Modern times bring modern approaches to medicine. Continual improvements in knowledge, technology and chemistry reveal new possibilities when it comes to spine surgery. Procedures become less and less invasive, with lesser risks and even lesser recuperation. This is also true for cervical radiculopathy.
It is believed that the treatment of cervical radiculopathy by the posterior approach is, in most cases, better than the anterior discectomy and fusion technique. Among others, the main reason for this could be that a laminectomy (spine operation, involving the removal of a portion of a vertebral bone – lamina) doesn't result in instability. This excludes the need for a cervical collar and the patient is able to function much sooner after the surgical intervention. This treatment is also cost-effective, avoids unnecessary scaring and additional wear and tear on the joints which is a side effect of the fusion technique.
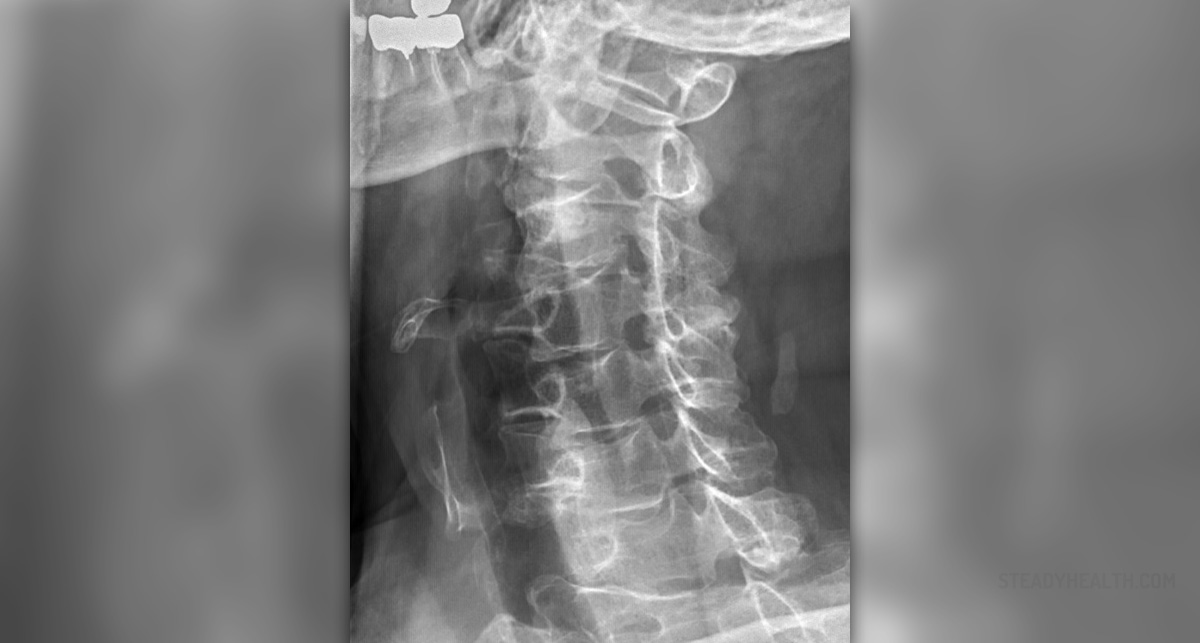
Cervical radiculopathy is a condition where one of the spinal nerve roots in the neck gets irritated and compressed. These nerve roots can be found in the spinal canal and the neuroforamen (openings between two vertebrae where nerve roots exit the spinal column).
There are many reasons why a nerve root might get irritated, but what is important is the possible consequences of the irritation itself. These include a number of sensory or motor inconsistencies, including pain, tingling, numbness (sensory), weakness or loss of reflex (motor). These symptoms may appear in the neck, shoulders, arms, hands and fingers.
Depending on the cause of the ailment, one of the first steps may include a non-surgical treatment. This could be administered through the use of medication or physical therapy. Still, in many cases surgery is the only answer.
There was a study involving 502 patients suffering from this condition. 200 of these 502 chose to have an "outpatient" spine surgery. These were performed under general anesthesia through the posterior approach. A laminoforaminotomy was implemented at affected areas. This procedure allows access to the affected nerve roots.
The patients were monitored for several hours after the surgery. They were discharged when they met the criteria needed. None of the patients stayed for recuperation, and out of the 200, 183 patients followed up for 19 months on average.
Compared with patients who were hospitalized afterwards, the outcomes did not differ a great deal. The study showed that the procedure itself is safe, with no signs of infections or major complications.
Taking into account the fact that not all patients are eligible for cervical radiculopathy, the results of the study are still very encouraging. They present a positive environment, free of unnecessary risks, which is a great basis for further improvements.


-Causes,-Symptoms,-Diagnosis,-Treatment_f_280x120.jpg)




Your thoughts on this
Loading...