
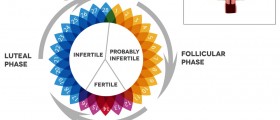
A short luteal phase is the most common reason behind recurrent miscarriage In order to correctly diagnose the problem a woman may need to chart her basal body temperature and chart her ovulation patterns for a few months and then consult with a medical professional to be tested. If a physician suspects a luteal phase defect, the woman will need to have a serum progesterone test to check the amounts in the body. The test is performed within 7 days after ovulation and is done via blood test to check levels of progesterone. If results are lower than normal, the doctor will then prescribe short luteal phase treatment options to correct the condition. Treatment for a short luteal phase could include progesterone supplementation during the luteal phase if it is determined that follicle development is normal.
Other protocols for treating a short luteal phase may include ovarian stimulation to induce better hormone production, one drug used is Clomid which tricks the body into thinking there is an estrogen shortage. Some physicians may also suggest the woman receives injections of human Chorionic gonadotropin which is done to stimulate the corpus luteum further. One downfall of HCG injections is that it will cause a false-positive result on a pregnancy test, which can be frustrating for a woman to deal with. Luteal phase defects are fairly common disorders and finding out the exact cause behind the problem is something currently being researched. Once the condition has been definitively diagnosed, a woman can consult with her physician in order to determine what the best course of action should be.
- www.betterhealth.vic.gov.au/health/conditionsandtreatments/menstrual-cycle
- www.who.int/selection_medicines/committees/expert/18/applications/Norethisterone.pdf
- Photo courtesy of Luis Alejandro Bernal Romero by Flickr: www.flickr.com/photos/aztlek/5823194366/











Your thoughts on this
Loading...