Introduction to Spina Bifida
The development of the human nervous system begins relatively early after the conception. The brain and the spinal cord develop from specialized plate of cells located at the back of the embryo. At some point the edges of this specific plate start to curl up toward each other and eventually form the neural plate. Being the precursor of the brain and the spinal cord the neural tube further undergoes specific changes. In case something interferes in this stage of the nervous system development, the affected baby will most likely end up with a neural tube defect.
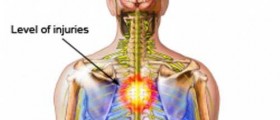
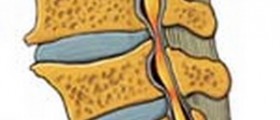
Spina bifida is one of these defects. The name of the condition means ‘cleft spine’ and this is quite correct since incomplete closure of the spinal canal allows some parts of the spine to protrude and get exposed to damage. Namely, the spinal cord is highly sensitive organ and this is the reason why it is located inside the spinal canal. The bones of the canal protect it from impacts of any kind. Now, when some portions of the spinal canal are missing, the spinal cord and its meninges may protrude, remain in the level of the skin or form a bulge in the middle of the back.
In the United States, according to statistics, each year between 1,500 and 2,000 out of 4 million babies are diagnosed with spina bifida.
Types of Spina Bifida
There are several types of this malformation, spina bifida occulta, closed neural tube defects, meningocele and myelomeningocele.
The mildest type is definitely spina bifida occulta. As a matter of fact this is the most frequently reported type of all neural tube defects. The very term ‘occulta’ refers to the presence of the malformation which cannot be seen with the naked eye. Namely, the spine protrudes through the gap in the spinal canal, is located under the skin but does not form any lumps so it is practically invisible. Nevertheless, such protrusion makes the spine quite vulnerable. Fortunately, in the majority of cases spina bifida occulta is asymptomatic and associated with no severe diability.
Closed neural tube defects represent a group of various spinal defects that affect the bone tissue, fat or the membranes covering the spine. Patients are either asymptomatic or develop severe disability such as paralysis and loss of control over their bladder and bowel.
Furthermore, in case one is suffering from meningocele there is only protrusion of the meninges through a gap in the spinal canal. The meninges may be covered with a layer of the skin or are completely exposed which puts an affected person under huge risk of infections, meningitis in particular. Again the severity of the condition ranges from mild to severe and quite debilitating forms.
And finally, there is myelomeningocele, the most complex of all the currently discussed malformations. The condition is characterized by protrusion of the spinal cord through a gap in the spinal canal and direct exposure of its tissues. Patients are partially or completely paralysed below the level of protrusion and there is also bowel and bladder dysfunction.
Prenatal Diagnosis and Treatment
Thanks to many diagnostic tools modern medicine offers today spina bifida can be easily diagnosed prenatally i.e. before the baby is born. Only mild cases when protrusion does not form a lump at the back and remains localized in the level of the skin may be overlooked.
Fetal ultrasound together with measurements of the maternal serum alpha fetoprotein (MSAFP) performed during the second trimester are great screening methods for neural tube defects including spina bifida. Under normal circumstances the fetus produces a specific protein called alpha-fetoprotein. It easily passes into the mother’s blood and can be measured when mother’s blood samples are taken. An increase in the level of this protein may, among several things, indicate the presence of neural tube defects. Fetal ultrasound gives perfect insight in the fetal structures and may detect abnormalities affecting the spinal cord and the nearby tissues.
Once the baby is born the condition can be confirmed after neurological examination (if there are neurological deficits) and with the assistance of X-ray, CT scan or MSI of the spine. These imaging techniques detect the gap in the spinal canal and protrusion of the spine.
Since there is no cure for spina bifida, the goal of the treatment is to prevent further damage to the spine and progression of current neurological deficits (if there are any). Treatment is individualized and adjusted to each patient mostly depending on the severity of the condition.
When parts of the spine are exposed, there is a risk of infections and these patients require hospitalization and rigorous measures against microorganisms. What is more, any exposed part of the spine must be protected against additional trauma. At some point neurosurgeons will perform surgery and close the gap in the spinal canal.
Today there is even more invasive surgery known as fetal surgery. The fetus is operated while still in the uterus. Even though this is a risky procedure, most doctors agree that the sooner the defect is corrected, the better are the chances that neurological deficits will not occur.
Later in life many patients require additional surgeries, especially if there are problems with their spine, feet and hips or they develop hydrocephalus. And finally, depending on the damage and neurological deficits patient may require various assistive devices.














Your thoughts on this
Loading...