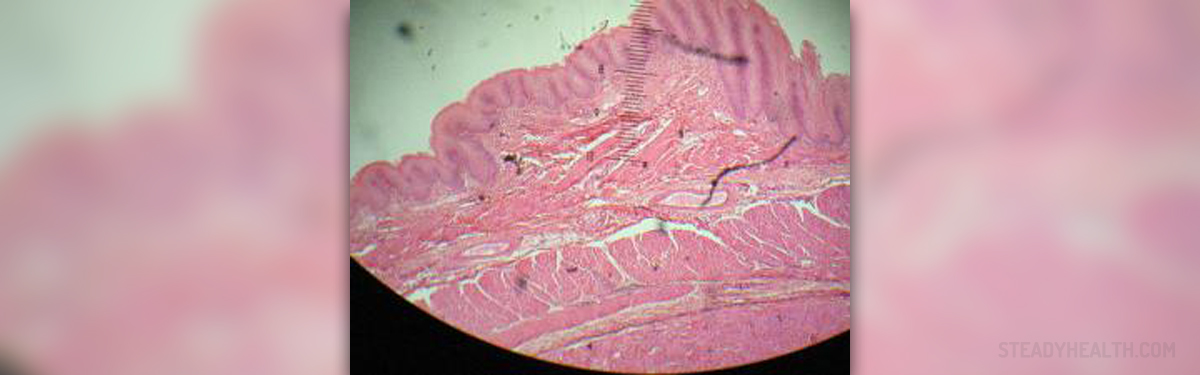
Barrett’s esophagus, also known as Barrett’s syndrome or columnar epithelium lined lower esophagus is the disease distinguished by an abnormal change in the cells of the inferior portion of the esophagus. In this disease the esophagus, a tube that carries the food from the throat to the stomach, becomes damaged by stomach acids. Color and composition of the cells lining the lower esophagus change and start to resemble the lining of the intestine. Barrett’s esophagus is a serious health problem, considered to be a premalignant condition because it is associated with increased risk of esophageal cancer.
Risk factors
This disease is common in people with gastro-intestinal reflux disease, also known as GERD. However, having GERD doesn’t necessarily mean the patient is going to develop Barrett’s esophagus. Factors that increase one’s risk of developing this disease are numerous. Among the most prominent factors there is a chronic heartburn and acid reflux. If a patient has these symptoms for more than 10 years, his chances of damaging the lining of the esophagus are very high. This happens because the stomach acids back up into the esophagus, causing the degenerative changes in the tissue.
Men are slightly more likely to develop this disease, especially if they are older adults, white or Hispanic.
Symptoms of Barrett’s esophagus
Barrett’s esophagus is diagnosed in about 5 to 15% of all patients who complain about heartburn. The interesting thing is that a large portion of these patients has no symptoms of the disease. However, a number of symptoms may point out to the development of Barrett’s esophagus: recurrent and ongoing heartburn, troubles with swallowing, vomiting coagulated blood, bloody or black stools, pain under the breastbone at the spot where esophagus ends, pain while eating, weight loss. Any kind of long-term troubles with heartburn and acid reflux is a warning sign. Symptoms such as the chest pain, difficulty swallowing, and bloody stool or vomit require immediate medical attention.
Treatment of Barrett’s esophagus
Barrett’s esophagus is normally diagnosed using endoscopy to examine esophagus and take a tissue sample. Lab tests will determine the degree of changes in the cellular tissue. People diagnosed with low-grade dysplasia or no dysplasia will be advised to take periodic endoscopy exams to monitor the changes on the cells and to continue their treatment for GERD.
If a patient is diagnosed with high-grade dysplasia, a precursor to esophageal cancer, more invasive treatments will be considered: surgery to remove esophagus, removal of the damaged cells with endoscope, using heat to remove degenerative tissue (radiofrequency ablation), or destroying damaged cells by making them sensitive to light (photodynamic therapy).













Your thoughts on this
Loading...