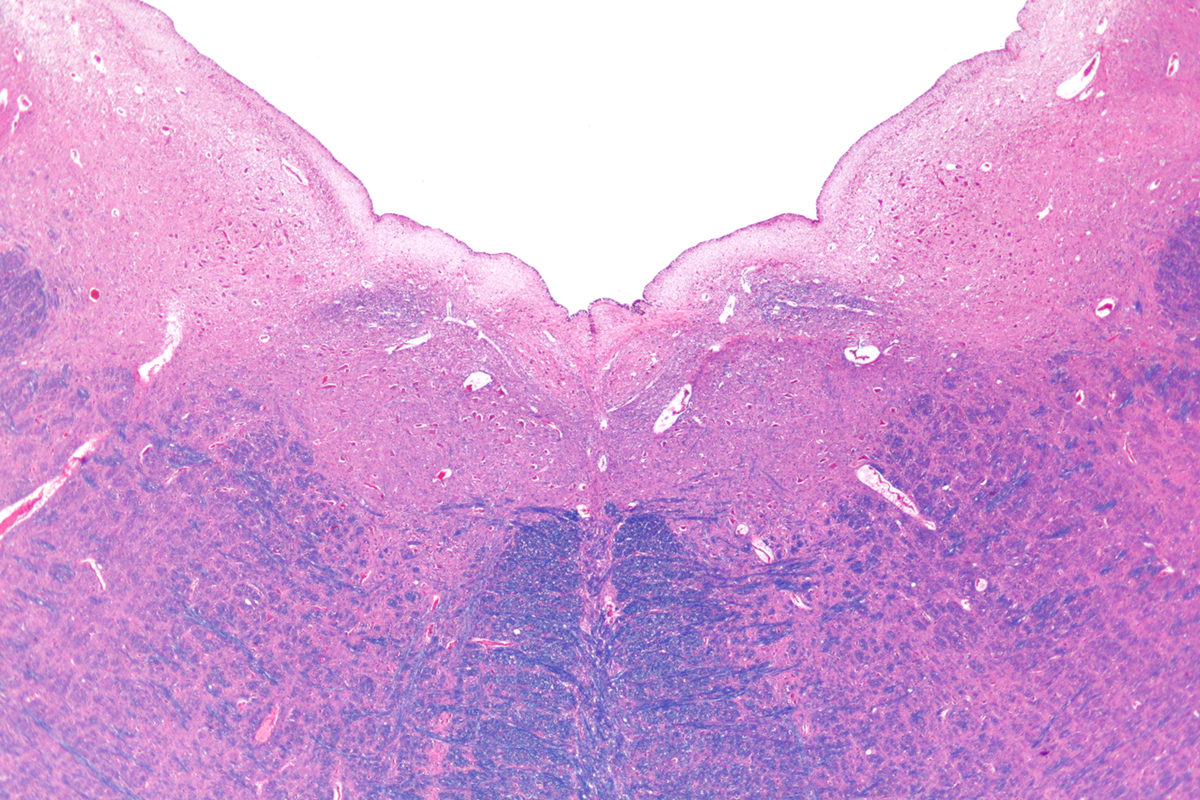
The vagus nerve is the 10th cranial nerve with many branches innervating various organs in the body. At the same time the vagus nerve collects and conveys sensory information to the brain informing the organ about the state of certain body's organs.
Vagus Nerve Stimulation Treatment
Vagus nerve stimulation (VNS) represents a treatment modality used together with the basic approaches in patients suffering from treatment-resistant epilepsy. This treatment approach is also beneficial for patients suffering from depression who do not respond well to prescribed medications.
When it comes to mechanism of action, scientists are yet to discover how stimulation of the vagus nerve modulates mood and seizures. It seems that the improvement occurs due to alteration of norepinephrine released by certain parts of the brain. The stimulation additionally increases the levels of inhibitory GABA and inhibits the abnormal activity of the reticular system.
As for the approval, in 1997 the FDA came to a decision that vagus nerve stimulation is a suitable adjunctive treatment option for partial-onset epilepsy while in 2005 the same agency approved the use of this treatment modality in patients suffering from treatment-resistant depression. However, there is still controversy regarding the treatment, especially when it comes to patients with depression. In spite of several studies that have confirmed the efficacy of vagus nerve stimulation in individuals with depression, the findings have not taken into account improvements over time in individuals without the device. There was only one controlled trial including patients who were implanted the device. In some of them the device was turned on while in others it wasn't. The results of the trial showed no greater improvement in patients in whom the device was turned on compared to the other group of tested individuals.
In spite of inconclusive opinion scientists currently investigate other potential uses of the treatment. They hope that one day vagus nerve stimulation might be capable of helping those suffering from anxiety disorders, Alzheimer's disease or migraines. It seems that even fibromyalgia and tinnitus may be one day brought under control with the assistance of vagus nerve stimulation.
As far as adverse effects of the treatment are concerned, these should never be overlooked. One of the most prominent side effects is intermittent decrease in respiratory flow during sleep. Namely, breathing disorders during sleep were confirmed in both pediatric and adult patients. The most frequently reported problems are an increase of apnea hypopnoea index and mild obstructive sleep apnea. Severe obstructive sleep apnea affects only small number of patients.
Furthermore, the treatment might bring along alteration of voice such as hoarseness, cough, pharyngitis and throat pain. Since the left vagus nerve does not participate in the innervation of the heart to same degree as the right one, it is better to implant the stimulator on the left side. By doing so the risk associated with potential arrythmogenic effects of vagus stimulation significantly reduces.
And finally, several more non-specific issues patients might experience include nausea, vomiting and indigestion. Paresthesia and dyspnea may occur as well but are relatively rare.
How is Procedure Done?
The vagus can be stimulated directly with the assistance of the cyberonics VNS devices or transcutaneously without any need for surgery.
Therapeutic vagus nerve stimulation is generally in the form of surgical implantation of the specific device. The stimulating device comprises a titanium-encased generator and a lithium battery along with a lead wire system made of electrodes. The leads to the vagus nerve are closely secured by an anchor tether. The battery serves the patients between one and 16 years.
The implantation procedure takes place on an outpatient basis. The surgeon makes an incision in the upper part of the chest and inserts the device right below the left collar bone. One more incision is made in the neck. It allows the access to the nerve. The goal is to wrap the leads of the device around the left branch of the nerve and finally connect electrodes to the generator. Once turned on the device will send electric impulses to the nerve cyclically.
As for transcutaneous vagus nerve stimulation (tVNS), it is achieved without surgical intervention. Namely, the goal is to stimulate the branches o the vagus nerve located under the skin. In the majority of cases the stimulation takes place on the concha of the ear.
One of the devices used in this purpose is cerbomed's NEMOS which is about to be released on the market. The efficacy of the device have been evaluated during several pilot studies. Drug-resistant epilepsy and Somatosensory pain have been the fields of interest. Patients from both groups, those suffering from epilepsy and individuals dealing with Somatosensory pain have responded well to t-VNS.
In conclusion, vagus nerve stimulation is supposed to be a treatment option once other available treatments fail to provide with desirable results. Doctors should never neglect the efficacy of traditional treatments and immediately opt for VNS without trying to bring the underlying condition under control with less invasive approaches. In spite of great efficacy, vagus nerve stimulation needs further evaluation and perhaps one day it will be suitable for additional medical conditions.














Your thoughts on this
Loading...