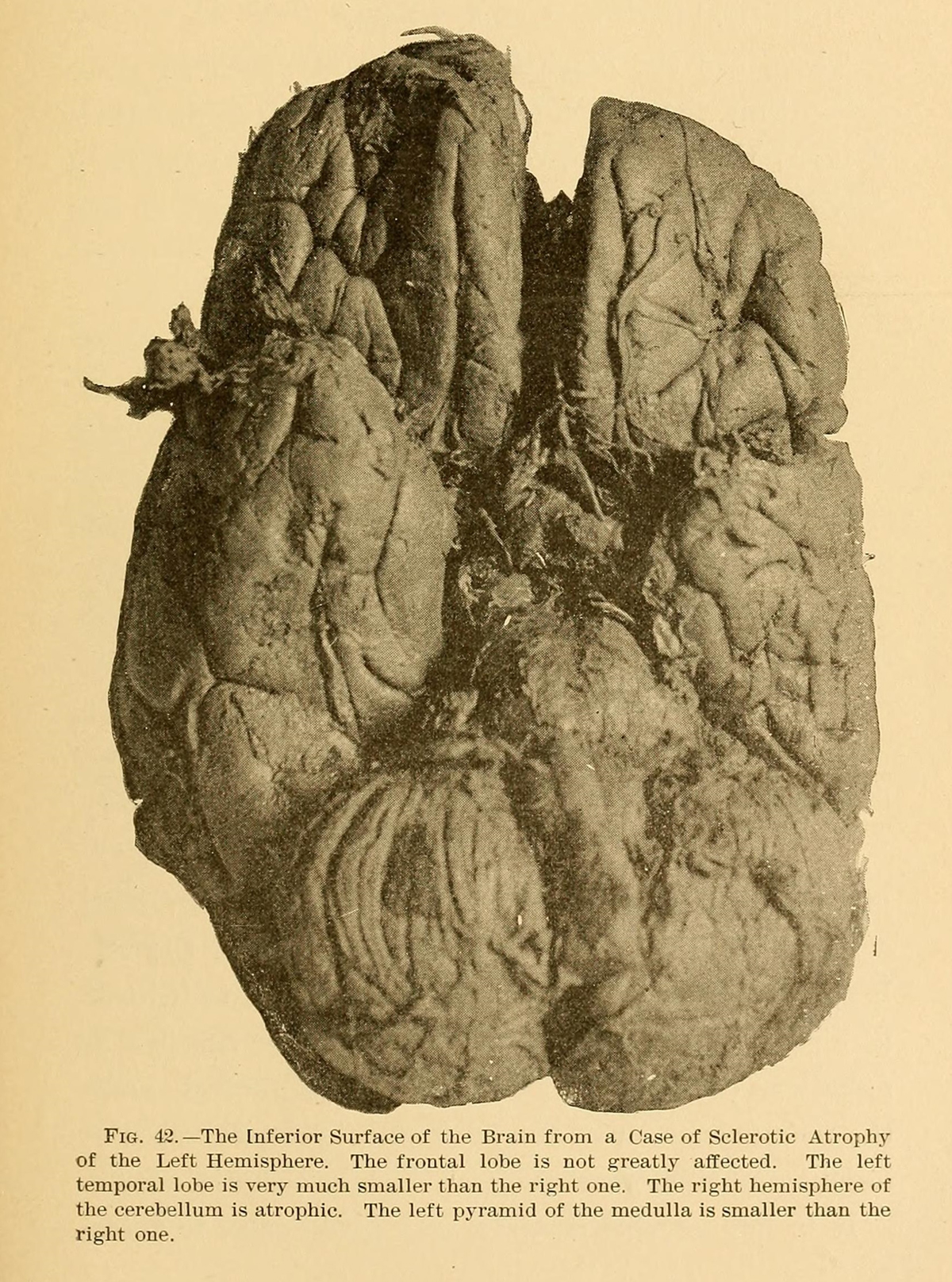
Epilepsy is one of the most widespread neurologic diseases that affects up to 4% of the world's population. An epileptic seizure is as sudden and transient signs or symptoms of abnormal, excessive or synchronous neuronal activity in the brain.
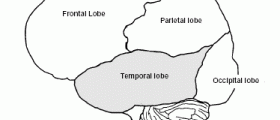
When antiepileptic drugs fail to manage the seizures, the patients may progress with surgical procedures, if their epilepsy can be treated that way. There are a couple of different kinds of epilepsy surgery. The best surgical choice may depend on the type of seizures one suffers from and where they originate in the brain.Temporal lobe resection
This kind of surgery is performed in the cases when doctors exactly know what part of the brain causes seizures. During this surgery, a small portion of the brain tissue will be removed. This method is effective for many patients. Great number of them stops having seizures after the surgery. Others might still experience some seizures, but they are a lot fewer than prior the surgery.
Multiple subpial transaction
Whenever surgeons think it is not possible to remove the part of the brain that causes seizures, they use multiple subpial transaction surgical method. It implies series of cuts that help separating the damaged part of the brain from the surrounding area. By this seizures stop spreading from one part of the brain to the others. Around 70% of patients that undergo this surgery feel much better afterwards and 50% to 70% of them stop having any seizures.
Corpus colostomy
This type of surgery is used to divide two hemispheres of the brain. It is most commonly used in children patients that may suffer from serious seizures that start from one side of the brain and spread to the other. Six to eight of ten patients will have fewer seizures after the surgery, from what they had before.
Hemispherectomy
This kind of surgery is very complex and it involves removing the outer layer of a hemisphere. It is most commonly used in children who suffer seizures, because of the brain damage in one hemisphere. Around 60% to 80% of patients treated with hemispherectomy will become free from seizures after the treatment.
Before the surgery
Patients being considered for the surgery will have to undergo a number of clinical tests called pre-surgical evaluation. These tests may include: EEG tests that measure the brain activity and locate the source of the seizures; CT scan that shows the physical structure of the brain and possible anomalies; Functional MRI scan that shows precisely which part of the brain handles critical tasks such as speech, motion, sensation and thinking; PET scan that will also give information about functions of the brain and point out to any abnormalities;And SPECT scan that shows different parts of the brain in different colors, showing how much of a blood flow each part of the brain receives. Higher blood flow usually indicates sources of seizures.During the surgery
Patients are often put in sleep with a general anesthetic so that a small opening in the scull can be made. In some rare cases, surgeon might wake up the patient during the surgery in order to precisely locate the part of the brain that controls language and motion.
After the surgery
Bone is replaced and fixed to the scull after the surgery, so it may start to heal. Patient’s head will usually be painful and swollen during the next couple of weeks. Patients will need to take painkillers, rest and relax over this period of time. They won’t be allowed to go to work or attend school for around three months. Anti-epileptic drugs will have to be used for a year or two after the surgery and then be significantly reduced or proscribed.
Risks
Risks generally depend on the type of the surgery. The most common risks include memory problems and difficulties to remember, understand or speak. Seizures may multiply after cutting the connections between the hemispheres, but they will be less severe. Patients may also have reduced or double vision after the surgery, and in some rare cases suffer from partial, one sided, paralysis.













Your thoughts on this
Loading...