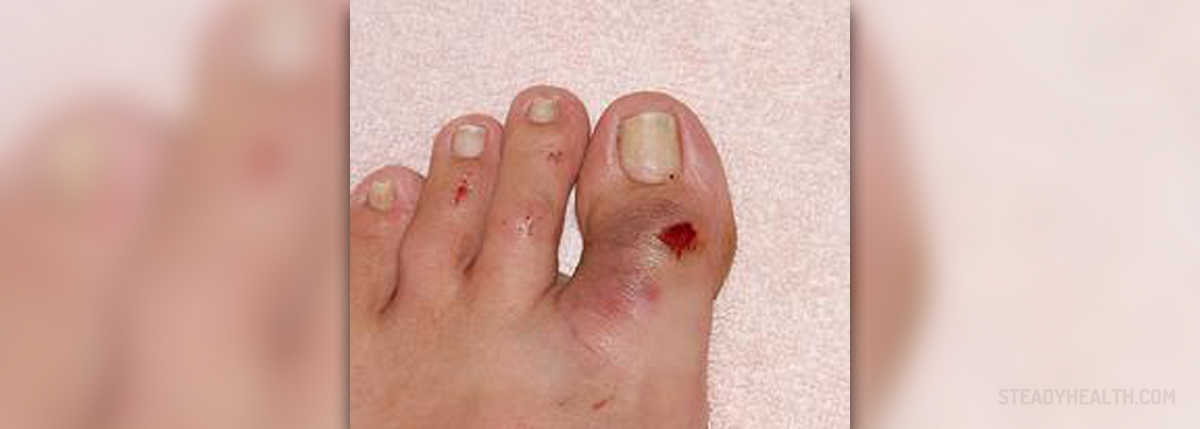
People suffering from diabetes face a variety of health problems affecting almost each and every organ in their body. This is why even the skin suffers due to inadequate level of glucose in the blood. The skin in such patients is quite delicate and susceptible to many changes. This particularly refers to the skin of diabetic patients' feet. Typical skin changes are associated directly to increased level of sugar in blood, or develop due to complications of the disease such as peripheral neuropathy and atherosclerosis.
Reasons behind Skin Changes in Diabetic Patients
Diabetic neuropathy is a complication of diabetes affecting nerves. Damaged nerves in the feet initiate severe changes to this part of the body. Feet become cold, they inadequately react to different sensations from the surroundings and may be easily damages. For instance, once the patients lose the inability to perceive hot stimuli, burns may occur easily if the affected feet is near the heat source. Also, such feet are more susceptible to infections because accidental and frequent cuts allow penetration of microorganisms.
Peripheral vascular disease reduces blood flow to the feet in these patients. Insufficient supply of oxygen and other nutrients is associated with progressive damage to the feet, postponing of wound healing and many more health issues.
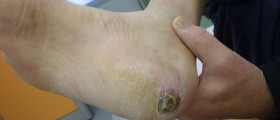
When a patient is suffering from both, diabetic neuropathy and peripheral vascular disease, the damage to the feet is even more complex and severe, leading to irreversible and non-healing ulcers which may even progress into gangrene. Such patients end up with an amputation of the affected part of the foot.
Diabetes and Types of Skin Changes on the Feet
The feet in diabetic patients may be dry. The reason for this is because the skin does not receive messages from the brain to produce sufficient amounts of sweat and oil which keep the skin moisturized. Many diabetic patients start suffering from dry skin once diabetic neuropathy takes place.
Dry skin is only a minor problem such patients commonly face with. There are much more complex changes affecting diabetic patients' feet. For instance, such individuals are prone to Athlete's foot, fungal infections of nails, calluses, corns, blisters, foot ulcers and ingrown toenails. Plantar warts also affect more people suffering from diabetes than healthy individuals.
Can Foot Problems in Diabetic Patients be Prevented?
Foot problems in such patients cannot be avoided because they will eventually develop. However, it is possible to postpone development of many changes affecting feet. This is achieved with treatment adjustments, maintaining optimal level of sugar in blood, regular exercise and adequate diet.
Even if diabetic neuropathy and peripheral vascular disease develop, patients are treated with certain drugs that may prevent rapid progression of changes affecting the feet. Finally, patients suffering from diabetes must check their feet regularly and report any change that occurs. This way the lesion can be timely treated.












Your thoughts on this
Loading...