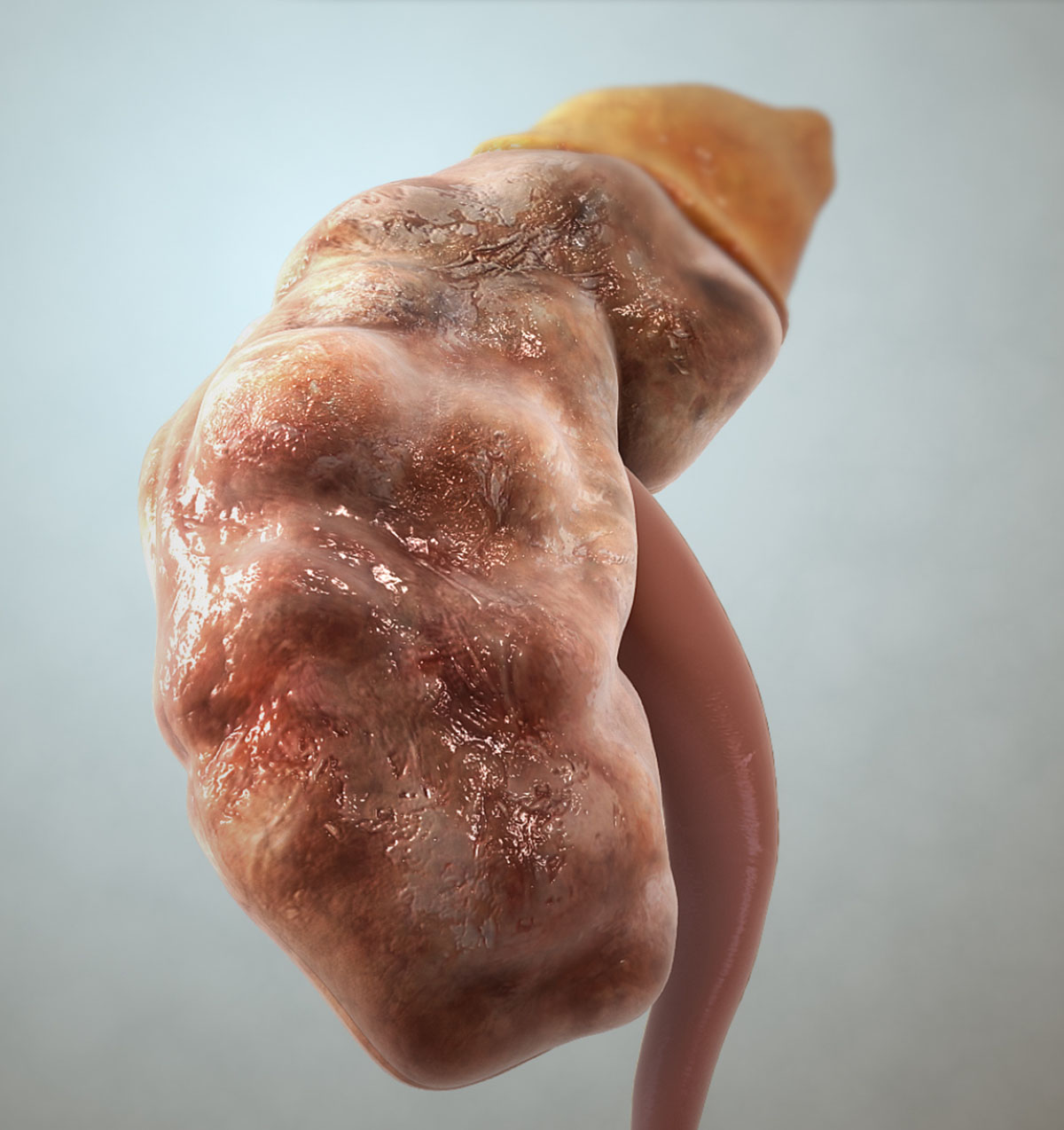
Definition of Chronic Kidney Disease
Chronic kidney disease is a certain type of medical condition which is characterized by a rather slow but progressive loss in renal function. It is also sometimes referred to as chronic renal disease. The symptoms of such medical condition are not always easily discernible since they may sometimes include only a reduced appetite while in some other cases the patient may feel generally unwell. This medical condition can be identified only by conducting a blood test for creatinine. Early stages of the disease may still indicate normal levels of creatinine, but they gradually get increased as the disease progresses. Kidney damage then needs to be investigated by conducting various other types of blood tests, imaging and sometimes even renal biopsy. The chronic kidney disease is characterized by five different stages. As of now there is no specific type of treatment which can be used for the slowing down of the progress of the disease.
