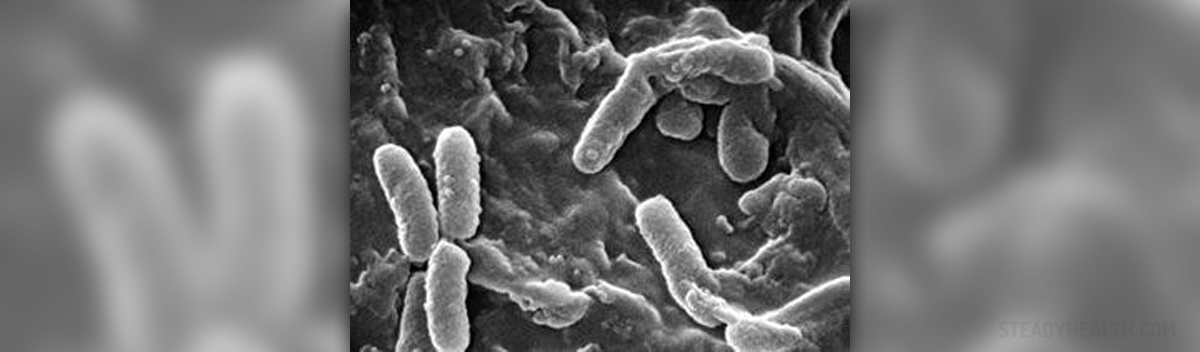
Definition
Pseudomonas aeruginosa is a Gram negative type of bacteriumand it is known for being prone to infect different sorts of tissues and organsinside the human body. In most cases, it affects individuals whose health iscompromised in different ways, so that is why most medical scientists refer toit as an opportunistic type of pathogen. The most common examples of suchclaims include burn patients who suffer from wound infections, cancer patientswho suffer from bacteriemia or neutropenia induced by hematologic malignanciesor chemotherapy, patients with a urinary catheter who suffer from urinary tractinfections and so on. In most of these cases the infections are categorized ashospital acquired. There are numerous different factors which may lead to thedevelopment of infections induced by Pseudomonas aeruginosa. The main problemwith this dreadful type of bacterium is that it may metabolize variousdifferent types of compounds which may be of great help when it comes togenerating significant amounts of energy. This is why Pseudomonasaeruginosa often contaminates disinfectants, intravenous solutions anddifferent items of hospital equipment and leads to development of epidemics with multiple numbers of patients who are infected by the same singlestrain of bacterium derived from the original source.
Treatment Options
The best treatment option for those who suffer from severecases of Pseudomonas aeruginosa infections includes the empirical therapybefore any tests are done. When a doctor suspects that some strain of Pseudomonasaeruginosa may be the main cause of severe infections, the empirical regimenconsisting of two different agents is the only way to avoid a catastrophe. Thedoctors need to be well informed about the patient’s previous exposure todifferent types of antibiotics and also about the local resistance patterns. Theappropriate choice of antibiotics should be very efficient when it comes tomaximizing the levels of serums so that the activity can be enhanced. Somecases may require the therapy to be slightly modified, mostly due to the factthat the emergence of resistance needs to be prevented and the energy needs tobe harnessed. The agents are commonly combined because as such they are muchmore effective in killing the harmful bacterium. The most frequently usedcombination of synergies of different agents include either an aminoglycosidecombined with an antipseudomonal beta lactam or a fluoroquinolone combined withan antipseudomonal extended spectrum penicillin. Combinations which involvedual beta lactams may sometimes be antagonistic and not that efficient. Thereare also certain isolates of Pseudomonas aeruginosa which are known for beingresistant to multiple antibiotics and those are considered as one of thebiggest challenges in the medical science. These are commonly resistant toantibiotics such as Ciprofloxacin, gentamicin, imipenem, ceftazidime andpiperacillin. This leads to the development of certain strains of this dreadfulbacterium which are actually resistant to all different types of antibioticscommonly used for the treatment of various infections. In such cases, physiciansneed to rely on a creative use of certain older agents such as colistine. Theseagents need to be administered intravenously and in some cases they may beassociated with certain unwanted side effects. Some cases may only be relievedby utilizing a surgical intervention which is focused on removing the nidus ofinfection.
Recommendations
As far as different recommendations go for those who sufferfrom severe infections triggered by the dreadful bacterium called Pseudomonalaeruginosa, there are several of them which can be made, but there stillremains a large amount of controversy surrounding them. As already explained,empirical therapy which combines two different types of agents characterized byvery potent antipseudomonal activity isthe best possible solution in the cases of infections where there is suspicionthat bacterium triggers them but the susceptibilities are still pending. It should be noted that the empirical therapyshould never involve any antimicrobial agents to which the patient has been exposedrecently. In cases of infections induced by Pseudomonal aeruginosa where thesusceptibilities are known, there is a wide array of monotherapy or combinationtherapy methods available for use. Two agents need to be used in cases when thepatients suffer from serious and life threatening infections such as sepsis,bacteremia in patients who are neutropenic, have infective endocarditis andnosocomial pneumonia. In such cases, the emergence of resistance may or may notbe prevented but the patient will most likely receive an agent to which thebacterium isolate may remain susceptible. There are also cases which can onlybe treated by a monotherapy, and they should never include the utilization ofmedications such as imipenem, fluoroquinolones and aminoglycosides. Combinationtherapy should never involve the use of dual beta lactam combinations asthey can be largely inefficient. Colistimethate may be considered toxic but itstill can be used in cases when the bacterium is thought to be multidrugresistant.













Your thoughts on this
Loading...