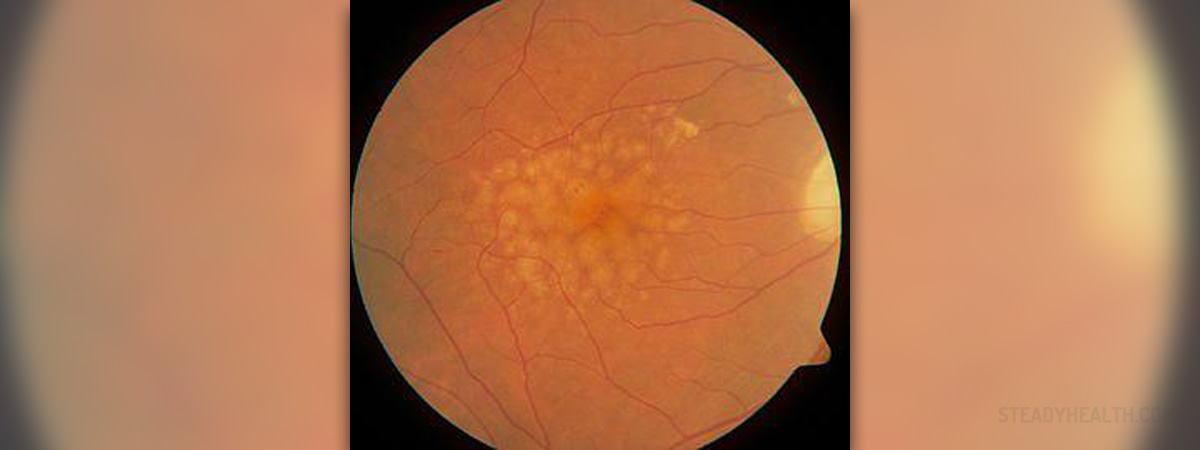
Diabetic Retinopathy
Diabetic retinopathy is an eye disorder which initially hides in the background and signals that there may be a damaging condition developing. Retinopathy exclusively affects the retina, which is a nerve layer at the back of the eye in charge of receiving light signals. Individuals who have had diabetes for years have some form of background diabetic retinopathy, but only about a fifth subsequently suffers from impaired vision. Retinopathy is characterized by vision loss and blindness, and it is potential complication of all diabetes types. It is a progressive disorder which results from weakened blood vessels in the eye. There are also a few types of the condition including hard exudates, hemorrhages, and microaneurisms. Hard exudates are characterized by lipid and protein leakage into the retina through busted blood vessels. In most cases the person’s vision is not affected unless the macula is involved as well. Hemorrhages are different in a sense that the blood from the busted vessels leaks directly into the retina. Such bleeding is similar to hard exudates because it does not lead to vision impairment unless the macula is included as well. Lastly, microaneurisms are manifested as red spots produces by small amounts of blood getting to the retina. The number of microaneurysms and hemorrhages is indicative of the progression of background diabetic retinopathy. Blood pressure needs to be lowered right away, and so does the level of sugar in the blood. If the blood sugar remains high, the condition will only be getting worse with time. It is possible for the weak blood vessels to burst in the eye and while the blood spills it can disturb the processes in the eye, affect vision, and cause a scar to form. If the blood accumulates around the macula, or the middle of the retina, it leads to swelling and vision problems. Another way in which diabetes leads to eye problems is by blocking the blood vessels that in turn deprive the retina of oxygen causing the formation of abnormal vessels. Background diabetic retina is fairly easily diagnosed during a routine check-up but it does not yield any symptoms. It is mostly treated as a sign that serious damage is coming. The presence of background diabetic retina is identifiable through a urine test as well and once detected there should be some form of treatment or preventative means introduced in order to stop any further damage. It is very important to keep the sugar levels in check. There are also a couple of signs pointing to the syndrome, such as difficulty adapting to the dark. One of the easiest ways to detect such a change is at a movie theatre, for instance. On the other hand, it is crucial for individuals with diabetes to have regular eye exams in order to catch the diabetic retina early. Once the vision starts to change as a result of the syndrome the condition has already spread too much. For those individuals whose doctors’ decided they are not at higher risk for developing diabetic retinopathy follow up exams every couple of years should be sufficient.
How is Diabetic Retinopathy Treated?
Presently, there is no cure for background diabetic retinopathy. However, there are treatment options which can aid in stopping further damage to the eye. For instance, certain types of laser treatments can prevent vision loss if the syndrome is detected early and there has not been too much damage. Laser treatments require no anesthetics, but eye drops are used to numb the eye during the procedure. The main aim of the laser treatment is to burn abnormal changes on the retina, and it should be pain free although mild form of discomfort is always felt. In most cases, laser eye surgery that is performed for any kind of treatment leaves the patients with no adverse effects. If retinopathy has not spread to the macula there is no need for therapy. Only regular check-ups are required. Sometimes a health care provider will suggest surgical removal of the vitreous gel or scars in cases of bleeding or detachment of the retina. Surgery as a means to treat retinopathy is only used if the laser was ineffective due to the fact that the disease is at a later stage. Most kinds of treatment options for retinopathy are successful in stopping the progression of the disorder, delaying vision loss as well as impairment. As there is no cure for either diabetes or retinopathy many individuals need to be treated more than once as both conditions get worse. The blood sugar and pressure have to be monitored and controlled even after eye treatments. In any case, careful monitoring of any changes in the body due to diabetes are the safest way to make sure the consequences of such an underlying condition are kept at a minimum.















Your thoughts on this
Loading...