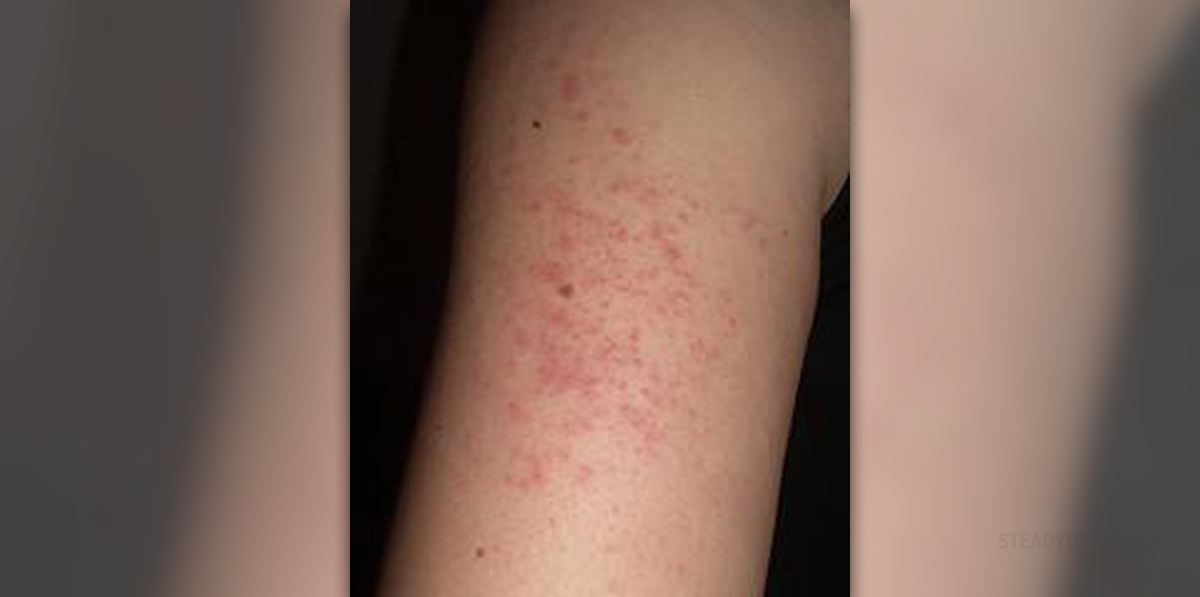
Keratosis pilaris is a skin condition affecting all age groups and both genders. This skin disorder is quite benign. The skin of the affected individual gets covered with many, small, rough and red (sometimes tan) bumps. These skin changes form around hair follicles and predominantly affect the upper arms, back, legs and buttock. In some people keratosis pilaris may develop on the cheeks.
The condition is widely known as 'chicken skin', 'goose bumps' or 'goose flesh'. Being completely harmless, keratosis pilaris is only considered an aesthetic problem.
Keratosis Pilaris Presentation
The condition is most commonly localized to specific body parts (the upper arms and the back). In rare occasions the entire skin gets covered with typical skin changes.
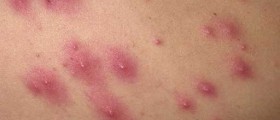
The rash in people suffering from keratosis pilaris comprises scattered, patchy groups of tiny little bumps (red or tan). One area may contain up to 100 bumps. The presence of such bumps gives the affected skin the texture of sand-paper. The skin around the bumps is inflamed and hence the red halo around the skin changes.Keratosis Pilaris Causes
The cause of keratosis pilaris remains unknown, but it seems that the condition has something to do with overproduction of keratin. It is estimated that approximately 50-70% of all patients carry genetic predisposition for the disease.
Keratosis pilaris occurs more in individuals with dry skin and whose with hypersensitivity reactions. It can be also connected with other skin conditions (e.g. ichthyosis vulgaris, eczema, atopic dermatitis etc.).Diagnosing Keratosis Pilaris
It is not hard to set the diagnosis of keratosis pilaris. This can be done by a well experienced doctor and the only thing he/ she needs to do is to perform a thorough physical examination and inspection of the skin. Typical organization and appearance of the skin changes makes setting of the diagnosis quite simple.Treatment and Prognosis
The condition is incurable. However, it may clear spontaneously without need for any medication. It is essential to mention that keratosis pilaris is not contagious and cannot be transmitted.
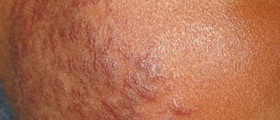
Potential complications of keratosis pilaris include postinflammatory hypopigmentation or hyperpigmentation. Permanent scarring rarely occurs and is only possible in individuals prone to deep picking and those who have undergone aggressive treatments.
People suffering from keratosis pilaris are due to prevent excessive skin dryness. They should, therefore, use only mild soap-less cleansers and lubricate the skin as much as possible. Proper lubrication is achieved with many over-the-counter lubricating moisturizer lotions. Lotions are supposed to be applied 2-3 times per day.
Some patients may be prescribed medium potency topical steroid creams. These are used for limited period of time (7-10 days). After the inflammation is brought under control, the rest of the bumps are removed with 2-3% salicylic acid in 20% urea cream.
One more treatment includes intermittent dosing of topical retinoids. Severe skin redness and inflammation may be reduced with topical immunomodulators. And finally, severe cases require oral intake of isotretinoin.













Your thoughts on this
Loading...