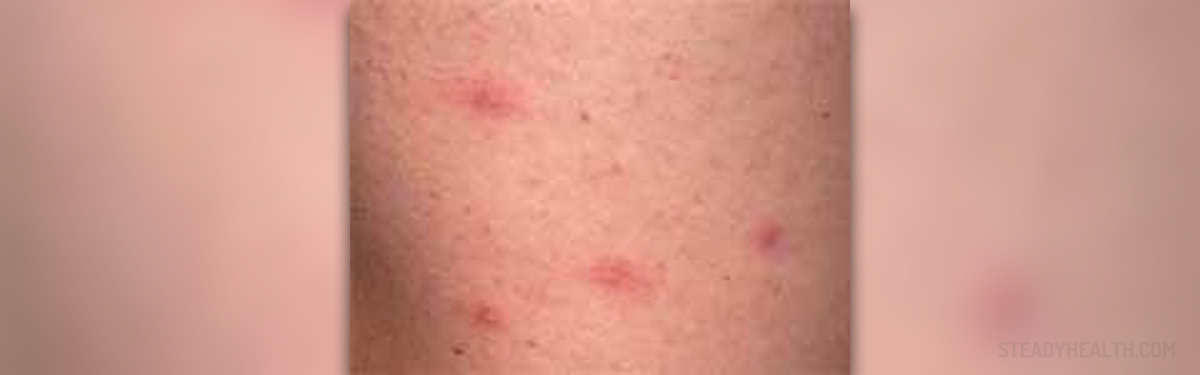
A fungal rash on the buttocks is medically known as tinear cruris, and more commonly referred to as jock itch. This is one of the most common fungal infections, which usually affects the region around the genitals, inner thighs, penis, scrotum, labia, vaginal opening and buttocks.
Several types of mold-like fungi called Dermatophytes, which normally live on the human body, cause a skin rash on the buttocks when their population overgrows and the person's microbial balance is disturbed. Fungi grow in dark and moist places, and the delicate skin folds around the buttocks, provide the perfect environment for their development. A fungal rash on the buttocks is associated with sweating, friction or abrasion and the direct rubbing of skin on skin.
Causes of fungal rash on buttocks
Fungi, responsible for skin rashes on the buttocks and nearby regions, normally live on the dead tissues of the skin, hair, and nails and thrive in warm, moist areas like the insides of the thighs. This area is usually sweaty and is not dried properly, so it provides the perfect place for fungi to grow. This condition is especially frequent among athletes, but anyone who sweats a lot can get jock itch. Males are at a slightly increased risk, as well as people with certain medical conditions, such as obesity, diabetes mellitus, or problems with the immune system.
Symptoms of fungal rash on buttocks
The symptoms begin as an itchy area in nearby skin folds, and the rash gradually develops, in some cases affecting the entire region. A fungal rash on the buttocks usually manifests in a circular pattern, causing a red and raised rash with elevated edges. The patient may complain about itching or burning sensations in the groin, thigh, or anal area. The skin will usually appear very red and inflamed. Flaking, peeling or cracking of the skin in the affected area is also very common. The rash may differ in appearance, from a dry and scaly rash, to a collection of small or red pink bumps at each hair follicle. In some cases, hair growth will stop in a region affected by jock itch.
Treatment of fungal rash on buttocks
Specific treatment for fungal rash on the buttocks depends upon the exact cause of the dermatitis. The rash usually responds to self-care. A lot of antifungal creams, corticosteroid creams, powders and sprays are available over-the-counter and most of them will be efficient in combination with both regular moisturizing (with creams such as shea butter) and allowing the area to breathe. Self-care is very important and the patient has to wash and dry the affected area carefully and change their clothes, and especially underwear, on a regular daily basis. When using over-the-counter medications, one should pay a special attention to use them as directed on the label. If the self-care does not help, or if symptoms last longer than two weeks, one should seek medical help.
If you are not sure whether your rash is fungal in origin or not, it is also best to seek medical help. Remember that contact dermatitis (resulting from chemical irritants), shingles, and even sexually transmitted causes such as genital herpes are also possible, along with causes like psoriasis. If antifungal creams do not resolve your symptoms, this provides a clear indication that you are likely to be dealing with something other than a fungal infection of the buttocks.















Your thoughts on this
Loading...