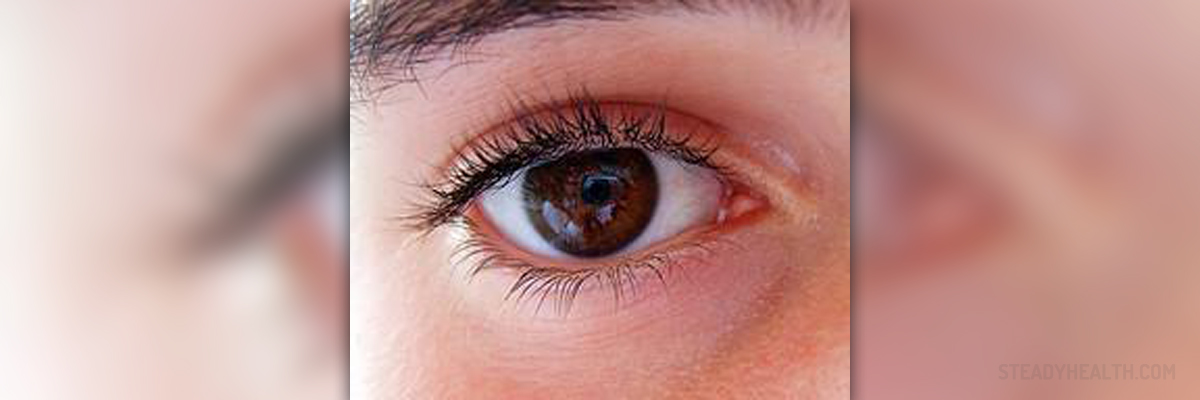
Diabetic retinopathy is a problem involving the retina of the eye, which becomes progressively damaged due to certain effects of diabetes. In the beginning, diabetic retinopathy does not cause any major vision problems, but as it progresses it can lead to complete loss of vision or blindness.
The treatment for this health issue depends on the stage in which it is. Background retinopathy does not require any specific treatment but annual check-ups at the ophthalmologist are required. Pre-proliferative retinopathy may or may not require treatment, depending on the amount of bleeding from the blood vessels into the retina. If the bleeding is excessive, laser treatment may be required. In maculopathy and proliferative retinopathy doctors usually recommend laser treatment, however, laser surgery will not be sufficient in advanced stages of proliferative retinopathy.
Laser surgery
As explained above, laser surgery is recommended in pre-proliferative diabetic retinopathy and in early or mild stages of proliferative retinopathy. It uses a technique called photocoagulation, in which the laser beam basically burns defective blood vessels in the eye. The procedure is usually done on an out-patient basis and it may require one or two or more sessions, depending on the severity of retinopathy.
The procedure is not painful but it may cause a mild prickling sensation. Eye drops are used to numb the eye and a special lens is placed to hold the eyelids open. Patients who undergo this procedure should expect to have blurred vision but only for a few hours after the procedure.
As for the complications and side effects of laser surgery for retinopathy, half the patients who have had it complain of difficulties with their night vision, while three percent of them experience some loss of peripheral vision.
Vitreous surgery
Vitreous surgery is the best treatment option for patients with advanced proliferative retinopathy. This procedure is required if there is a large amount of blood in the center of the eye, blurring the vision, or if excessive scarring causes detachment of the retina.
Because the blood gathers in the vitreous gel in front of the retina, the surgeon will make a small incision in it. Any scar tissue will be removed and the vitreous gel will be replaced with liquid or gas to hold the retina in place. Tiny clamps may be used to further strengthen the retina. As the gas or liquid dissipates or gets absorbed, new gel will be formed to replace the one removed in surgery.
Vitreous surgery is done using local anesthetic and sedatives, although in some clinics they use general anesthesia too. This surgery requires several days of recovery, during which time the patient will have to wear an eye patch. The vision will probably be blurred for several weeks before improving.













Your thoughts on this
Loading...