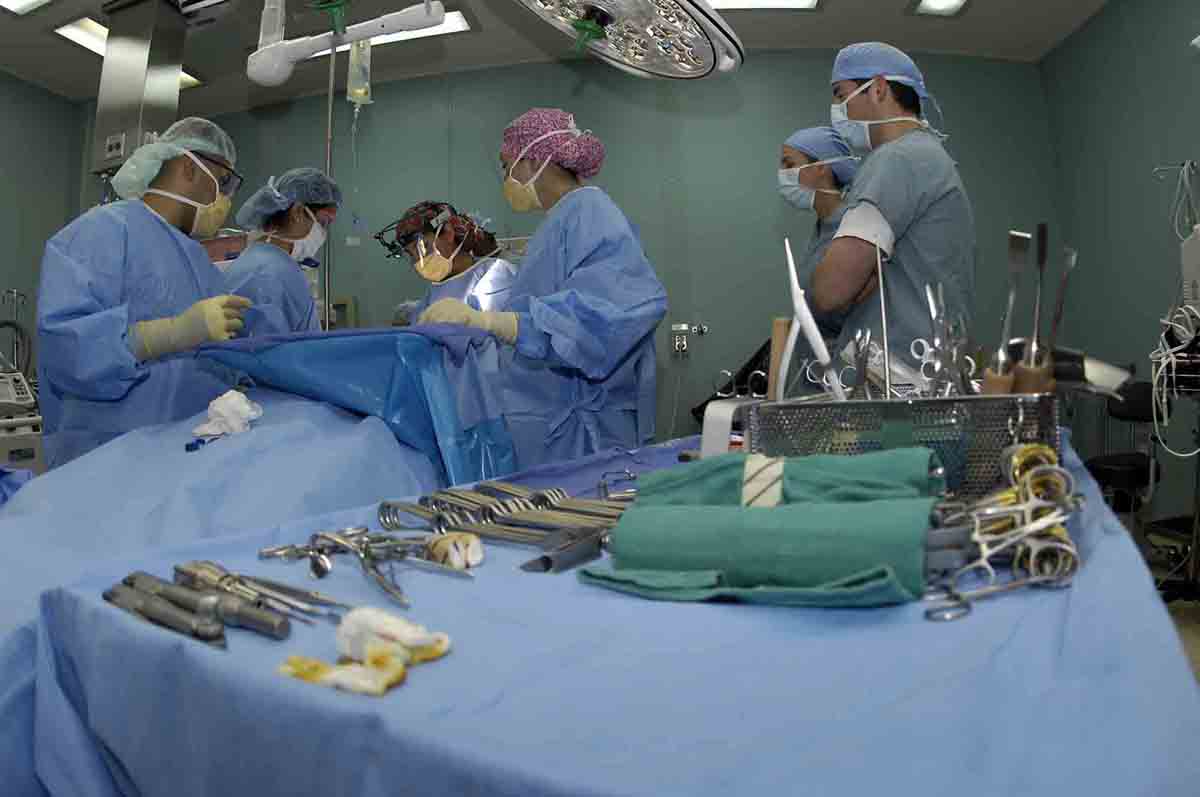
Rectal ProlapseRectal prolapse is a condition in which walls of rectum protrude through the anus. A rectocele occurs when the rectum pushes through the back wall of the vagina. Both of these conditions may be result of chronic constipation or habit of straining to have bowel movements. Also, rectocele may occur as a consequence of childbirth process.
Rectal prolapse and rectocele are associated with the following symptoms:ConstipationPain and discomfort during bowel movementsMucus or blood discharge from the protruding tissueLoss of urge to defecateFecal incontinence (inability to control bowel movements)Treatment depends on severity of the case, but generally without surgery most prolapsed rectums become worse. Operation can be done through abdomen, vagina or the anus.
Surgery for Prolapsed RectumThe day before the surgery, patient will need to fast and drink special liquid to clean out intestines. When arrives to the hospital, a patient will be prepared for general anesthesia. The procedure involves following techniques of performing rectal prolapse.
LaparotomyLaparotomy is an open abdominal surgery. This procedure includes one large incision in the abdomen. Surgeon carefully moves away organs to get to the rectum. The rectum is then lifted and stitched to the sacrum. Sometimes, surgeon may also shorten the bowel.
LaparoscopyLaparoscopy is a keyhole abdominal or telescopic surgery. This procedure is followed by less painful and shorter recovery. Through several small incisions in the abdomen, surgeon inserts instruments and repairs prolapsed rectum.
Anal surgery
Anal surgery is performed via anus under anesthesia. Surgeon removes part of prolapsed bowel and the rest of it returns through the anus in order to restore function and appearance. This method is recommended for elderly patients.
Procedure for RectoceleThis surgery can be done through the vagina, the anus, the abdomen or the perineum. Regardless of used methods, surgeon aims to restore the wall between rectum and the vagina. Procedure involves incisions in the back wall of the vagina. Pelvic floor muscles and perineum (if necessary) are repaired with absorbable stitches. Afterward, vagina is stitched and urinary catheter is placed.
RecoveryAfter the procedure, patient’s temperature, pulse and blood pressure is closely monitored. Patient receives IV fluids and pain-killers. Urinary catheter remains inserted until a patient restores the ability to urinate on their own. Patient stays in hospital 3 to 6 days after the surgery. Once at home, a patient should have plenty of rest, avoid straining, avoid foods that cause constipation and drink plenty of water.
ComplicationsThere are several possible complications of the surgery such as: hemorrhage, infection, bladder or rectum damages, allergic reaction to anesthetic, necrosis of the rectal wall and recurrence of prolapsed rectum.










Your thoughts on this
Loading...