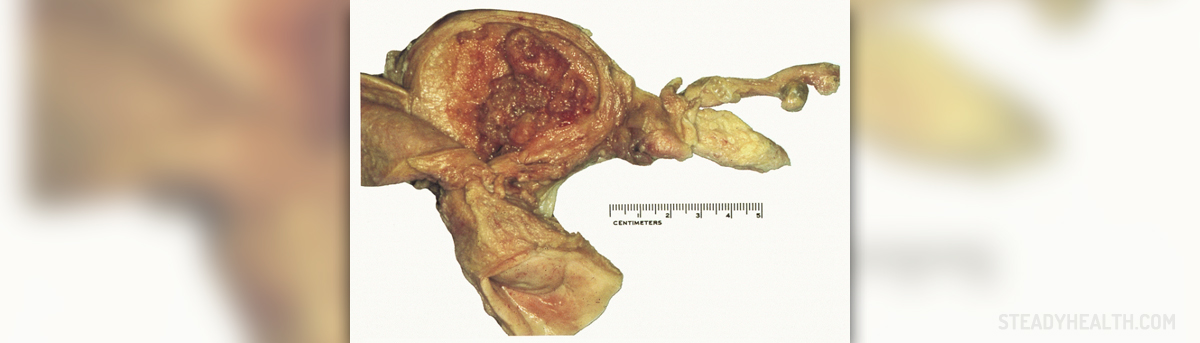
Generally, it is assumed that endometrial hyperplasia is caused by excessive levels of the female hormone estrogen, which is dominant in some parts of the menstrual cycle. When there is a lack of the hormone progesterone, that normally counters estrogen, endometrial hyperplasia can develop. Some ideal conditions for endometrial hyperplasia to develop are cases where a woman is taking medications for breast cancer, estrogen medications, and the menopause or PCOS. Abnormal vaginal bleeding is one of the major indications that a woman might have endometrial hyperplasia. This can come in many forms of course very heavy periods, prolonged periods, or bleeding in between periods are among them. It is diagnosed through an endometrial biopsy, or through ultrasound technology.
Treatment
In many cases, hormonal medications like the birth control pill, or progesterone (to counter estrogen) are able to effectively treat endometrial hyperplasia. In other cases, these medications do not work and the condition persists. For women who are not having any more biological children, a hysterectomy (the removal of the uterus) or endometrial ablation (the destruction of the lining of the uterus, which is possible using various non-surgical methods) are recommended sometimes. In around 10 to 20 percent of all cases of endometrial hyperplasia, the condition points to cancer. In these cases hysterectomy is the safest option. Still, it is important to remember that endometrial hyperplasia is not cancer in itself.










Your thoughts on this
Loading...