Epidemiology
There are more than 16 percent of American citizens who are older than 20 and are affected by the chronic kidney disease. There are also approximately 2 million Canadian citizens affected by the chronic kidney disease. The number of people in the United Kingdom affected by the chronic kidney disease is more than 8 percent of its entire population.
Causes and Diagnosis
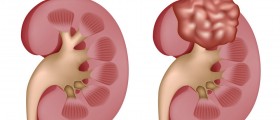
The most common causes of chronic kidney disease include glomerulonephritis, hypertension, diabetes mellitus, bilateral kidney stones, reflux nephropathy, toxin induced tubulointerstitial nephritis, polycystic kidney disease, lupus nephritis, diabetic nephropathy, focal segmental glomerulosclerosis, vasculitis, hemolytic uremic syndrome, bilateral renal artery stenosis and ischemic nephropathy. First off, chronic kidney disease needs to be differentiated from acute renal failure because it cannot be reversed. Abdominal ultrasound is usually one of the first steps in the proper diagnosis of chronic kidney disease. Kidneys affected by CKD commonly tend to be smaller than usual. As mentioned earlier, blood tests for creatinine are also excellent indicators, since chronic kidney disease always involves heightened levels of the serum creatinine. Some cases may involve further tests such as nuclear medicine MAG3 scans and DMSA scans.
Signs and Symptoms
In most cases, chronic kidney disease cannot be characterized by any symptoms in its initial stages. It is only when the amounts of serum creatinine get increased that the function of the kidney gets decreased. One of the most common symptoms is metabolic acidosis which occurs due to the accumulation of uric acid, phosphates and sulfates. It may also lead to several other medical complications. Another common sign of chronic kidney disease is a medical condition called hyperphosphatemia in which the excretion of phosphate gets significantly reduced. This medical condition usually progresses to other severe medical conditions such as vascular calcification, renal osteodystrophy and hyperparathyroidism. These three medical conditions are known for leading to extremely impaired cardiac function. Fluid volume overload is also common for those who suffer from chronic kidney disease and it is usually characterized by various forms of edema, some of which may even be life threatening. Some other common signs and symptoms of chronic kidney disease include significantly decreased synthesis of erythropoietin and accumulations of potassium and urea which ultimately lead to azotemia and uremia. It is a widely known fact that chronic kidney disease is also often associated with increased blood pressure and therefore it may often lead to severe medical conditions such as congestive heart failure and hypertension.
Stage 1 of chronic kidney disease is characterized by only mildly diminished function of the kidneys. This stage also includes kidney damage characterized only by certain abnormalities in imaging studies and urine or blood tests.
In stage 2 of chronic kidney disease, one can notice kidney damage as described in the stage one, but this time also accompanied by pathological abnormalities and mild reduction in GFR.
Stage 3 of chronic kidney disease is clearly defined by moderate reduction in GFR.
Stage 4 of chronic kidney disease involves severe reduction in GFR and according to the treatment plan it usually involves the preparation for renal replacement therapy.
Stage 5 of chronic kidney disease is commonly characterized by kidney failure and in some cases it may require permanent renal replacement therapy.
Prognosis and Management
The treatment method for all those who suffer from chronic kidney disease aims to stop or slow down the progression and prevent the aforementioned stage 5 from occurring. The types of medications commonly used for the treatment include angiotensin II receptor antagonists and angiotensin converting enzyme inhibitors. Most cases of chronic kidney disease may also require a replacement of two hormones commonly processed by the kidneys, known by the names of calcitrol and erythropoietin. Those who suffer from chronic kidney disease also suffer from elevated serum phosphate levels so they also need to be treated with phosphate binders. The stage 5 requires dialysis or a kidney transplant.











Your thoughts on this
Loading...