A liver transplantation, also known as a hepatic transplantation, is the replacement of a diseased liver with a healthy liver allograft. A liver transplantation is one of the most expensive medical treatments nowadays but it is generally well accepted treatment option for patients with end-stage liver disease and acute liver failure.Whole-liver cadaveric organs transplantation
The operation most commonly implies removal of the damaged liver and its replacement with a graft in the recipient’s natural anatomic position. For transplantation are often used whole-liver cadaveric organs collected from donors who have died from causes that have nothing to do with liver diseases. The main problem that occurs today is organ availability so many patients have to wait long time before being able to receive a transplant.
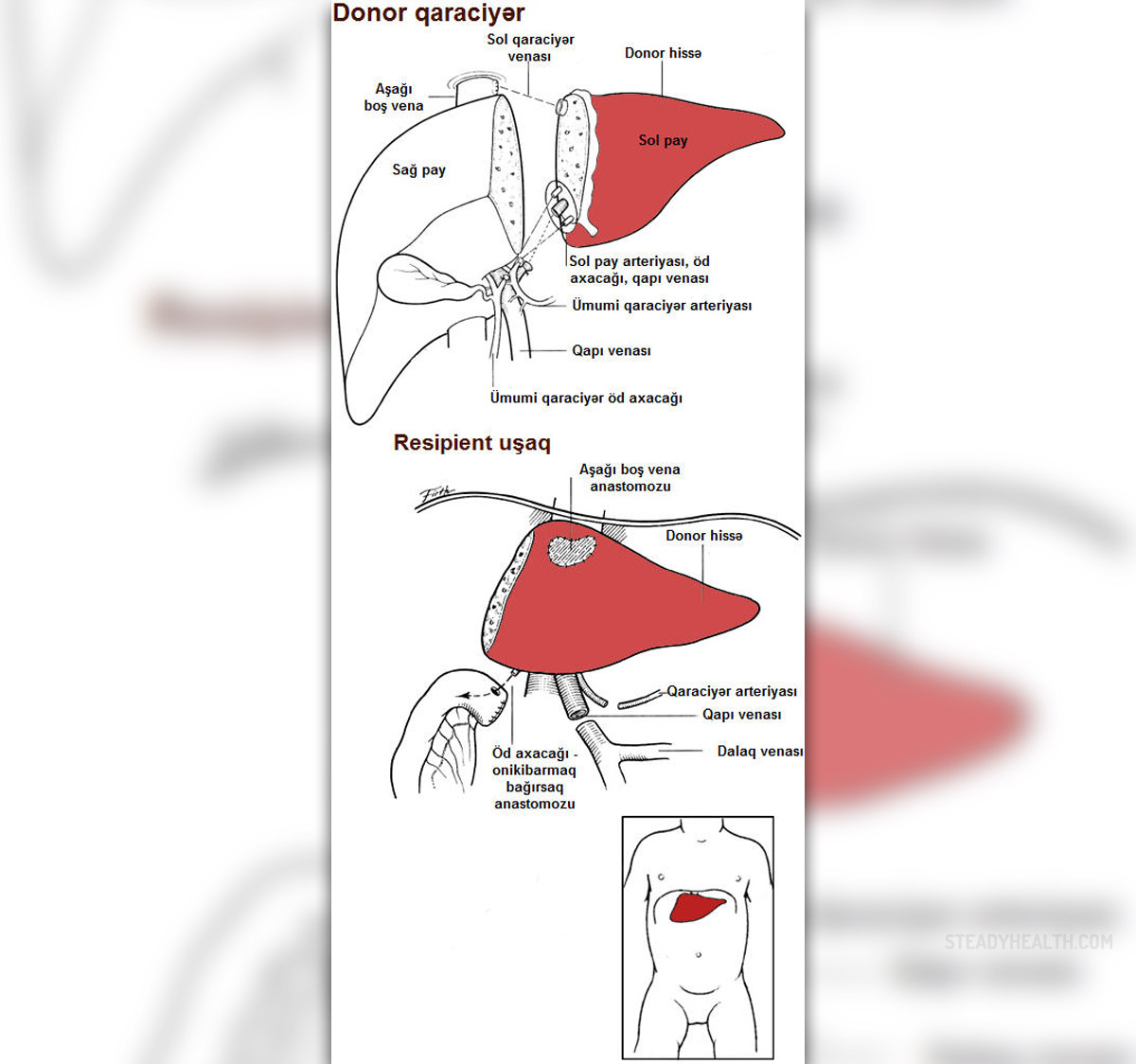
Living-donor liver transplantation
Because of the availability concern living-donor liver transplantation are becoming frequent. They imply taking a portion of the liver from an immunologically compatible donor, most commonly a relative, and replacing the entire diseased liver of the patient with the graft from donor’s liver. The donor is left with enough liver to preserve normal liver functions, and patient receives enough liver to restore normal functions. Both donor and recipient will benefit from proliferation of cells within a liver tissue that begins within 12 hours pass transplantation. This will result in the growth of the liver.
Living replacement method is necessary if patient’s medical results show deterioration of hepatic synthetic function, coagulophaty, portal hypertension, variceal bleeding, hypersplenism, ascites, or hepatic encephalopathy.Complications after the surgeryLiver transplantations are most commonly safe and well accepted treatments. However, some complications might follow as a result of a surgical treatment. Biliary and vascular complications together with rejection of the transplanted liver may be the main causes of losing the hepatic graft. The failure of the new liver occurs in 10% to 15% of all cases and in some cases it may even occur due to preexisting disease of the donated organ.
Medical therapy advanced in over last couple of years so that the diagnosis is nowadays more efficient and postoperative treatment increased the patients’ survival rate. However, biliary complications still remain a serious clinical complication that lead to increased morbidity, liver dysfunction, and graft loss. They might happen in 10-30% of patients who undertake liver transplantation. Advances in therapeutic ERCP have made it possible to avoid the risks associated with surgical intervention. ERCP with sphincterotomy reports morbidity rate of 9.8% and a mortality rate of 2.3% so it may be considered a therapeutic technique, rather than a diagnostic tool.














Your thoughts on this
Loading...