
What is Lumbar Puncture?
A lumbar puncture also known under the name spinal tap is a powerful diagnostic and therapeutic tool. It allows doctors to collect samples of cerebrospinal fluid which are then sent for biochemical, microbiological and cytological analysis. Also, by removing the excess of such fluid doctors can successfully reduce increased intracranial pressure.
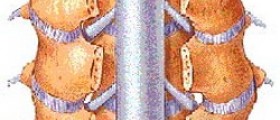
Cerebrospinal fluid is under normal circumstances a colorless fluid. It circulates around the brain (and goes through brain ventricles) and the spinal cord nourishing these organs and cushioning them. In case of brain or spinal cord infections or other medical conditions the components of cerebrospinal fluid change or its regular components increase in the amount. Such changes are sufficient enough to help doctors diagnose the underlying problem.
Why is Lumbar Puncture Performed?
In the majority of cases a lumbar puncture is performed to confirm or rule out meningitis, inflammation of the brain's membranes. For instance, this is a routinely performed procedure in infants who have fever of unknown origin because they are highly likely to develop meningitis and show no typical signs of the infection (irritation of the meninges-meningismus). However, in older patients meningitis leads to typical symptoms and signs such as headaches, light sensitivity, drowsiness, confusion and sometimes skin rash. By performing lumbar puncture doctors can identify culprits of meningitis if it is bacterial in origin or specific changes in the level of substances normally found in cerebrospinal fluid in case one is suffering from viral meningitis.
Furthermore, this diagnostic procedure is of utmost importance in case of subarachnoid hemorrhage, hydrocephalus and benign intracranial hypertension. Subarachnoid hemorrhage generally develops as a result of stroke. This is a medical emergency which may easily trigger severe brain damage, cause neurological sequelae and even death. By performing a spinal tap doctors easily confirm the presence of blood in cerebrospinal fluid and can easily confirm subarachnoid hemorrhage.
Additionally, by examining samples of cerebrospinal fluid doctors can also identify cancer cells which points to the presence of metastases of various tumors, both those that primarily affect the brain and the spinal cord and others that originate from other organs in the body.
A lumbar puncture is also efficient in diagnosing Guillain-Barré syndrome. Namely, the level of protein in cerebrospinal fluid is much higher in individuals suffering from this syndrome compared to healthy individuals.
And finally, a spinal tap is an excellent means of administrating certain drugs right into cerebrospinal fluid. This is necessary when the drug itself cannot pass the blood-cerebrospinal fluid barrier because of its molecular characteristics. For instance, such approach is used for the purpose of spinal anesthesia. Also, certain chemotherapeutics that need to reach the brain or be distributed along the spinal cord are administered in such a way.
Still, even though some individuals may actually require a spinal tap there might be contraindications for the procedure. For instance, a lumbar puncture is never performed if an increase in intracranial pressure is idiopathic i.e. its underlying cause is not identified. Also, if there is an increase of this type a spinal tap may precipitate uncal herniation and make matter worse. Precautionary measures are of major importance when the procedure is done in people over 65 years of age, patients with reduced GCS or conscious state as well as those with recent history of seizures. A lumbar puncture is also contraindicated in people suffering from coagulopathies and those with decreased platelet count, patients with infection at the puncture site and those with confirmed sepsis. The presence of abnormal respiratory pattern, elevated blood pressure with bradycardia and vertebral deformities are all additional contraindications for lumbar puncture.
How is Lumbar Puncture Performed?
Patients who undergo lumbar puncture should be placed in a left/right lateral position. The neck is supposed to be bent in full flexion and the knees bent in full flexion as well towards the chest cavity. Some patients may sit on a stool and bend their entire upper portion of the body forward. The site of the puncture is first prepared with the assistance of aseptic technique and local anesthetics and once the doctor opts for the appropriate location he/she inserts the spinal needle, pushes it until it pierce the dura matter which is characterized by dripping of cerebrospinal fluid through the inserted needle. While the needle is still in the subarachnoid space doctors collect samples of cerebrospinal fluid. In the end the needle is withdrawn and doctors apply pressure on the injection site. After the procedure patients may be asked to lie on their back and remain in the position for approximately 6 hours while doctors in the meantime check for the presence of any neurological abnormalities even though this is actually out-of-date approach currently choosen by small number of doctors.
The entire procedure takes about 45 minutes, is not painful and is also relatively safe. The most commonly reported side effect is headache which affects around one-third of all patients and develops a day or two after the procedure. In spite of this potential side effect doctors opt for spinal tap many times and perform it impeccably hoping that it will help them find the underlying causes of conditions their patients are suffering from.


_f_280x120.jpg)








Your thoughts on this
Loading...