A herpes skin rash is a skin rash that occurs in people infected with one of the herpes viruses. The outbreaks can be primary (the first one you experience after infection) or recurring, typically when your immune system is weakened, as these viruses remain in your body in a dormant state.
There are many herpes viruses that can cause a herpes rash on different parts of the body. People are commonly affected by three types of herpes viruses. They include Herpes Simplex type I, which is responsible for cold sores and fever blisters, Herpes Simples type II, which causes herpes of the genital area, and finally, Herpes zoster which is responsible for shingles.
Cold Sores
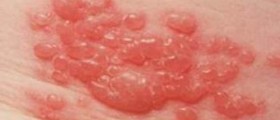
Cold sores are also known as fever blisters, and they occur in people who are infected with Herpes Simplex virus type I. This infection is very contagious. It affects the oral cavity and the face. In this case, the herpes rash typically features small blisters that occur in clusters on and around the lips.
They are filled with liquid and are rather painful. The eruption of blisters occurs spontaneously, and people who have experienced cold sores before will often be able to tell that a cold sore is coming when they experience the tell-tale tingle associated with outbreaks.
In the oral cavity, blisters rupture almost instantly due to increased moisture. The rupture leaves open sores which are very painful. Unfortunately, there is no cure for cold sores. Still, the symptoms may be alleviated by numbing agents such as phenol, Benzocaine, lidocaine, etc.
Anti-viral medications such as acyclovir, Valacyclovir are used as well since they inhibit the multiplication of viruses, but they are only effective if you catch a cold sore before it reaches the blistering stage.
Genital Herpes
Genital herpes is caused by the Herpes Simplex virus type II. This herpes virus can be easily transferred via sexual contact. Both genders can be affected. With this virus, a herpes rash also occurs in the form of blisters and may affect different parts of the male and female genitalia.
The symptoms of genital herpes vary a lot. Some people only complain about slight discomfort while others suffer from rather painful skin changes. Apart from this nasty herpes rash, genital herpes can cause additional symptoms such as fever, malaise, depression, painful urination and unusual vaginal discharge.
Similar to cold sores, genital herpes is treated with anti-viral medications best used at the very first sign of symptoms. The rash is genital herpes is more susceptible to secondary infection due to specificity of this area. It is, therefore, essential to keep the affected skin clean.
Shingles
Shingles are caused by a virus that belongs to the Herpes family even though it is not the same as Herpes Simplex virus type I and II. Shingles may develop a long time after a person has had chickenpox, to be more precise has been infected with the Varicella zoster virus. After a person has gone through chickenpox, the virus becomes latent and is located in the nerve cells.
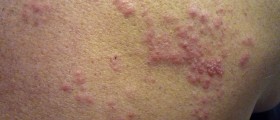
Certain conditions such as age, chronic illnesses or insufficient immunity may lead to a reactivation of the virus and the typical herpes rash for shingles occurs. It features with bumps and blisters that are located along the affected dermatome, and patients are likely to experience significant discomfort. Herpes rash in shingles is usually in the form of a belt or band, it is itchy and causes tingling or burning sensations. Even this type of herpes rash is treated with anti-viral medications. Patients may be additionally prescribed topical ointments to reduce itchiness and painkillers in case of severe pain.
- It is estimated that more than 90% of adults in the U.S. carry VZV and are at risk for the development of herpes zoster. Between 1996 and the present, the rate of VZV infection has been as high as 0.3 cases per 1,000. However, the factors that predispose certain individuals to the reactivation of infection are not clear.
- VZV reactivation increases with age. This is thought to result from the decline in virus-specific, cell-mediated immune responses that accompanies advancing age. For example, one study reported a 0.3% rate of VZV reactivation in the overall population, compared with 1.0% in persons older than age 80.
- In another population-based study, the incidence of VZV reactivation was 0.5% in people older than age 75. In a third study, the incidence exceeded 1% in persons older than 65 years of age. A second onset of disease occurs in 6% of older individuals, often after an interval of more than a decade.
- The incidence of complications, such as postherpetic neuralgia (PHN), is also a function of increasing age. The rate of PHN is almost 30% higher in people older than age 50 compared with younger individuals. In addition to advanced age, other conditions that change cell-mediated immunity can increase VZV reactivation, such as neoplastic disease (particularly involving the lymphatics), diseases that require immunosuppressive therapy (including corticosteroids), and organ transplantation.
- Reactivation of the virus is significantly more common in women than in men, especially among the elderly. There also appears to be a higher incidence of VZV reactivation in Caucasians than in non-Caucasians. In a geriatric study, 3.4% of Caucasian subjects developed herpes zoster compared with 1.4% of African-Americans.
- Injury to the dermatomes may be an important risk factor for VZV reactivation. It has been proposed that traumatic stimulation of the nerve may trigger reactivation of the virus in the dorsal root ganglion. However, because herpes zoster does not affect likely trauma sites, many trauma cases do not result in zoster flare-ups.
- Some individuals may be genetically predisposed to the development of herpes zoster. In a Scandinavian study, changes in the gene for interleukin-10 (an immune-system mediator) were associated with an increased incidence of herpes zoster. A French study supported the contention that a family history of herpes zoster correlates with an increased risk of zoster reactivation.
- Patients with herpes zoster usually present to a physician when VZV reactivates in the sensory ganglia. The initial symptoms may include malaise, generalized headache, and photophobia.5 Patients may also experience itching, tingling, and severe pain. Fever rarely occurs in the early stages of infection unless the immune system is compromised.
- Within 3 to 5 days of the initial symptoms, an erythematous maculopapular rash erupts unilaterally in the nerves of sensory dermatomes adjacent to the involved ganglia. Over the next 7 to 10 days, the rash progresses to pustules and ulceration, with crusts, scabbing, or both, which can persist for up to 30 days in the acute phase. At the end of the healing process, altered (post-inflammatory) pigmentation may develop along the affected dermatome.
- The herpes zoster rash usually occurs on the chest or face. Involvement of the seventh cranial nerve can result in weakness in facial muscles and dermatological eruptions in the external auditory canal (zoster oticus). This combination of facial– muscle weakness and zoster oticus is known as Ramsay–Hunt syndrome. Involvement of the seventh cranial nerve can also cause ringing in the ears, hearing loss, nausea and vomiting, vertigo, and involuntary eye movements.














Your thoughts on this
Loading...