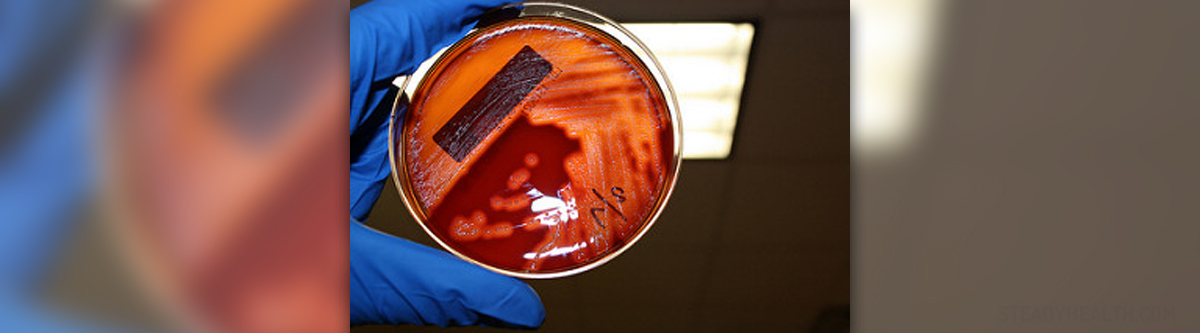
If you live in the United States and are seeing an obstetrician/gynecologist, or a Certified Nurse Midwife (CNM), you will definitely be offered the chance to be screened for GBS during your third trimester of pregnancy. The United States maternity care system takes a universal approach to GBS screening in pregnancy. Screening for Group B streptococcus is usually performed between 35 and 37 weeks of a pregnancy. A swab is taken from both the vagina and the rectum, and the results are ready within a day or two. If you test positive for Group B streptococcus, you will be given IV antibiotics during labor to prevent passing the infection onto your newborn. Some doctors advise treating a pregnant woman with Penicillin before birth and then testing again, but many say that this approach is not effective and any woman who tests positive for GBS during pregnancy should receive IV antibiotics while they are in labor. Most European countries do not offer routine Group B streptococcus screening and testing and take a a risk-based approach to GBS care instead. Women who test positive for Group B Strep are treated with vaginal Hibiclens (chlorhexidine) instead of, or in addition to, IV antibiotics.














Your thoughts on this
Loading...