
Diabetes and Eye Disease
One of the most common negative health effects of diabetes are vision problems. Vision problems range from mild to severe and often affect those who have had diabetes for at least 5 years. Among the different types of eye diseases is retinopathy, a condition characterized by the swelling of the blood vessels that is coupled with leaking of the blood into the eye. The primary cause of retinopathy is the high level of sugar in the blood followed by high blood pressure. Diabetic retinopathy can lead to complete vision loss and is the leading cause of blindness among adults in America. Regular checkups are mandatory for diabetic individuals for retinopathy does not reveal symptoms during the early stages. Even when persons notice changes in vision simply buying new glasses would not solve the problem. Clinicians agree that the best way to avoid the progression of retinopathy is to keep the levels of sugar under control. Aside from retinopathy, cataracts and glaucoma are also present in individuals suffering from diabetes.
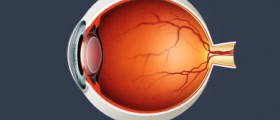
Diabetic RetinopathyDiabetic retinopathy is a condition that affects the retina and causes changes in vision. Retinopathy needs to be found before it produces any symptoms in order to stall its development. Annual checkups are often sufficient for those with long term diabetes. Retinopathy is produced by both Type I and Type II diabetes, but those affected by the former rarely experience eye problem before reaching puberty. Further, for the first five years Type I diabetics are likely to be free of vision problems. On the other hand, vision changes are more common with Type II diabetes. Once the underlying condition is diagnosed there is a strong possibility that vision changes will have already taken place. Other than keeping the blood sugar levels in check, high cholesterol and blood pressure also need to be controlled to stop the advancement of vision problems. Further, retinopathy can be divided into three distinct categories including the non-proliferative, the maculopathy, and the proliferative retinopathy. The non-proliferative retinopathy is characterized by a complete lack of symptoms despite the fact that there is already damage done to the blood vessels. Following the doctor’s advice and managing diabetes seriously is the only way to prevent further loss. Maculopathy is distinguished by the destruction of the macula, the central and most important part of the retina. When the blood leaks reach the macula serious vision loss is unavoidable. Lastly, during the proliferative stage new blood vessels are growing in the back of the eye but they are usually malfunctioning due to the complications caused by diabetes. Decreased levels of oxygen are also present, further thinning and disabling the vessels.
Cataract and Glaucoma with DiabetesCataracts are manifested through blurriness and clouding of the vision. The lens is affected by a cataract and although the condition is widespread among the general population in individuals suffering from diabetes it begins in early age. As is the case with retinopathy, high blood sugar speeds up the development of the problems. Similarly, the primary form of treatment is surgery to insert a lens implant while most individuals need glasses or contacts to see properly. In the case of glaucoma, eye pressure is too high as a result of liquid build up. In turn, the pressure destroys the blood vessels and nerves, leading to the subsequent loss of vision. The most prominent similarity between glaucoma and retinopathy is the fact that neither expresses signs or symptoms before the disease is so advanced that treatment has little effect. The symptoms of glaucoma include blurred vision, pain, headaches, excess watering of the eyes, and ultimately vision loss. The treatment ranges from eye drops and medications to laser surgery but prevention is the best medicine. Regular annual eye exams for diabetic individuals are crucial for keeping the vision strong and remaining problem free.
Driving with Diabetic RetinopathyIndividuals who are only affected by the non-proliferative retinopathy usually do not have any problems driving as they are not feeling any symptoms of the disease. If the person is prone to hypos careful treatment is required to treat them. In the case of frequent hypos the individual is obligated to stop driving. Further, laser surgery can interfere with night vision and produce a glare that wasn’t there before. Driving during the day is acceptable, but night time driving is best avoided whenever possible. Driving in the fog, rain, or reduced visibility conditions is not advised although the person is legally allowed to operate a motor vehicle. In addition, glare is a common occurrence among those affected by maculopathy and proliferative retinopathy. Glare is characterized by the inability to see through sun light or car headlights shining directly into the eyes. Glare is a symptom of cataracts as well, which can be surgically removed. Sunglasses are often able to solve the problem, but driving at night might not be safe.















Your thoughts on this
Loading...