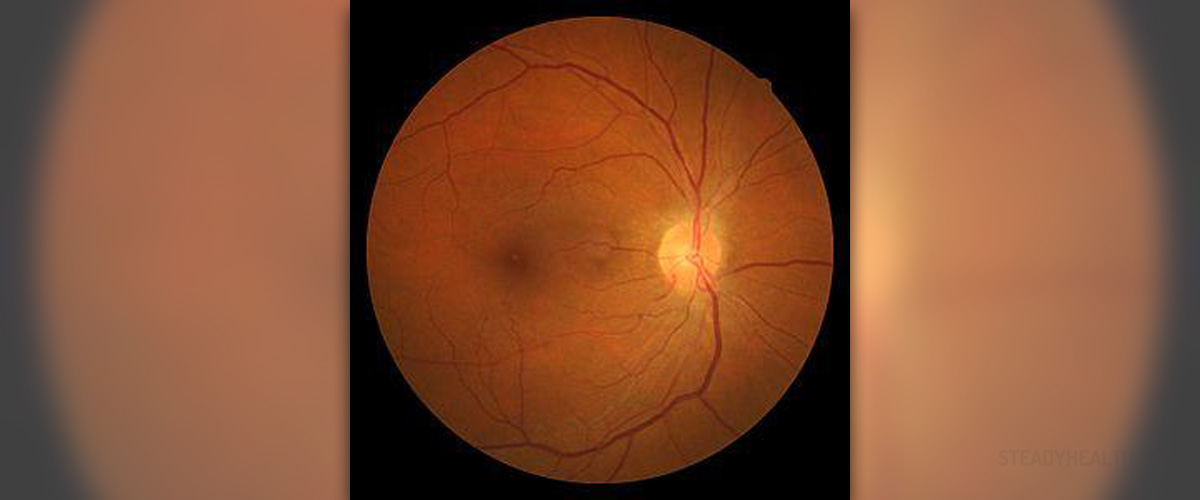
Human retina consists of two overlying layers, outer and inner. Outer layer is made of one layer of epithelial cells and located near the richly vascular choroid, while the inner retina consists of several layers of neural cells and some supportive tissue.
Blood Supply to Retina
Retina gets the blood from one of two possible sources. Epithelial cells, photoreceptors and some other tissue are supplied by the choroid. The choroid, on the other hand gets the blood from ciliary arteries coming down from the ophthalmic artery and internal carotid artery. Epithelial cells and photoreceptors are divided by certain barrier, designed to protect the neural retina (inner layer of retina) from some large toxic molecules. Central retinal artery and vein (coming from the ophthalmic artery and veins) supply the blood to the inner neural retina.
This part of the body could be affected by the problems in blood vessels, but which part of the retina will be involved depend on the problems and its location.
Systemic Diseases Affecting Retina
Different medical conditions may affect functioning of retina, including some systemic problems. Retinopathy could result as the consequence of high blood pressure (hypertension), or be associated with atherosclerotic stenosis of the carotid, sickle-cell C disease or thalassemia or in some cases with severe traumas or injuries.
Hypertensive retinopathy is commonly found in patients with chronic hypertension. This condition is characterized by narrowing of the arteries (known as copper wiring), vascular leakage and arteriosclerosis. These symptoms are specific and easily identified on fundoscopy. Acute hypertensive crisis in young adults may also be presented as choroidal changes or occlusions of the retinal vein.
Chronic hypertension usually doesn’t affect the vision or causes slight problems. Malignant hypertension is known to provoke headaches and decreased vision and this condition is a medical emergency and should be treated as such. Vision problems due to hypertension can usually be resolved controlling the blood pressure.
Ocular ischaemic syndrome is uncommon problem, caused by severe ipsilateral atherosclerotic carotid stenosis and consequent ocular hypoperfusion. Patients are usually older people (50 to 80 years of age), suffering from hypertension, diabetes, cerebrovascular disease or ischaemic heart disease. Men are twice more likely to develop this problem than women. The vision decreases gradually, over weeks and months, there is some redness of the eyes, corneal edema, periorbital pain and prolonged recovery after exposure to bright light. Treatment consists of topical steroids, mydriatic medications and some laser treatment, but the outcome is generally poor.
Sickle cell retinopathy is very severe. It is associated with sickle-cell C disease or sickle-cell thalassemia, causing arterial occlusion, peripheral arteriovenous anastomoses and growth of some new vessels. Patients usually don’t experience any problems until late stages (stage 4 or 5), when some trivial trauma to the eye may end up causing some bleeding, fibrovascular proliferation or retinal detachment. Laser treatment and surgery may control neovascularization in some cases, which basically determines the successful outcome.
Purtscher’s retinopathy occurs in patients suffering from some serious head traumas, chest compression or other crush injuries. Other causes may include: pancreas problems, lymphomas, diseases of the connective tissue and diseases leading to bone marrow transplant, as well as pregnancy and childbirth. Patients experience sudden and complete loss of vision, due to white retinal patches and bleeding around the disc. There is not available treatment and the visual recovery depend on the damage of the macular or optic nerve.














Your thoughts on this
Loading...