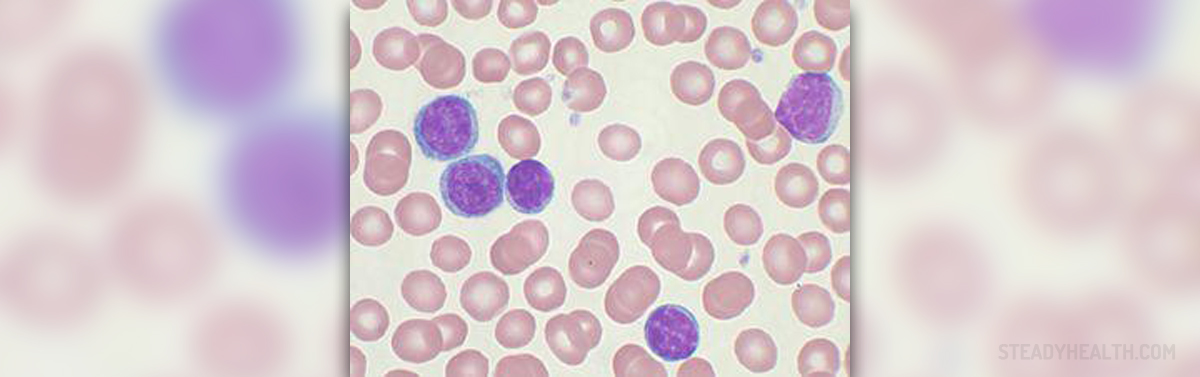
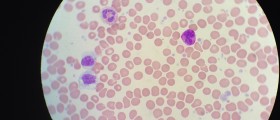
Haemolytic anaemia is a condition characterized by rapid and premature destruction of red blood cells. Red blood cells (erythrocytes) normally live up to 120 days. However, in haemolytic anaemia their life span is much shorter. The process of haemolysis develops either due to intravascular factors such as complement fixation, trauma or several more extrinsic factors or as a consequence of extravascular factors.
Why does Haemolytic Anaemia Occur?
Haemolytic anaemia may be congenital or acquired. Genetic causes of the condition include hereditary spherocytosis and elliptocytosis as well as haemoglobin abnormalities (sickle cell anaemia, thalassemia) and enzyme defects (glucose-6-phosphate dehydrogenase deficiency).
Acquired haemolytic anaemia may develop in a form of immune disease such as haemolytic disease of newborn or autoimmune disorders. A variety of autoimmune disorders are related to haemolytic anaemia. There are, for example, warm antibody type disorders such as systemic lupus erythematosus and Evan's syndrome. Furthermore, cold antibody type autoimmune diseases associated with haemolytic anaemia include cold haemagglutinin disease, paroxysmal cold haemoglobinuria etc. Drug-induced haemolytic anaemia may develop due to penicillin, cephalosporins etc. And finally, non-immune haemolytic anaemia results from trauma, different infections, hypersplenism, liver disease and may be associated with several more diseases.
Clinical Characteristics of Haemolytic Anaemia
Patients commonly develop symptoms of anaemia together with symptoms and signs of the underlying condition that has led to anaemia in the first place. Mild cases of anaemia may not be symptomatic while severe decrease in the number of red blood cells leads to tachycardia, dyspnoea, angina and weakness. Chronic haemolysis is associated with formation of gallstones. Intravascular haemolysis results in dark urine.
Treatment for Haemolytic Anaemia
Since active haemolytic anaemia may trigger folate deficiency, such patients may significantly benefit from folic acid. All medications that might have triggered haemolysis must be discontinued and replaced with suitable substitute drugs.
Blood transfusions are only indicated when utterly necessary. Iron therapy is generally recommended for patients suffering from persistent and severe intravascular haemolysis which induces chronic and substantial iron loss.
Patients in whom this type of anaemia is caused by certain autoimmune illnesses may benefit from corticosteroids. These drugs suppress excessive response of the immune system and prevent further uncontrollable damage of red blood cells.
Some patients may require splenectomy. This procedure is recommended for patients with enlarged spleen (hereditary spherocytosis) and is not found suitable for people with cold agglutinin haemolytic anaemia.
With proper treatment many complications of haemolytic anaemia such as high output cardiac failure, jaundice, iron deficiency etc. can be successfully prevented.











Your thoughts on this
Loading...