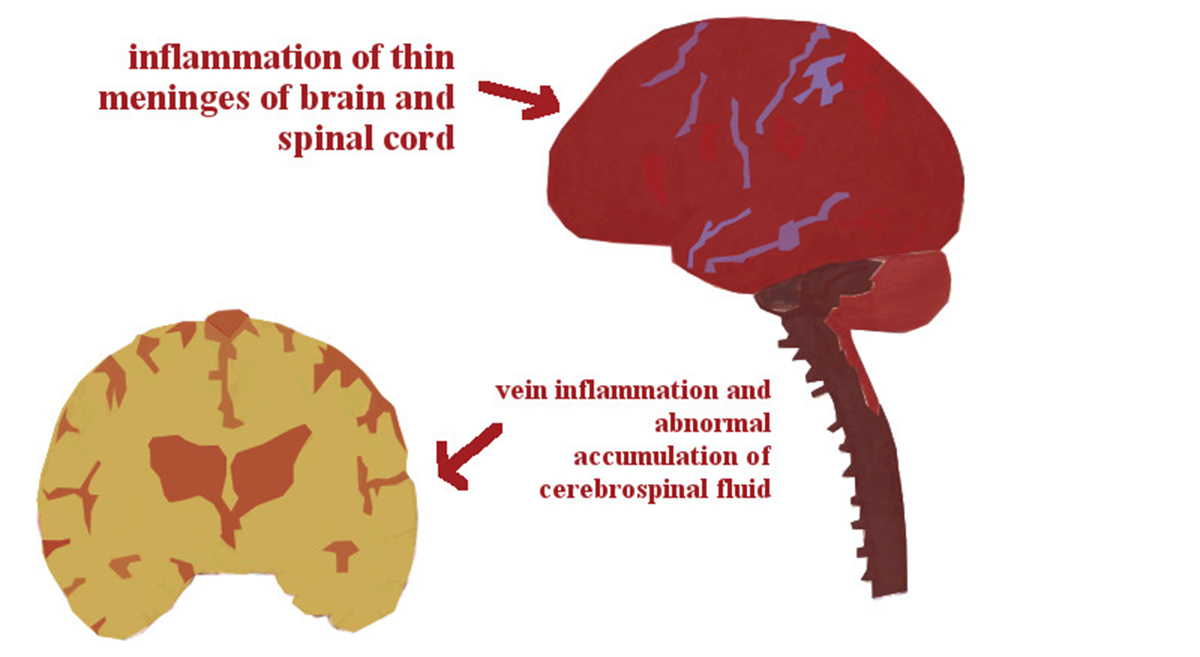
Bacterial meningitis is inflammation of the meninges (the membrane that surrounds the brain and the spinal cord) caused by different bacteria. Apart from bacterial meningitis people may also develop viral meningitis and, as the very name suggests, in this case the infection is caused by certain viruses. Unlike viral meningitis, which is usually mild and not associated with serious complications, bacterial meningitis can be quite severe and cause serious consequences including death.
Different Bacteria as Culprits of Meningitis
Bacterial meningitis is commonly caused by three types of bacteria including Haemophilus influenzae type b, Neisseria meningitidis and Streptococcus pneumoniae. Today among three of these infective agents Neisseria meningitidis and Streptococcus pneumoniae represent the main culprits of bacterial meningitis. It is essential to confirm the type of bacteria responsible for the infection. This way the most suitable antibiotic will be chosen for the treatment.
Spread of the Infection
Bacterial meningitis affects people all around the world. The bacteria normally enter one's body through the mouth and the nasal cavity and form there reach the meninges either directly by affecting the nearby structures firstly or indirectly when microorganisms are transferred via blood. The infective agents are easily transmitted during a close contact with the infected person. Bacteria spread with discharge from the nose and throat.
Clinical Characteristics of Bacterial Meningitis
Typical symptoms in people suffering from bacterial meningitis include fever, headache and stiff neck. These symptoms may develop over several hours or a few days. Additional symptoms and signs include nausea and vomiting, increased sensitivity to light (photophobia), confusion and sleepiness. Skin rash usually affects patients suffering from meningococcal meningitis. Newborns and infants with meningitis develop fever, headache and they also have stiff neck. They are inactive, irritable and refuse to eat. Progression of the infection may eventually cause seizures. Potential complications of bacterial meningitis include encephalitis, severe brain damage, coma and death. Survivors from severe from of the infection may end up with hearing loss, mental retardation, paralysis and other neurological sequelae.Treatment and Prevention of Bacterial MeningitisThe cornerstone of treatment for bacterial meningitis are antibiotics. Patients suffering from seizures are additionally treated with antiepileptics and symptomatic treatment generally accompanies the basic treatment with antibiotics.
It is possible to prevent bacterial meningitis. This is achieved with several vaccines. People can be vaccinated against Haemophilus influenzae, some strains of Neisseria meningitidis and different types of Streptococcus pneumoniae. Vaccination against Haemophilus influenzae is repeated at least three times until the child turns 6 months and the fourth dose is administered between 12 and 18 months of age. Vaccine against meningococcal meningitis is not routinely prescribed especially in children under the age of 2 (in them the vaccine is usually ineffective). Such vaccines are still under investigation and development. And finally, the vaccine against streptococcal meningitis is recommended in people older than 65 years of age and younger individuals with certain health issues. Each case of bacterial meningitis must be reported to state or local health authorities and people with close contact with the infected person are administered antibiotics prophylactically.










Your thoughts on this
Loading...