
About bedwetting
Bedwetting, medically known as enuresis, is a problem with controlling the bladder. The person suffering from bedwetting has difficulties controlling urination while awake or sleeping. Nocturnal bed wetting most commonly affects children. They normally achieve bladder control at different ages and first learn how to achieve daytime continence while they may still have difficulty achieving nighttime continence. The condition is not considered serious in case the child has not reached preschool age.
Nocturnal enuresis is classified as primary or secondary. Primary nocturnal enuresis is defined as inability to stay constantly dry at night while secondary enuresis develops if the child has experienced at least 6 months of dryness at night and then shows inability to control urination at night.
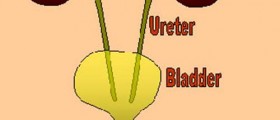
There are many psychological issues and medical conditions associated with nocturnal bedwetting. Primary nocturnal enuresis is, for example, connected with chromosomal abnormalities. Furthermore, the condition may develop as a consequence of abnormally positioned ureter, constipation, excessive urine output, certain heart conditions, neurological disorders, sleep arousal disorder, urinary track infection and urethral obstruction. Secondary bedwetting is strongly associated with many psychological issues, stress or can be a side effect of certain medical conditions such as diabetes, excessive production of the thyroid gland hormones, epilepsy or obstructive sleep apnea.
Therapy for Bedwetting
It is essential to find the underlying cause and pay attention to social as well as psychological impact of the condition. Treatment for bedwetting includes behavioral modification, medications and in certain cases surgery.
Behavioral modification is essential for managing nocturnal enuresis. Parents are advised to be patient and support their child. This therapy may show positive results within a month. Positive reinforcement is one technique that includes periodical waking the child at night to use the bathroom. Restricting the intake of fluids late in the day and encouraging regular habit to urinate are also beneficial. Alarm devices represent an excellent way to treat bedwetting but they are generally recommended in children over the age of 7. The device works by a sensor that detects the urine. Once the alarm is activated the signal is sent and its purpose is to wake the child. The alarms may produce sound, light or they vibrate. This helps the child to stop urinating in the bed and to continue urination in the bathroom.
Bladder training is a good option for children whose bladder cannot hold sufficient amount of urine. The goal of this treatment is to gradually increase the amount of urine the child can hold which is adapted to the child's age. This method is recommended prior to using medications and starting with the alarm device.
Medicamentous treatment is reserved for children in whom the condition cannot be brought under control with nonpharmacological treatments. There is a variety of medications and the doctor will chose the most suitable one.













Your thoughts on this
Loading...