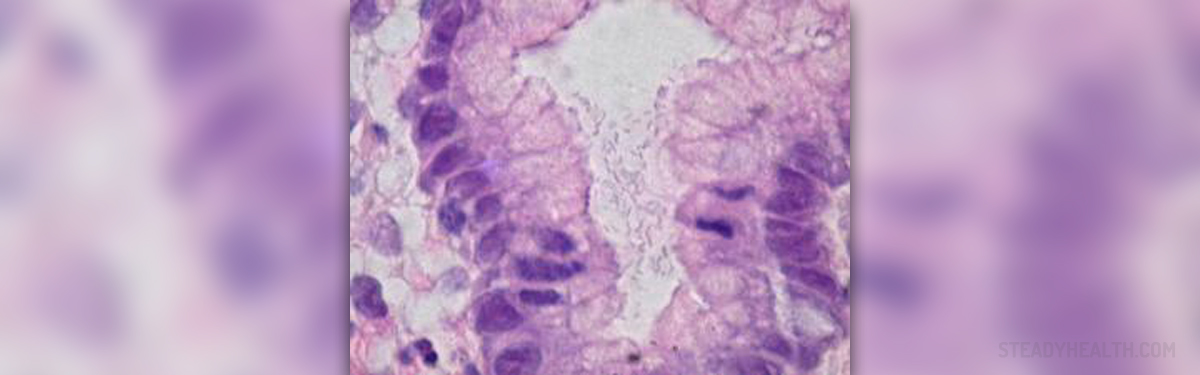
Chronic Gastritis
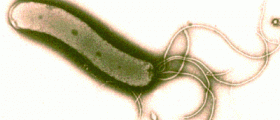
Chronic gastritis is an inflammatory disease of gastric mucosa. Causes are numerous, and the pathogenesis is unclear. The most common cause is Helicobacter pylori.
Chronic gastritis may be a direct continuation of acute gastritis, but, also, it can be caused by other factors such as long-term use of very spicy, hot or cold foods, strong drinks, coffee, smoking and swallowing focal purulent discharge from the upper respiratory tract. Besides that, chronic gastritis may be caused by a nutritional allergens and longer use of certain drugs.
Today, there are more and more evidences that genetic factors and immune processes are involved in the occurrence of chronic gastritis.Inflammatory process may be diffuse, localized to certain parts of the stomach or limited to a small zone - zonal gastritis. In order to simplify access to chronic gastritis this disease is now divided into: Erosive - hemorrhagic gastritis Non-erosive specific chronic gastritis Non-erosive nonspecific chronic gastritis
Erosive - Hemorrhagic Gastritis
This type of type of gastritis may be asymptomatic, but also may be accompanied with dyspnea or bleeding from the upper gastrointestinal tract. Bleeding occurs in less than 6% of patients.Causes of haemorrhage usually include: alcohol, non-steroidal antirheumatics and physiological stress that has arisen due to a severe acute illness or surgery.
Non-erosive Nonspecific Gastritis
Combination of biopsy and endoscopic findings is used in its diagnosing, because, it hardly can be diagnosed by only endoscopic methods.Symptoms of Chronic Gastritis
Symptoms of chronic gastritis are minor and uncharacteristic even in more serious forms. Patients usually complain about dull and diffuse epigastric pain which worsens after eating, especially after abundant meal, because of spreading the inflamed gastric wall.Beside pain, there is disgust, bloating and fullness, particularly after meal. Appetite is variable: sometimes there is a feeling of hunger and patient eats all foods, while change in appetite means attraction to, for example, spicy or salty foods.
There is heartburn and belching, irregular bowel emptying - diarrhea or constipation. Patient’s face is burning red after the meal. Also, bleeding can occur.
Diagnosis
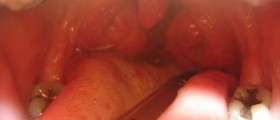
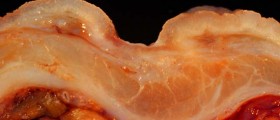
Diagnosis is primarily made by Helicobacter pylori isolation. Endoscopic examination and stomach mucosa biopsy are the most secure methods, by which doctor looks preservation of the lamina, the penetration of lymphocytes from superficial to deeper layers and the intensity of the gland formations reduction.Treatment
Moderate physical activity, well-boiled meat, soft boiled eggs, fresh cheese and mashed vegetables and fruits are recommended with bearing in mind the individual food tolerance.The most important thing is how the patient eats, not what he/she eats. In addition to diversity, meals should be small and often. The spices, coffee, tea and alcohol should be removed from the diet. Besides all this, therapy against Helicobacter pylori should be included. Treatment is long and persistent.
Occasional gastroscopy is required.









Your thoughts on this
Loading...