When air is prevented from entering the sinus opening, it will usually result in a blocked sinus. There are four different pairs of cavities in the sinus, and they all help with the process of warming and filtering the air that comes in and out. Each pair of cavities has an opening named ostium which is attached to the passage of the nasal cavity. When the mucus is thicker than usual, it can block the ostium and then in turn irritate the lining. The lining of the mucus passageway has small hairs called cilia, the cilia have the job of taking the built-up mucus out of the nose. However, if these hairs get irritated it can affect their job, and this can start a buildup of the mucus and block the sinuses.
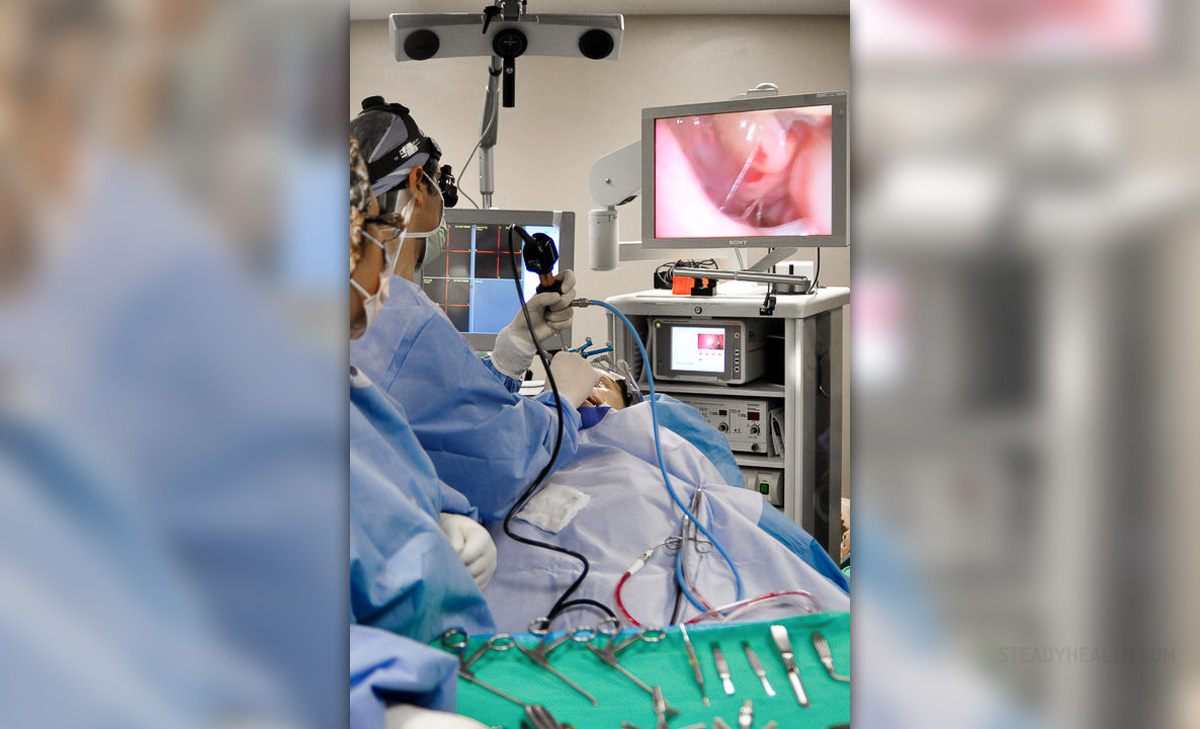
The Risks of Blocked Sinus
Having a blocked sinus can impact a person’s life by causing them to experience pressure and headaches. They cannot indulge in certain activities, such as scuba diving. It also causes the host to generally feel uncomfortable. To prevent other complications, it is imperative to release the blockage.
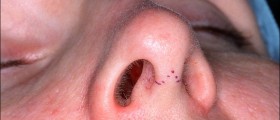
Endoscopic Sinus Surgical Procedure
It is more often than not performed as an outpatient procedure. The surgeon will attempt to clear the blockage by removing the inflamed tissue, and possibly the bone, as well as the infection. The procedure takes around three hours to complete, sometimes meaning an overnight stay. Once the procedure is complete, they will pack temporary sponges in the nose.
However, it will not be completely packed to permit natural nasal breathing. The surgeon may decide to remove any polyps present at the same time as the procedure for the blocked sinus. There is very little pain following the procedure, some may feel slightly tired. If a patient has suffered with quite a lot of swelling, this may take a few months to completely dissipate. The patient may notice some dry blood and some crusting inside of the nose, which may benefit from washing with salt water now and then.
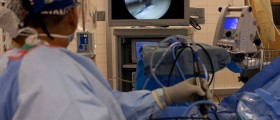
- Since functional endoscopic sinus surgery was introduced, the indications for performing this procedure have been expanding. The advances in the endoscopes, the camera, instrumentation, and navigation have laid the groundwork for an ever-expanding world of endoscopic surgery to access the skull base, optic nerve, cavernous sinus, pituitary, orbit, pterygopalatine fossa, and many other spaces and structures.
- Sinus disease is also a significant financial burden on the health care system. For instance, there is, on average, a yearly expenditure of $8.3 billion for chronic rhinosinusitis in the United States.
- In addition to cost, CRS has a major negative implication on the quality of life of patients emotionally and physically. Diagnosis of CRS should be based on symptoms and objective findings on physical examination using anterior rhinoscopy, or nasal endoscopy, or on computed tomography scans. Based on the clinical practice guidelines, CRS is initially treated with saline irrigation and/or topical intranasal steroids. When maximal medical therapy fails, the next step is endoscopic sinus surgery.
- Contraindications for FESS include patients who have general contraindications for general or local anesthesia. Also, contraindications for purely endoscopic surgery include lesions/ pathologies extending into the palate, skin/soft tissues, laterally into or above the orbit, lateral recesses of the frontal sinus, or advanced intracranial involvement. In cases with significant extensions, a combined endoscopic and open approach may be required instead.
- A thorough nasal endoscopy is performed using a 0 or 30-degree scope. Then, the lateral nasal wall near the uncinate and the axilla of the middle turbinate are infiltrated with 1% lidocaine with 1:100,000 epinephrine using a 3 ml syringe and 27 gauge needle. Following that, oxymetazoline-soaked cotton pledgetts are placed in the middle meatus (though some surgeons prefer 4% cocaine solution).
Possible Complications Following an Endoscopic Sinus Surgery
After any surgery, there is always a risk of inflammation and/or infection. If you notice a discharge following the surgery or a feeling of pressure, then it is advisable to see your doctor. For a few days following the procedure some people may experience nose bleeds, but if this continues for more than a day or two, see your doctor.
- www.nhs.uk/conditions/sinusitis-sinus-infection/
- www.nhs.uk/conditions/nasal-and-sinus-cancer/
- Photo courtesy of BestInPlastics by Wikimedia Commons: commons.wikimedia.org/wiki/File:Endoscopic_Sinus_Surgery.jpg












Your thoughts on this
Loading...