Defining the theoretical framework and the term
The NHS, i.e. the United Kingdom National Health Service, provided the general public with the one definition that states what clinical governance represents exactly. The definition is aimed at embodying three most vital attributes, and those three attributes are:
Acclaimed and affirmed high standards of the health care Transparent responsibility and accountability for those standards Constant dynamic of the improvementConstituents most vital
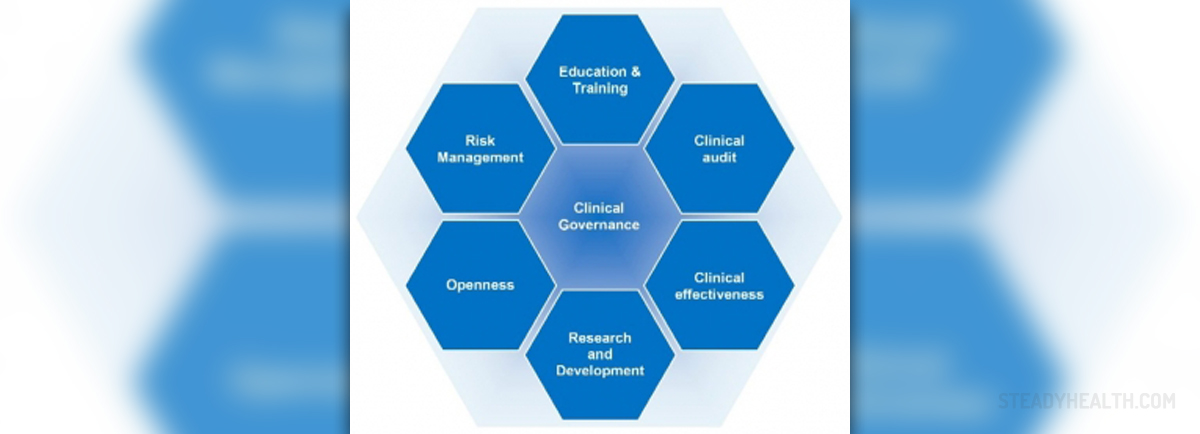
The framework in question is known to be comprised of at least the following important constituents:
Education and training. The special emphasis is on continuing education, which means that each and every clinician ought not to refrain from continuous education after qualification. Clinical audit. This refers to the review of clinical performance, as well as to the refining and improvement of clinical practice as a result and the measurement of performance against agreed standards. Clinical effectiveness. It concerns the overall measurement of the extent to which a particular intervention is effective and functions in a manner most proper. Research and development. A proper professional practice has always been in favor of introducing the changes that represent the embodiment of those most recent and up to date pieces of evidence acquired by way of research and research studies. Openness. Those processes that are available and open to the “inspection” of the public, with paying special attention to the status of a patient and practitioner, confidentiality represent a vital part of most beneficial and quality assurance. Risk management. It refers to the close inspection of the following aspects – the risks for patients, risks for practitioners and risks for the organization in question.



-Test-And-What-Do-The-Results-Mean_f_280x120.jpg)






Your thoughts on this
Loading...