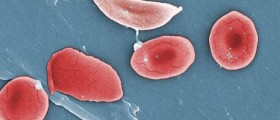
Fanconi anemia is a rare genetic disease that mostly affects people of the Ashkenazi Jews and Afrikaners in South Africa. This condition is actually an inherited blood disorder that leads to the problems in normal functioning of bone marrow. About 20 percent of affected individuals will develop cancer, usually the acute myelogenous leukemia, and about 90 percent of patients will develop marrow failure, before they are 40 years old. Marrow failure is a severe condition characterized by inability of the body to produce blood cells. This condition affects many body’s organs, systems and tissues, and it is often associated with many serious health problems.
Fanconi anemia genetics
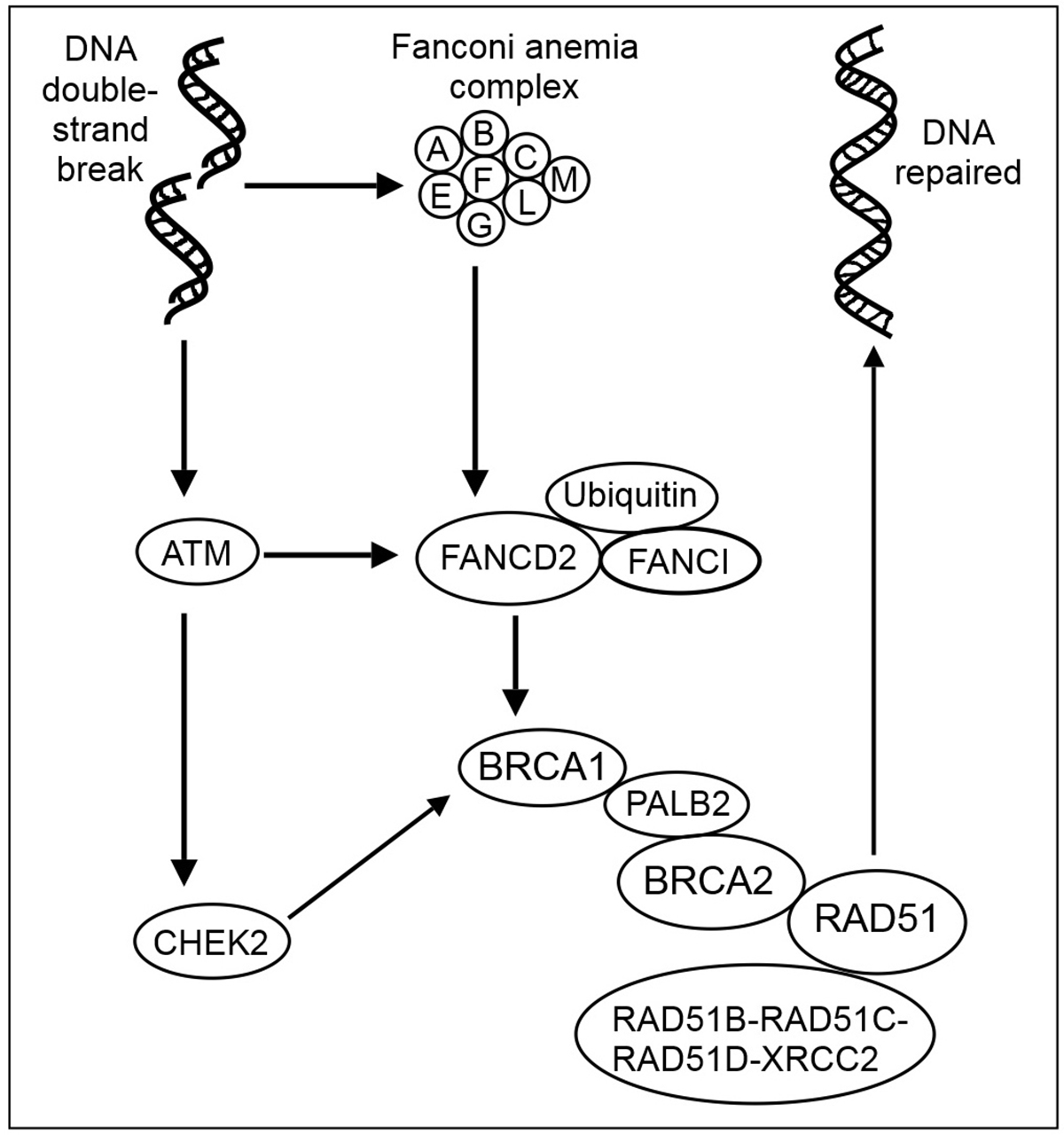
Fanconi anemia is an autosomal recessive genetic disorder, which means that two genes, one from each parent, are required to cause the disease in offspring. If the mother has a Fanconi anemia gene, there is a 50% chance that her son will also have it. This disease is associated with thirteen genes, but it occurs only in about one per 350,000 live births. It is estimated that about 1000 people from all over the world suffer from this condition at this point. One in 90 individuals in the Ashkenazi Jewish population carries the gene, and this is why it mostly affects people of this ethnic group. The only way to prevent the disease from occurring is to have a genetic testing as a part of family planning. The testing is highly recommended for the people of the Ashkenazi Jews.
Life expectancy
In many cases, Fanconi anemia results in severe complications. The average lifespan of affected individuals is usually somewhere around 30 years, and most of the individuals will eventually die prematurely as a result of complications related to bone marrow failure, leukemia, and solid tumors. People who are diagnosed with Fanconi anemia in childhood have greater risk of cancers later in life. People who survive to adulthood are most likely to develop cancerous solid tumors of mouth, tongue, throat, or the esophagus.
Treatment for Fanconi anemia
Fanconi anemia responds to a number of treatments, but the improvement is only temporary. The long-term treatment involves a bone marrow transplant if a donor is available. In most cases, patients are treated by androgens and hematopoietic growth factors. According to the statistics, only 50 to 75 percent of patients respond to this treatment. However, even the bone marrow transplantation carries certain risks such as the increased risk in organ toxicity and in graft-versus-host disease, and development of glucose intolerance.











Your thoughts on this
Loading...