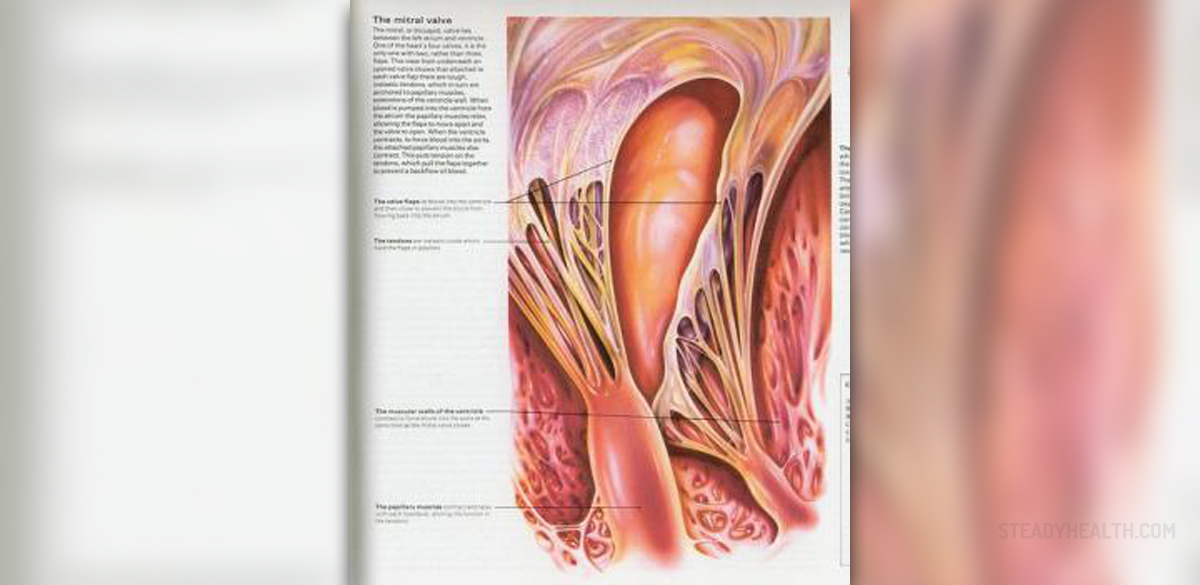
Mitral Regurgitation
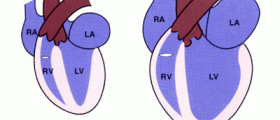
Mitral regurgitation is a state in which the blood from the left ventricle re-enters the left atrium instead of being pushed into the aorta. The mitral valve is a structure which separates left ventricle from the left atrium. Normally it closes during the contraction of the left ventricle. However, in regurgitation the mitral valve cannot close completely and some of the blood re-enters the left atrium. This condition can be compensated in the beginning of the disease but if left untreated it may progress and become decompensated.
Mitral regurgitation develops gradually and has 3 stages. In acute stage of the disease chrodae tendinae or papillary muscle rupture due to certain medical conditions such as myocardial infarction. This results in volume overload of both, the left atrium and ventricle. The filling pressure of the left ventricle rises and this, together with increased amount of blood in the left atrium, leads to elevated blood pressure inside the left atrium. The pressure can further transfer onto the lungs and cause pulmonary edema.
If the patient manages to tolerate the acute phase he/she enters the second phase of mitral regurgitation called chronic compensated phase. This phase features with hypertrophy of the left ventricle. In this stage the disease progresses and finally leads to dysfunction of ventricle muscle. The dysfunction interferes in normal emptying of the ventricle during systole, the blood still regurgitates into the left atrium and this all can be kept under control for certain period of time. In final stage, chronic decomplensation leads to pulmonary congestion.
Causes of Mitral Regurgitation
In people who are under 40 the most common cause of mitral regurgitation is rheumatic heart disease.
The prolapse of the mitral valve is another cause. It occurs as a consequence of mixomatous degeneration of the mitral valve. The process is rather slow and the most serious complication includes rupture of the chordae tendinae.
Furthermore, mitral regurgitation may develop as a consequence of coronary artery disease and resulting ischemia.
In some people regurgitation is caused by mitral annular calcifications which do not allow the valve to properly contract and close.
If the left ventricle dilates this also leads to annular dilatation and the valve, even though it is not damaged, cannot close adequately.
Another cause is rupture of tendinase due to certain heart conditions such as endocarditis, heart attack or trauma. Even papillary muscle dysfunction can consequently result in mitral regurgitation.
Apart from the previously mentioned additional cause of mitral regurgitation include Marfan syndrome, systemic lupus erythematosus, osteogenesis imperfecta, Ehlers-Danos syndrome and many more.














Your thoughts on this
Loading...