males are also more prone to taking medications associated with gynecomastia. The following etiologies are estimated when considering males who seek medical attention for gynecomastia:
Persistent pubertal gynecomastia – 25 percent Drugs – 10-25 percent No detectable abnormality – 25 percent Cirrhosis or malnutrition – 8 percent Primary hypogonadism – 8 percent Testicular tumors – 3 percent Secondary hypogonadism – 2 percent Hyperthyroidism - 1.5 percent Chronic renal insufficiency – 1 percentTreatment is mostly obsolete when it comes to gynecomastia. Still, when choosing a method, a major factor should be the duration of the condition.
After 12 months or longer, it is highly unlikely that medical therapy will induce any regressive behavior. Thus medical therapy should only be implemented in early stages.
Pubertal gynecomastia will eventually resolve itself. The process often takes no more than three years. If the enlargement is greater than four centimeters in diameter, it may not fully regress.
A reduction mammoplasty is a surgical procedure considered when the patient has a long-term gynecomastia or a macroplastia. It may also be done on patients for whom medical therapy failed. Aesthetics are also a reason to subject one’s self to this intervention. More extensive plastic surgery is recommended in patients with marked gynecomastia. Those who have developed excessive breast-sagging (usually caused by weight loss) are also subject to this procedure.
Complications include tissue-sloughing, contour irregularity, hematoma/sarcoma formation and permanent numbness in the nipple area.














Your thoughts on this
Loading...